Living on the streets or in overcrowded homeless shelters makes it nearly impossible to stay healthy. Individuals in this situation are prone to extreme stress, compounded by exposure to communicable diseases, respiratory illnesses, the flu, hepatitis and more. Additionally, they contend with violence, malnutrition and harmful weather conditions, further exacerbating their circumstances.
“These patients are negatively impacted by social determinants of health and they are often in desperate need of care,” says Holly Kirkland-Kyhn, an assistant professor at the Betty Irene Moore School of Nursing at UC Davis.
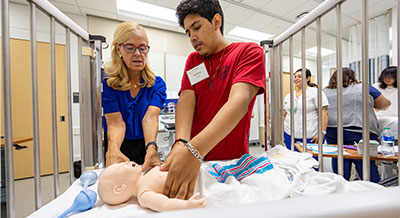
Kirkland-Kyhn is part of a team bringing that care to vulnerable populations thanks to the school’s new Integrative Nurse-Led Mobile Clinic project.
“Everyone deserves equitable health care,” says Deb Bakerjian, associate dean for practice. “Our goal is to prioritize the health care needs of these patients who come from very different backgrounds. This includes both their physical and mental health needs and requires our providers to use a person-centered, culturally sensitive approach to individualize care.”
The mobile aspect of care lies at the heart of the program, which is funded by a $4 million grant from the Health Resources & Services Administration (HRSA). HRSA defines mobile as “providers moving to where patients are.”
Kirkland-Kyhn is a nurse practitioner and has also led wound care at UC Davis Medical Center. Now, she sets her sites on boarding the van with the School of Nursing’s nursing and physician assistant students and nurse practitioner residents to take care into the community three times a week.
Immediate care and education for the future
Chronic health conditions like high blood pressure, diabetes and asthma worsen due to the lack of medications or a secure place to store them properly. Minor issues like cuts or common colds easily progress into more severe problems like infections or pneumonia.
“The best thing that nurses can do to be able to provide education and support for people, which is not really a medical model,” Kirkland- Kyhn explains. “Most people come to us to treat their wounds. But they also want us to teach them how to care for wounds themselves, or how to do CPR.”
The combination of poor health, heightened stress levels and unhealthy environments leads to frequent visits to emergency rooms and hospitalizations. By bringing care to those who need it, students learn the realties faced by these individuals before they encounter them in a hospital or clinic. Care on wheels comes in the form of a retrofitted van that carries care supplies for future patients and specially designed tents for the providers to provide care.
“We focus on people who are unhoused, are refugees, are from low socioeconomic circumstances or may be unaccompanied children,” Bakerjian says.
Increased access fosters health equity
Homeless individuals experience higher rates of illness and face a reduced life expectancy, dying up to 17 years earlier than the general population in the United States.
In 2021, the National Academy of Sciences, Engineering and Medicine (NASEM) released the Future of Nursing 2020-2030: Charting a Path to Achieve Health Equity. Authors emphasized the problems with access to care including the lack of insurance, inability to pay and lack of clinics or providers in local geographic areas. The nurse-led mobile clinic project follows report recommendations including expanding care through nurse-managed health centers.
“As an indispensable partner in the mission of UC Davis Health, we must work to improve access to care for underserved patients in the greater Sacramento region. Through our educational programs and community outreach, we work to fulfill our vision of optimal health and health care equity for all,” says Stephen Cavanagh, School of Nursing dean.
The overarching goal is to improve health outcomes and health equity for these underrepresented populations. It leverages the experience of UC Davis Health faculty and the School of Nursing’s partnerships with the Sacramento County Public Health Center. Kirkland- Kyhn works to partner with additional community organization who are already serving these populations and have established trust with them.
“When we partner with someone already in the community, we can prepare for our visit. Who’s been recently discharged? Who has specific needs? We can be ready to care for them when we arrive,” Kirkland-Kyhn says.
Care — and lessons in care — for the patients. Eye-opening experiential learning for the students.
“You’ve got to be a little bit of a politician to build trust and a little MacGyver to help,” explains Kirkland-Kyhn.
“Health care providers need to approach health care with humility,” Bakerjian adds. “It’s the interaction and relationships you develop with the people that are most important and the most effective.”