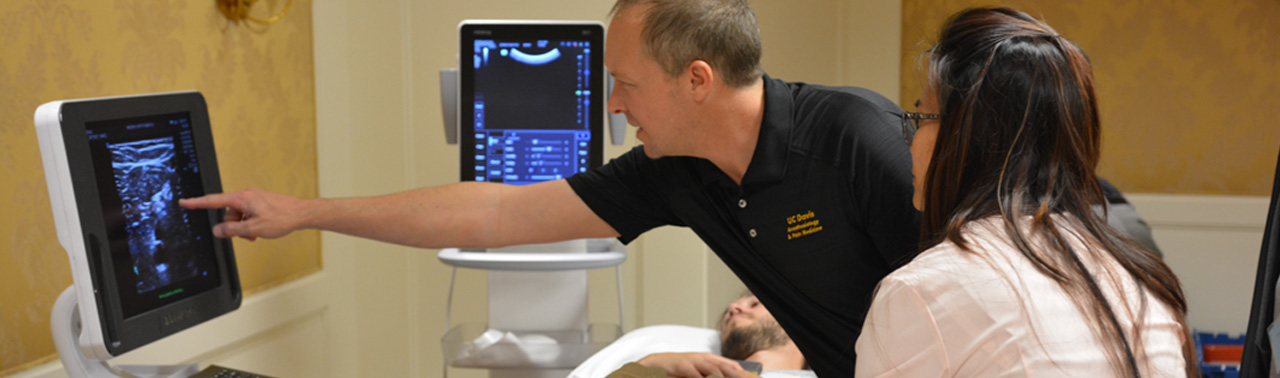
Welcome! Our ACGME- approved fellowship at UC Davis Medical Center provides the knowledge, skills, and experience required to become a perioperative consultant in regional anesthesia and acute pain management. Our fellow is fully involved in an expansive curriculum that involves advanced regional techniques, catheter placement, acute pain management, and clinical research.