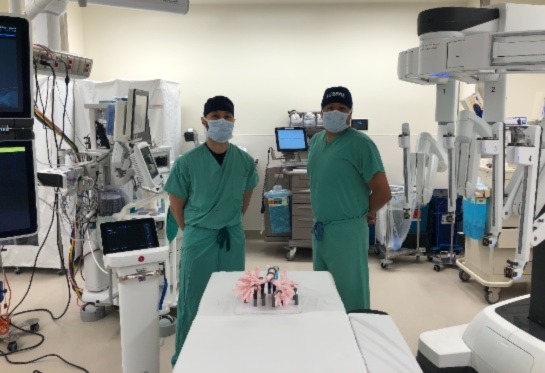
UC Davis Health performs first robotic-assisted bronchoscopy procedure
New robotic platform offers diagnosis and removal of lung cancer during single surgery
UC Davis Health physicians have performed the first single-anesthesia diagnosis to treatment of lung cancer using a fully robotic approach in the UC Health System.
The procedure, known as robotic-assisted bronchoscopy, allows for the diagnosis and removal of a lung cancer mass during one surgery. It reduces anxiety and unnecessary waiting time for patients.
Interventional Pulmonology is one of six specialties in which UC Davis Medical Center offers minimally invasive, robotic-assisted technology. Others include gastrointestinal, cardiothoracic, gynecologic oncology, otolaryngology and urologic surgery.
“Innovations such as the robotic bronchoscopy platform are patient care at the absolute highest level, from diagnosis to treatment with a multidisciplinary team approach,” said Bahareh Nejad, medical director of Robotic Surgery. “As we continue to grow the UC Davis Robotics Program, the institutional support we have received has been instrumental. We are excited to facilitate more growth with robotic surgery to make patient treatment better and more efficient.”
Streamlining patient care
Traditionally, when a patient is diagnosed with a suspicious nodule or mass in their lung, they are referred to a pulmonologist, who may perform a lung biopsy to confirm if it is cancerous.
If the lung nodule or mass is confirmed to be cancer, the patient may be referred to a thoracic surgeon, who determines if it can be surgically removed. If it can, the patient undergoes another procedure on a separate day that requires additional anesthesia. On average, patients may wait up to three months from the time a nodule or mass is first discovered to when they receive a diagnosis and treatment.
“Waiting months between a biopsy and a diagnosis can be an emotionally difficult and exhausting experience for patients,” said Chinh Phan, director of the UC Davis Interventional Pulmonology Program. “By utilizing the robotic-assisted bronchoscopy platform we can help reduce the anxiety and unnecessary waiting times that patients traditionally experience.”
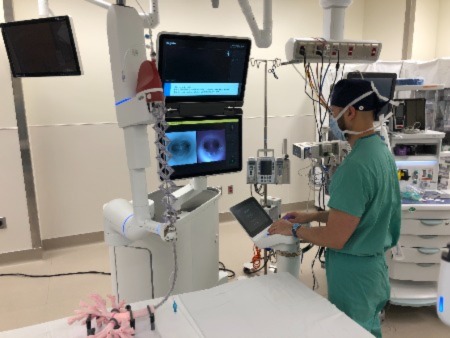
The robotic-assisted bronchoscopy procedure utilizes the Ion Endoluminal Platform by Intuitive. The high-tech system creates a 3D map of the patient’s lungs using a CT scan. The software then generates the safest and most efficient route through the lung to the nodule or mass. Once the route is determined, an ultrathin and ultra-maneuverable catheter is guided to the site of the lung nodule or mass, where it is marked and biopsied with precision and stability. Lymph nodes are also biopsied during the same procedure, using endobronchial ultrasound. The samples are then evaluated on-site.
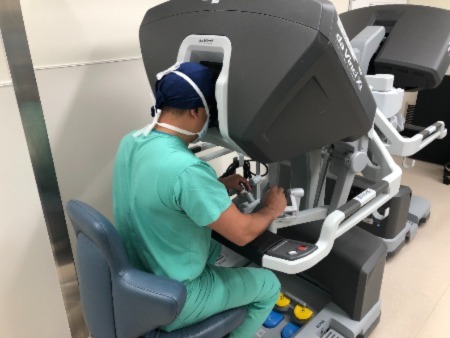
If the lung nodule is determined to be an early-stage cancer, the surgical team uses the same navigational route to mark the area with dye to prepare for its removal. Then, the patient, still asleep, has a second robotic procedure to remove the lung cancer on the same day.
Recently, the UC Davis Health team identified a 1.5 cm pulmonary nodule in the right upper lobe of a patient’s lung, performed a biopsy, identified malignant cells from rapid on-site evaluation, and injected an inert dye for marking, all within 45 minutes. Surgeon Luis Godoy subsequently used the Da Vinci Robotic System by Intuitive to safely resect the lung cancer. The patient was discharged home 24 hours after being diagnosed and cured of lung cancer.
"With these two robotic technologies, we now have the ability to diagnose and treat suspected early-stage lung cancer patients in one anesthetic event,” explained Phan. “To put it into perspective, the National Comprehensive Cancer Network guidelines for time from diagnosis to surgical treatment of lung cancer is eight weeks; we have set a new standard for innovative and efficient patient care.”
Waiting months between a biopsy and a diagnosis can be an emotionally difficult and exhausting experience for patients. By utilizing the robotic-assisted bronchoscopy platform we can help reduce the anxiety and unnecessary waiting times that patients traditionally experience.”—Chinh Phan
Shift in preventative screening
Lung cancer is the leading cause of cancer-related death in the United States among men and women, making up almost a quarter of all cancer mortalities. It is a malignancy that tends to spread quickly, shows no symptoms unless it is very advanced, and can silently spread to virtually any part of the body. This makes early screening and treatment critical.
In 2021, the United States Preventive Services Task Force updated its lung cancer screening guidelines, making more people than ever eligible. The new guidelines recommend annual screening in adults aged 50 to 80 years who have a 20 pack-year smoking history and currently smoke or have quit within the past 15 years. By some estimates, 14.5 million Americans are now candidates for screening — an increase of 6.5 million people, including more high-risk women, and Black and Hispanic smokers, who were previously underrepresented in screened populations.
“The most effective method for treating cancer is to catch it early and to start treatment as soon as possible,” explained Phan. “With these news screening guidelines and our robotic-assisted bronchoscopy platform, we are introducing a paradigm shift in lung cancer treatment that will further advance health equity for our community and others.”
Collaboration and looking forward
The robotic bronchoscopy program is a multidisciplinary collaboration. It includes operating room staff, the anesthesia and pathology teams and leadership, who provided the necessary tools and facility space to deliver the best care possible.
“We would not have been able to implement this innovative platform without the commitment of everyone involved and I am thankful to all who contributed to this milestone achievement,” said Phan. “Our health system is now equipped to help patients detect and defeat lung cancer earlier.”
Moving forward, the UC Davis Interventional Pulmonology Program has already implemented strategies of growth in their integrated service lines and plans to implement their comprehensive anesthetic diagnosis, staging, and lobectomy into additional treatment programs.