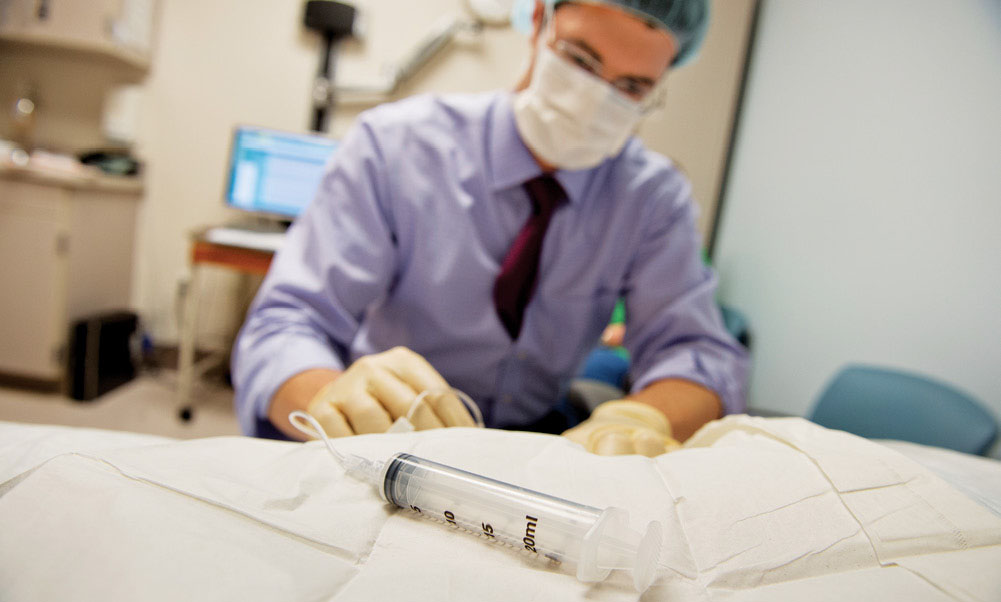
Relieving pain, reviving spirits
Clinic takes on patient suffering
Donald Tweet was running low on hope. Battling late-stage colon cancer was one thing, but the pain that accompanied it? That was almost impossible to endure.
By early 2014, Tweet was taking so much oral pain medication that the gregarious UPS driver could not get out of bed and was “totally out of it all the time,” his wife, Krystalon, recalls. And even at those high levels the morphine and Dilaudid brought little relief.
“It was horrible,” she says, “just horrible.”
But deliverance came last April when Tweet’s oncologist referred him to the UC Davis Cancer Pain Management and Supportive Care Clinic — and the clinic’s director, David Copenhaver.
Among other changes, Copenhaver recommended implantation of an intrathecal pump to deliver medication via catheter into Tweet’s spine and, thus, directly to his central nervous system. Dispensing the drug this way not only reduces the medication’s side effects but dramatically increases its potency as well.
Tweet passed away in early July at age 53, but the pump transformed his final weeks, allowing him to attend church, visit with friends, even ride his beloved motorcycle.
“It was a miracle,” his wife says. “It was the first time in two years that he actually found relief and was able to participate in life.”
For Copenhaver, Tweet’s experience illustrates the essence of his core clinical mission: to use all means possible to help patients manage cancer-related pain, thereby preserving quality of life.
It sounds like a no-brainer. But Copenhaver says pain management in cancer patients still rarely receives the specialized attention it deserves. The National Cancer Institute (NCI) agrees, reporting that despite the availability of a wide range of pain control therapies, undertreated cancer pain is a serious and neglected public health concern.
“We’ve become very accomplished at curing cancer and extending the quantity of life, but when it comes to the quality of life measures that are so important to patients, there are definitely gaps in care,” says Copenhaver, whose professional priorities were shaped by serving as caregiver to his grandfather, who suffered pain while battling multiple myeloma.
Statistics illustrating the incidence of pain afflicting cancer patients prove his point. Among those with advanced cancer, as many as 80 percent of patients report experiencing pain. For patients in active treatment and undergoing chemotherapy, up to 70 percent of patients experience pain.
Barriers to effective pain management are many, the NCI reports. Clinicians may lack expertise in assessing pain and prescribing suitable therapies, or may be concerned about side effects or patient addiction.
Patients, meanwhile, may be reluctant to report pain, fear side effects or feel concerned about being viewed as a “bad patient” or addict, especially in an era of rampant prescription drug abuse. The health- care system itself often hinders cancer pain management too, either through restrictive regulations, supply issues, or high costs coupled with low insurance reimbursements.
“The statistics show that we’re not doing enough to help patients manage pain,” Copenhaver says. “It’s no one’s fault, but as health professionals, we need to work together and tackle this because it’s a major issue.”
At the UC Davis Comprehensive Cancer Center, Copenhaver and his colleague Scott Fishman from the Division of Pain Medicine are working on multiple fronts. They now see patients at regular weekly clinics in the cancer center, as well as daily at their offices.
They are also reaching out to oncologists and others across the health system, emphasizing their availability to help and the importance of recognizing pain control as an integral aspect of cancer treatment.
Because cancer cases are complex, involving multiple diagnoses and side effects, the clinicians draw on a broad therapeutic repertoire. Copenhaver, board certified in anesthesiology and pain medicine, helps patients through the use of everything from the intrathecal pump to regional blocks and other injections, pharmacologic compounding to maximize relief, and a careful focus on nutrition and strategies to improve sleep.
Psychiatric and psychological interventions are another critical component, as mood plays a significant role in how patients experience and tolerate pain.
Copenhaver’s patients typically fall into one of three groups along a continuum — those undergoing active treatment and coping with side effects, those with advanced cancer facing the end of life, and a middle group of patients who have completed treatment and are left with residual pain, such as neuropathy.
This middle group, Copenhaver explains, has historically “fallen off the radar a bit,” with their pain often going undertreated. The NCI estimates that as many as one-third of patients will experience pain post-treatment.
“As we get better and better with our chemotherapy, we have more patients in remission, and survivors grow in number,” Copenhaver says. “But many are left with exquisite pain problems.”
Jeanna Smith, 29, is not scheduled for chemotherapy until later this year but is already battling intense pain related to her metastatic carcinoid cancer, which involves tumors in the gastrointestinal system. Smith, an emergency room nurse, says it varies from “aching to sharp, dull and stabbing pain so bad I can barely breathe.” She also suffers from nausea, vomiting and diarrhea.
With oral medications providing little relief, Smith was referred to Copenhaver, who “recognized right away that I had zero quality of life and needed to get my pain under control before my body was hammered with chemo.”
In late May, Copenhaver implanted an intrathecal pump. Roughly the size of a hockey puck, the battery-powered, programmable pump is surgically implanted in a patient’s abdomen. A catheter is then tunneled under the skin and inserted in the spine where the cerebrospinal fluid lives, and medication is delivered in a controlled stream according to each patient’s needs.
In addition to morphine, the pump can dispense local anesthetics and other medications to reduce pain and help with symptoms such as bowel dysfunction.
Smith says that while Copenhaver is still adjusting the drug dosage, the pump has already made a difference. Just as important, she says, is the comfort she draws from Copenhaver’s optimism.
“He is so positive, so reassuring and so obviously determined to do whatever it takes to help manage my pain,” Smith says. “He has been an absolute blessing. I truly, truly hit the jackpot when I got Dr. Copenhaver on my team.”
Tweet was among those patients who faced pain as cancer reaches its most advanced stage. At age 50 he underwent surgery to remove parts of his liver and stomach, and was treated with chemotherapy as well. Test results initially indicated that he was cancer-free, but last year he began experiencing stomach problems and other symptoms, and oncologists said there were no remaining surgical options.
What did remain was the pain, and Tweet was forced to consume ever greater quantities of pills to cope. Once an outgoing man who loved to socialize and build model airplanes, Tweet became crippled by his pain, virtually unable to function.
Then came the intrathecal pump and, gradually, Tweet’s curtain of pain began to lift.
“All I can say is, Dr. Copenhaver was a star,” Tweet’s widow says. “He even made house calls to adjust the dosage, if needed. He promised us he would ease my husband’s pain, and that’s what he did.”

