A call for comprehensive care for children with spinal cord dysfunction
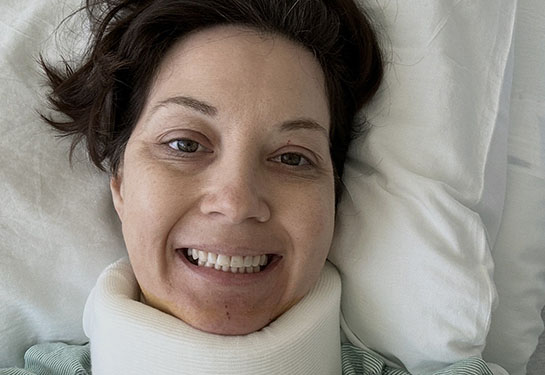
In this Q&A, UC Davis Health physical medicine and rehabilitation specialist Maya Evans shares important health information for clinicians and parents caring for children with spinal cord injuries and those with spinal cord dysfunction like spina bifida. Evans is an associate clinical professor at UC Davis Health and the medical director of the spina bifida program at Shriners Children’s Northern California. She co-wrote a review paper on spinal cord injuries with pediatric rehabilitation specialist Loren Davidson.
How common are spinal cord injuries in children in the United States?
About two out of every 100,000 children in the United States has a spinal cord injury. More than 95% of these cases are teens, with males outnumbering females by a ratio of 4:1.
What do families need to know when their child is diagnosed with a new spinal cord injury?
When a new spinal cord injury is diagnosed, one of the first questions families ask is whether the child will be able to walk. Engaging a pediatric physiatrist in this discussion will provide the best quality information and long-term care.
Children with spinal cord injury can benefit from acute inpatient rehabilitation. This is an intensive program that provides three hours of therapy, six days a week. The goal is to maximize patient function, educate caregivers, and assist with a successful transition to home and school. After discharge, outpatient therapies help with gaining developmentally appropriate skills.
One of the first questions families ask is whether the child will be able to walk. Engaging a pediatric physiatrist in this discussion will provide the best quality information and long-term care.”—Maya Evans
What are some clinical recommendations to take care of children with spinal cord injury or dysfunction?
In children born with spina bifida, care often starts with prenatal consultation. After delivery, care is ideally delivered at regular intervals through clinics with providers from different disciplines, including pediatric rehabilitation, urology, neurosurgery and orthopedics. Care coordination is a key function of these clinics.
These kids may develop spasticity during periods of rapid growth. This can be due to tethered cords that cause pain, deformity and limited functionality. A pediatric physiatrist can detect this early and coordinate a multidisciplinary effort to maintain function.
People with spina bifida, especially when they are infants, also need close monitoring for hydrocephalus. This condition can present with headaches, vomiting and seizures.
To maximize function and independence, it’s important that patients are referred to early intervention services and receive regular evaluations of therapy needs and school accommodations. These children may develop serious skin, renal and musculoskeletal conditions. They have a relatively higher risk of upper urinary tract disease, such as hydronephrosis. They also require frequent monitoring of renal and bladder function. For children with a neurogenic bladder, urinary tract infections are defined and treated differently.
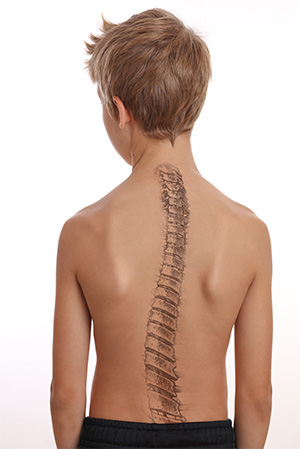
As for kids under 12 with an acquired spinal cord injury, around 90% of them develop scoliosis. Most will require surgery regardless of their injury level. In spina bifida, rapidly progressive scoliosis and back pain may indicate spinal cord tethering.
We also recommend prompt treatment for skin breakdown, a complication of loss of sensation in certain areas. This is done by removing all pressure from the affected area, optimizing nutrition, and providing proper wound care.
What are the treatment options for children with spinal cord dysfunction?
In spinal dysraphism, based on the type of neural defect, the child might need surgical treatment before or shortly after birth to prevent infection. It is estimated that 80% of kids with spina bifida would need ventriculoperitoneal shunts to drain excess fluid buildup in their brain. This percentage is decreasing, partly due to fetal surgery.
For acquired cases, neurologic recovery varies and depends on the injury type and severity. There are no approved therapies to regenerate the damaged spinal cord, and permanent neurologic issues are common and could impact future growth and development.
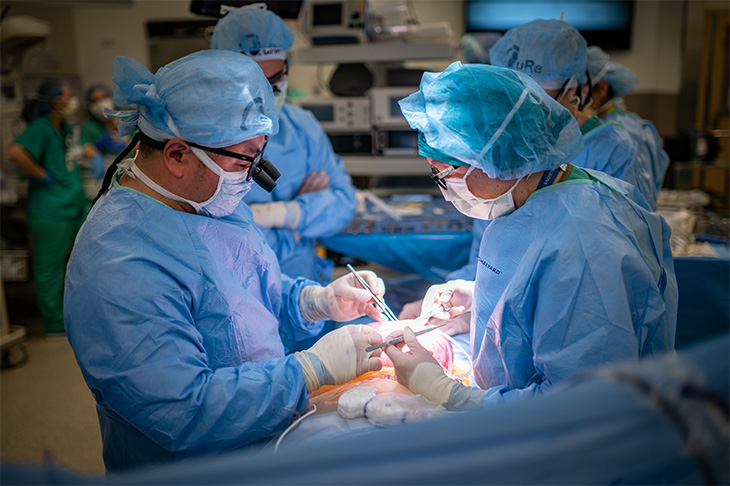
For example, spinal injuries caused by trauma may lead to vertebral instability and require surgical fusion. The surgery may stop the growth of the fused region and affect the height and mobility of the spine. If the injury is due to cancer affecting the spine, there may be a need for surgery and radiation, which might cause damage to the spinal cord. As for kids with spinal cord dysfunction due to infection, they are given treatment to fight inflammation and remove infection.
While there is no cure for spinal cord dysfunction, research is ongoing. The field of stem cell research continues to make strides in identifying potential restorative treatments. For example, research on the use of mesenchymal stem cells during intrauterine closure for spina bifida is underway.
Also, several exciting medical technology devices are in development, such as exoskeleton orthoses brain–machine interfaces, and limb reanimation through a variety of stimulation paradigms.
Can a child with spinal cord dysfunction live independently as an adult?
Teens with spina bifida typically have a delay of two to five years in acquiring self-care skills. Understanding this will help manage expectations, limit parent and teacher frustration, and set the teen up for success.
The ability of a child with spinal cord injury to live independently in adulthood and actively participate in the community depends on a variety of factors, including neurologic level of injury, socioeconomic resources and accessibility issues.
There are a variety of assistive devices, such as braces, walkers, crutches and manual and power wheelchairs. The child’s pediatric physiatrist and physical therapist will recommend developmentally appropriate devices to maximize independence and access while decreasing the potential for overuse injury. Power mobility may be needed if there is limited upper extremity strength or limited endurance. These devices are often very heavy and require a wheelchair-accessible van for transportation, which can significantly limit their utility.
Driving also improves community integration, odds of employment and life satisfaction. There are a variety of vehicle modifications that enable safe driving for individuals with lower and or upper extremity weakness. An occupational or physical therapist with additional certification as a driver rehabilitation specialist will determine what modifications are needed.
Read the review article: “Congenital and Acquired Spinal Cord Injury and Dysfunction,” published in Pediatric Clinics of North America.
Related readings:
- World’s first stem cell treatment for spina bifida delivered during fetal surgery
- CuRe trial highlighted in UC Davis podcast, Unfold
- First stem cell clinical trial for spina bifida treatment announced
- State stem cell agency funds clinical trial for spina bifida treatment
- Watch the Spina Bifida CuRe series (video)