Guide to pediatric inflammatory bowel disease
Download the PDF of our “Patient Information Guide: Inflammatory Bowel Disease Program”
This guide includes helpful information and planning tools, a food journal tracking sheet and a patient transition checklist.
Understanding Inflammatory Bowel Disease
Basic knowledge about inflammatory bowel disease (IBD) will help you better understand your or your child’s disease and – more importantly – help you recognize symptoms to help manage the condition.
What is IBD?
We encourage you to ask questions and be an active part of your or your child’s care team.
IBD is a chronic inflammation or irritation of the intestines that is not due to infection. In patients with IBD, the immune system overreacts and causes injury to the intestines.
There are two main types of IBD: Crohn’s disease and ulcerative colitis. Crohn’s disease can involve any part of the intestine from mouth to bottom. Ulcerative colitis usually involves only the large intestine (colon).
It is important not to confuse IBD with irritable bowel syndrome (IBS). Although the symptoms of IBS are sometimes similar to those of IBD, the disorders have very different causes and treatments.
Who gets IBD?
It is estimated that over one million Americans – children and adults alike – suffer from IBD. Males and females are affected about equally.
What causes IBD?
IBD is thought to be caused by a combination of both genetic and environmental factors that lead to injury of the intestines. There is a lot of research underway to better understand IBD.
What are the symptoms?
Signs and symptoms of IBD may include:
- Abdominal pain
- Diarrhea or bloody bowel movements
- Weight loss or poor growth
- Fatigue/decreased energy level
- Unexplained fevers, joint pain or mouth sores
- Anemia (low red blood cell count)
If you are experiencing a flare
Even with medical treatment, a person with IBD can experience a flare – an episode when symptoms reappear. It is important that you report your or your child’s symptoms early so your doctor can provide the best treatment. This may help you stay well and prevent some of the complications related to IBD.
Symptoms of a flare
Avoiding a flare is better than treating a flare. Taking your medications as directed can help control your symptoms and help to avoid a flare.
Alarm symptoms may include:
- Abdominal pain
- Blood in bowel movements
- Diarrhea/increased bowel movements
- Nausea/vomiting
- Fevers
- Joint pain
- Fatigue
- Change in appetite
What to do
Call your doctor at the onset of any symptoms of a flare. Please call 916-734-3750 on weekdays before 4:30 p.m. or 916-734-2011 after hours, weekends and holidays to speak with the on-call physician.
- Identify the flare symptoms
- Know what medications you or your child are taking and the doses
- Take your medications consistently and as prescribed
We will perform certain tests to diagnosis IBD, as well as to help us understand what parts of your or your child’s body are affected, and to develop the best treatment plan. We also test for any possible flare and to watch for side effects of any medications you of your child may be taking.
We will complete a comprehensive initial evaluation and monitor your or your child’s response to treatment. We will provide you with a complete explanation of any test results and answer any questions you may have.
It is important that you understand why these tests are being done, complete blood work or other tests as requested and keep all follow-up appointments to ensure your or your child’s health progresses.
Tests may include:
Esophagogastroduodenoscopy (EGD)
An EGD examines the lining of the esophagus, stomach and duodenum (the first part of the small intestine). The exam is done with a flexible tube called a scope, which has a light and a camera on the end. The doctor will look for redness, swelling, bleeding, ulcers or infections. Small tissue samples called biopsies will be collected and observed under a microscope.
Colonoscopy
A colonoscopy examines the entire colon (large intestine). A scope with a light and camera on the end will be used for the test. The doctor will look for redness, swelling, bleeding ulcers or infections of the bowel wall and collect biopsies for observation under a microscope.
It is normal to feel nervous about these procedures. The procedures are done under anesthesia so that you or your child will generally not feel anything or remember the procedure. The goal is to gain a better understanding of your or your child’s disease as safely and comfortably as possible.
You will be given important information to follow before and after one of these procedures. If you have any questions, please call our clinic or send an electronic message to your or your child’s nurse or physician through MyUCDavis Health (MyChart®).
Some general items to keep in mind when having an EGD or colonoscopy include:
- You or your child should not eat or drink for several hours before the procedure. This may include red and purple liquids and certain medications such as aspirin and ibuprofen (e.g. Advil, Motrin, etc.).
- The day before a colonoscopy, you or your child will be asked to undergo a “cleanout” to clear the colon and ensure a successful procedure. You or your child must adhere to a strict diet for at least the day prior to the procedure. You will also be given medications to take to help with the cleanout process. This will be explained in detail prior to the procedure.
- Most procedures are same-day, meaning that after you or your child wake up from the sedation or anesthesia, you can go home.
- Following these procedures, you or your child may experience some bloating, abdominal cramping or pain, nausea, sore throat, or some blood in bowel movements. If you or your child has continued blood in bowel movements, worsening abdominal pain, high fever or vomiting, contact your doctor or the on-call physician immediately.
Blood work
Blood tests are done on a regular basis to monitor the disease activity and the effects of medications. Some common blood tests include:
- Complete blood cell count (CBC) for anemia (low red blood cell count), signs of infection, or potential side effects of medications
- Liver enzymes (AST and ALT) for potential side effects of medications or complications
- Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) for inflammation
Stool studies
When having symptoms of a flare, stool (bowel movement) studies may be done to check for infections or inflammation.
Radiology studies
These tests help to look for inflammation and check for complications. Examples of radiology studies include CT scan, MRI and upper GI series. Your doctor or healthcare provider will explain these to you in more detail if they are needed.
PillCam®
A capsule endoscopy, also known as PillCam®, observes the esophagus, stomach and small intestine. The procedure involves swallowing a capsule the size of a large vitamin pill. The capsule includes a camera that sends pictures of the intestines to a recorder on your or your child’s waist. The recorder will be collected approximately eight hours after the capsule is swallowed and the pictures will be reviewed. The PillCam® is disposable and will naturally pass in a bowel movement.
We will work with you to develop a comprehensive, personalized treatment plan for you or your child. We will help you understand the treatments available and value your input on which options you or your family prefer. We encourage you to ask questions if and when concerns arise.
Taking medication as prescribed is extremely important. Missing a dose means the medication may not help as intended, while taking too much can be harmful. There can be side effects from some medicines that we monitor for with routine blood tests and physical exams.
Let us know if you have any concerns or if you or your child have any problems or side effects with any prescribed medications or treatments. Tell us if you or your child are taking medicines other than those prescribed by your UC Davis Children’s Hospital doctor, including any herbal or alternative medicines or supplements.
Medications
Listed below are the most common medications used to treat IBD in children, teens and young adults. Information on non-medication therapies such as nutritional support is also provided. Before starting any treatments, please discuss it with your or your child’s care team.
Prednisone
Prednisone is a medicine known as a corticosteroid. It is similar to hormones made by the body and helps to reduce inflammation. Prednisone may slow down the body’s natural production of these hormones. Because of this, it is important to take the medicine as prescribed and to slowly decrease the medicine as directed. Do not stop it without talking to your doctor.
Side effects of prednisone can include weight gain, hunger and changes in mood and sleep patterns. These usually improve as the dose is lowered. Other side effects can include weakening of the bones, increased risk of infections, high blood pressure, high blood sugar and stomach irritation. Patients who take prednisone or other corticosteroids should be current on vaccines, undergo regular eye exams and may need to have bone density tests.
Mesalamine
Mesalamine is an aspirin-like medicine that can be taken by mouth or given by suppository or enema. These medicines include the brand names Asacol, Colazal, Pentasa, Canasa, Lialda, Apriso and Rowasa. Rare side effects of these medications include allergic reactions, pancreatitis and kidney injury. Those who take mesalamine should wear sunscreen to reduce the risk of skin rashes and sunburns.
6-mercaptopurine (6MP)/Azathioprine
These medications act as an immunosuppressant. Suppressing the immune system reduces inflammation in the GI tract. These medications do not work right away, so you or your child may need to be on a combination of medications at first. Regular blood tests will check for possible side effects, including low white blood count and irritation of the liver or pancreas. Patients taking these medications should be cautious about their amount of sun exposure. They are also at a small increased risk for lymphoma (a tumor of the lymph glands) compared to the average person.
Methotrexate
Methotrexate is another immunosuppressant. It can be taken by mouth given via injection. Blood tests will be done often to check for potential side effects such as irritation of the liver and low white blood cell count. There is also a small risk of lymphoma. Pregnant women or women planning to become pregnant should not take this medication.
Anti-tumor necrosis factor medications
These medicines include Remicade, Humira and Cimzia. They block the action of a protein in the body called TNF-alpha (tumor necrosis factor) made by the body’s immune system. People with IBD may produce too much TNF-alpha which can cause inflammation. Remicade is given as an IV infusion and takes about three hours to infuse. The frequency of the infusions depends on symptoms, but it is usually given every eight weeks. Humira is given by injection every two weeks, and Cimzia is given by injection every month. Before receiving any of these medications, your doctor will test for tuberculosis. Regular blood tests will monitor for possible side effects, including low white blood cell count, irritation of the liver, infections such as tuberculosis and a small increased risk of lymphoma.
Other treatment options
Although treatment with medication is the first option for patients with IBD, some patients may require surgery. Surgery may be needed to address serious IBD complications, or for disease that has not responded to medications. Surgical options are discussed further in later in this handbook.
A total or partial liquid diet is another treatment option for IBD. This may include a liquid diet by mouth, by a nasogastric tube (a tube that delivers the formula directly into the stomach) or naso-jejunal tube (a tube that delivers the formula directly into the intestine.) This type of therapy has been shown to be a safe and successful option in place of medication. More information about diet and nutrition is also discussed later in this handbook.
Adherence means how well you or your child follows the medical advice given (for example, taking medicine, making diet changes, exercise, etc.). Good adherence is one of the best ways to stay healthy and symptom-free.
Taking your medications is particularly important. Studies have shown that patients who do not take their medications have a 30 to 40 percent greater chance of experiencing a flare of their disease.
Many medications can be taken once or twice daily, but certain medications need to be taken more often. With medications that need to be taken more often, talk to your or your child’s doctor about trying to simplify the schedule. We know that with school, work, sports and other activities it can be easy to forget or miss a dose – this is more common than you might think.
We encourage you to talk openly with your care team about any problems or concerns with the prescribed medications. We understand that you are doing your best to manage your condition according to your or your child’s age and ability. Our aim is to provide you with clear and simple instructions on how to take care of yourself or your child, including taking medications and eating the right diet.
Let us know when you have difficulties following the recommended care plan or diet so that we can help. Be sure to take medications as prescribed and request refills in a timely manner.
Helpful hints
- Set an alarm on your cell phone or watch as a reminder to take or administer medication
- Look up www.mymedschedule.com, a website that can send reminder text or e-mail alerts
- Keep medications where you can see them (e.g. next to your toothbrush or in the kitchen) and include them as part of your daily routine (fit them into your life instead of rearranging your life around them)
- Leave a reminder on the refrigerator or bathroom mirror, on a calendar or in a daily planner
- Keep a medication journal or chart and check off when you take or administer each dose
- Use pill boxes and count out medications for the whole week to help you stay organized
- Ask for help from family members to remind you to take or administer medications (your child can take on more responsibility as they get older, but should recognize when they need help and ask for it)
Medications are typically the first therapy for IBD and many patients respond well to medical therapy. However, surgery may be needed if serious complications from IBD develop (see below) or if medications are unable to control symptoms.
Complications of IBD that may require surgery include:
- Intestinal obstruction (blockage in the intestine)
- Uncontrollable bleeding
- Stricture formation (narrowing of a section of the intestine)
- Perforation of the intestine (tear or hole in the intestine)
- Formation of a fistula (abnormal connection from the intestine to another part of the body) or abscess (collection of pus and inflammation)
- Toxic megacolon (bacteria and gas build up in the intestine causing it to become dilated or stretched out)
If surgery is the right option for you or your child, be aware of any warning signs or symptoms following the surgical procedure. These will be discussed with you before and after your or your child’s surgery and we encourage you to ask questions. If any symptoms occur following the surgery, and call your care team immediately.
Our team is up-to-date on the latest surgical treatments for IBD. If surgery is required, we will explain the options available to you or your child and answer any questions you may have. We can also put you in touch with other patients and families who have undergone surgery for IBD as additional resources.
The following are some of the most common surgical treatments for IBD. Before any of these procedures are performed, discuss the benefits and risks of the surgery with your or your child’s IBD and surgery team.
Common procedures for ulcerative colitis:
Proctocolectomy with ileostomy
In this procedure, the colon and rectum are removed (proctocolectomy). A surgically created hole in the abdomen (ileostomy) is made for the removal of stool. After this procedure, an external bag is worn over the hole to collect stool. The ileostomy can be permanent or temporary. Newer surgical techniques have eliminated the need for a permanent ileostomy for many patients.
Proctocolectomy with ileal pouch-anal anastomosis (IPAA)
This procedure is performed in two or three stages. The colon and rectum are removed and a temporary ileostomy (surgically created hole in the abdomen) is made. The ileum (end of the small intestine) is then made into a pouch and connected to the anus. The ileostomy is closed once the pouch has healed. Pouchitis (inflammation of this newly formed pouch) is a common complication of this procedure, occurring in up to half of patients, and usually in the first one to two years after surgery. Symptoms include, but are not limited to, diarrhea, bloody bowel movements or abdominal pain. This condition can usually be treated with antibiotics.
Common procedures for Crohn’s disease:
Strictureplasty
This procedure widens a narrowed or tight area of the intestine, and prevents the removal of a section of the intestine. It is most effective in the lower parts of the small intestine (jejunum and ileum).
Intestinal resection
In this procedure, a section of unhealthy intestine is removed (resection) and the two ends of healthy intestine are joined together (anastomosis). Unfortunately, IBD can reappear at or near the area that was joined together.
Proctocolectomy with ileostomy
As with ulcerative colitis, this procedure is an option for patients who have severe Crohn’s disease that affects their colon. In this procedure, the colon and rectum are removed (proctocolectomy). A surgically created hole in the abdomen (ileostomy) is made for the removal of stool. After this procedure, an external bag is worn over the hole to collect stool. The ileostomy can be permanent or temporary. Newer surgical techniques have eliminated the need for a permanent ileostomy for many patients.
Good nutrition is an important tool to manage IBD as it supports health, growth and bone strength. It is important to discuss your or your child’s diet with the dietitian. They can offer ideas about how to track progress; however, it will be up to you to improve your or your child’s eating habits. Some diets or supplements may interfere with IBD medications or may not be appropriate for you or your child.
Our dietitians will help teach you about nutrition and IBD. You or your child will meet with a dietitian every year (or more often if needed) to monitor growth and make recommendations to improve your or your child’s health through nutritional changes, or refer you to a growth specialist if needed.
We encourage you to be open and honest about your or your child’s eating habits, to ask questions and work with your dietitian to establish nutrition goals. You will also monitor your or your child’s height and weight on a growth chart.
Why nutrition is important
Good nutrition is important in the management of IBD. There are many causes of poor nutrition in children and teens with IBD, such as eating less because of a poor appetite or cramping. The body needs more calories to repair the damage of inflammation, but the intestinal tract may not be able to absorb nutrients properly during a flare.
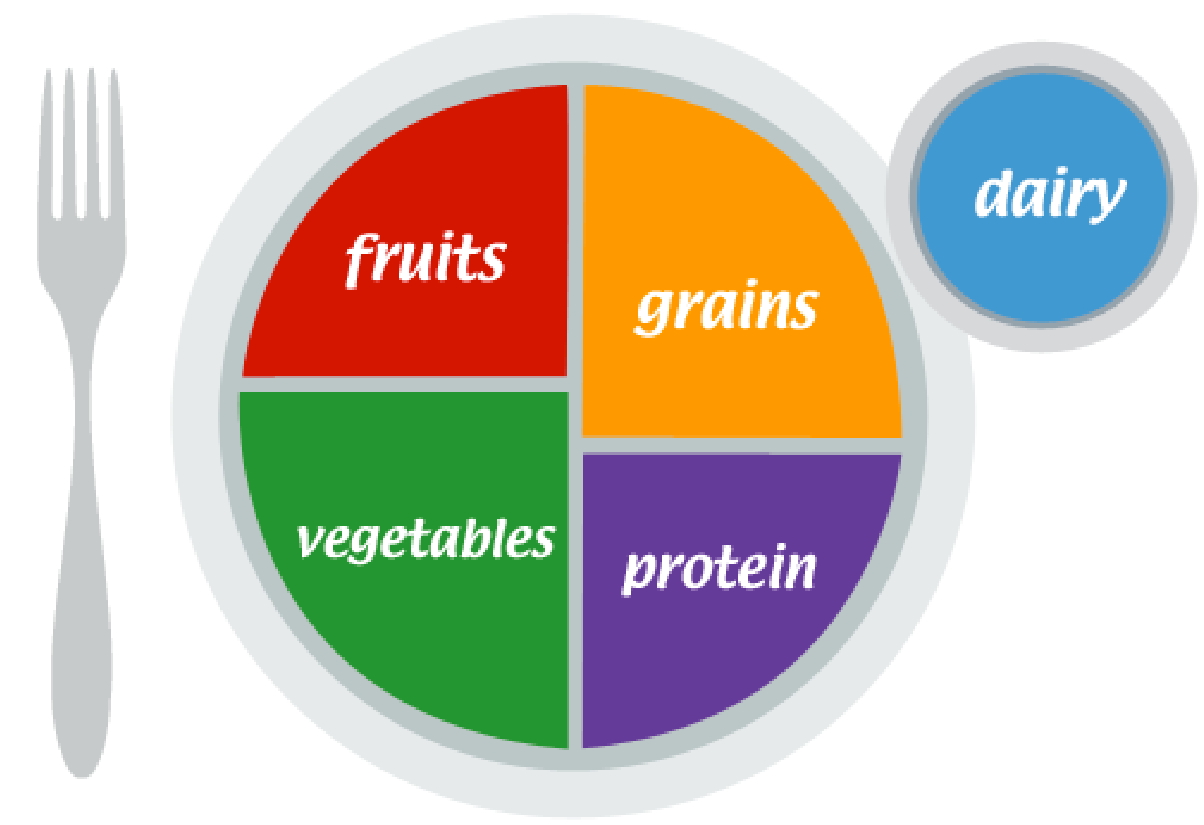
MyPlate is the preferred model of good nutrition. It uses a dinner plate to illustrate the five food groups that are the building blocks for a healthy diet – vegetables, fruits, grains, protein and dairy.
Visit the MyPlate website at myplate.gov for a daily checklist, tracking tools, quizzes, recipes, tips and more information. Recommendations for physical activity and explanation of benefits are also included.
Which foods are important
Children and adolescents grow quickly and need well-balanced nutrition. Protein is important for healing and repairing body tissues. Fat is a very concentrated calorie source that can add calories when your appetite is low and you are eating less. Carbohydrates are the main energy source for the body and, if eaten in appropriate amounts, can help protein repair body tissue.
For patients with IBD, water is especially important during bouts of diarrhea. Drink more water if you have diarrhea to prevent dehydration. An increased amount of protein and water are needed to combat inflammation.
Special diets
It is a myth that there are foods that can cause, fix or cure IBD. There is no evidence that any food or diet can trigger a flare or cause a remission and many claims have not been medically proven. Some diets, if under medical supervision, may be safe; therefore, it is important to discuss any possible changes with your doctor and dietitian.
It is especially important not to automatically remove foods or entire food groups from your diet to try to prevent symptoms of cramping or diarrhea. A food journal is useful to determine food intolerances. If some food groups are taken out of the diet completely, vitamin or mineral deficiencies occur.
There may be specific times when monitoring intake of certain foods may be useful:
- After surgery or if the intestine is narrowed by inflammation, foods that are high in fiber may cause pain and block the intestine. A low-fiber diet may be helpful until the inflammation has improved. Your doctor or dietitian will let you know if you or your child should follow a low-fiber diet.
- Salt intake should be monitored while on corticosteroids. Salt increases fluid retention and causes swelling, a side effect of steroids.
- Some people may not tolerate milk or other dairy products. This is usually a temporary problem. Dairy products are a great source of protein, calcium and vitamin D, and should only be restricted if they cause problems.
All dietary changes should be discussed with a dietitian to ensure that you or your child are still getting the right amount of nutrients. During a period of inflammation, a diet high in calories and protein, particularly from meat and dairy, may be helpful to combat weight loss or feeling tired.
Liquid diets or supplements
For patients having difficulty eating, liquid supplements can be useful. These liquids may need to be given with a temporary feeding tube to provide the calories needed to ensure growth.
Your doctor may discuss a treatment option that involves using liquid supplements as the primary or only source of nutrition. The use of total or partial liquid diets has been researched in several studies. Total or partial liquid diets may be as effective as using steroids, may improve growth and may be effective in preventing flares of IBD. If you are interested in this type of nutrition treatment, ask your doctor and dietitian for more information.
Vitamins and minerals
Vitamins and minerals are important for bodies to work properly and perform daily tasks. Absorption of some vitamins and minerals may be affected by IBD and may need to be increased during times of inflammation.
Calcium
Research has shown that individuals with IBD are at risk for osteoporosis (a condition that leads to thin, weak bones). This may happen for several reasons including decreased amounts of calcium and vitamin D due to not eating or drinking enough dairy products, improper intestinal absorption and/or long-term steroid therapy.
Steroids may interfere with the body’s ability to absorb calcium. Eating the recommended amounts of dairy products and/or taking vitamin and mineral supplements can help prevent weak bones.
Vitamin D
Vitamin D deficiency is common in patients with IBD, even when the disease is in remission. It is unclear exactly why this is so common, but it may be caused by a combination of low vitamin D intake, poor absorption of vitamin D and decreased time spent outdoors. Just like calcium deficiency, vitamin D deficiency can be associated with increased risk of osteoporosis. Your doctor may check your or your child’s vitamin D levels with a blood test and may recommend supplements if needed.
Folic acid
Folic acid deficiency can occur because of decreased appetite or decreased intake of foods containing folic acid, or because certain medications can interfere with its absorption. Meats, breads and cereals, and dark green leafy vegetables are high in folic acid.
Iron
Iron deficiency can occur due to ongoing blood loss from the intestines and can lead to anemia, which can cause fatigue or weakness. Increasing foods rich in iron is important. These foods include meats, fortified breads and cereals, and some fruits and vegetables like raisins, spinach and bananas. Blood tests for anemia and may indicate the need for an additional iron supplement. Iron supplements work best when taken with vitamin C, such as a glass of orange juice.
Multivitamins
Since eating less and intestinal inflammation may reduce the intake and absorption of other vitamins and minerals, a complete multivitamin and mineral supplement is usually recommended. Each multivitamin and mineral supplement is different. Check the label to make sure that the key vitamins and minerals are included (vitamin D, calcium, folic acid, zinc and iron) and that most of each of the nutrients in the supplement supply 100 percent of recommended amounts
Complementary and alternative medicine (CAM)
Surveys have reported that anywhere from 21 to 68 percent of patients with gastrointestinal diseases have used some method of complementary and alternative medicine, including herbs, fish oil and probiotics. There is limited information on the short and long term effects of these therapies, as well as limited scientific evidence on their safety and efficacy. It is important to speak with your doctor and dietitian about any herbal supplements you or your child currently take or are thinking about using. Some herbs may interact with medications or may worsen IBD symptoms so it is important to discuss all additional medicine practices with the care team.
There are some substances that may help treat the symptoms of IBD:
Fish oil
Fish oil has anti-inflammatory properties and has been proven to be effective in the treatment of a number of inflammatory diseases. There have been several studies using fish oil in adults with IBD with varying results. The research is ongoing. Until recommendations are established, it may be helpful to eat two servings of fish per week for good heart health.
Probiotics
Probiotics are microorganisms present in the gastrointestinal tract that may benefit certain health conditions. Research has shown promise in the use of probiotics with ulcerative colitis and pouchitis; less so for Crohn’s disease. So far probiotics appear to be safe; however, it can be difficult to find a supplement source with live bacteria. Therefore, it may be beneficial to eat yogurt (if tolerated) for the probiotic bacteria and a good source of protein and calcium.
Other diets and supplements
You may come across information about other special diets from people you know or online. For example, the soothing properties of aloe and coconut oil have been suggested as helpful in alleviating symptoms of IBD. Most recently, a semi-vegetarian diet has been found to be potentially helpful for patients with Crohn’s disease. Before starting any special type of diet, you should discuss this with your health care provider. Also, start only one new thing at a time. This makes it easier to identify any benefits or potential side effects.
We are committed to helping our patients learn the skills needed to take care of their own medical needs as adults. We will continue to work with you or your child when transitioning to adult and self-care is appropriate.
Responsibilities and expectations
When we talk about self-management and transition, we are talking about the process of you or your child learning to be independent and self-sufficient in care.
Some adolescents with IBD will switch from a pediatric gastroenterologist to an adult gastroenterologist. Patients who continue to see their pediatric specialist will need to switch from dependence on parents or caretakers to independent self-management.
Making the transition to self-care can be difficult. It is a long-term process taking anywhere from several months to more than one year; it does not happen overnight. It is important that this process is started when you or your child are ready.
What to know for successful self-management
Key topics for successful transition to self-management include:
Knowledge
- Disease
- Medications (name, dose, purpose, side effects)
- Laboratory and radiology tests
Independence and assertiveness
- Independent health behaviors (responsible for medications and office visits)
- Self-advocacy (speaking up for yourself at school or work)
- Insurance issues
Lifestyle
- Effects of smoking and alcohol
- Consequences of not taking medications
- Fertility and sexuality
The age at which these topics are discussed depends on maturity level and support system. These topics and any questions you or your child may have should be discussed openly with your doctor.
Resources for transitioning to self-management
A transition checklist is included in the Patient Information Guide (PDF). Please answer each item on the checklist by placing a check mark under the column on the right side that indicates whether you or your child can do the task by yourself, with some help from others, or cannot do or need lots of help from others.
There are no right or wrong answers. The answers will help us identify what we can do to help you or your child better manage your or their care. The checklist can be updated regularly until you or your child are able to check the “I can do this by myself” columns for all items.
Download the Patient Information Guide: Inflammatory Bowel Disease Program (PDF)



