Residency Program - Case of the Month
December 2011 - Presented by Meighan Tomic, M.D.
Answer:
Adrenal Myelolipoma
Histological description:
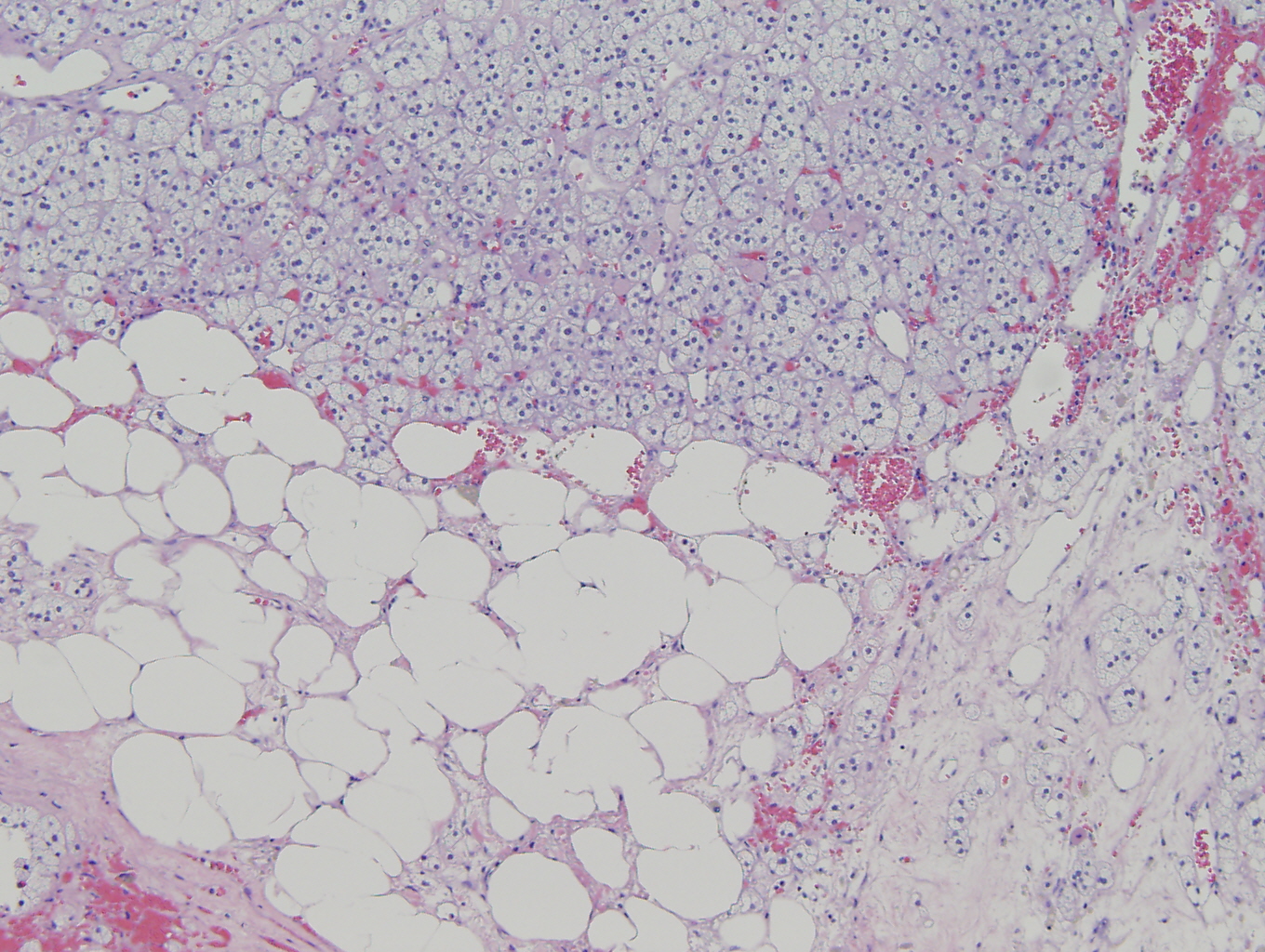
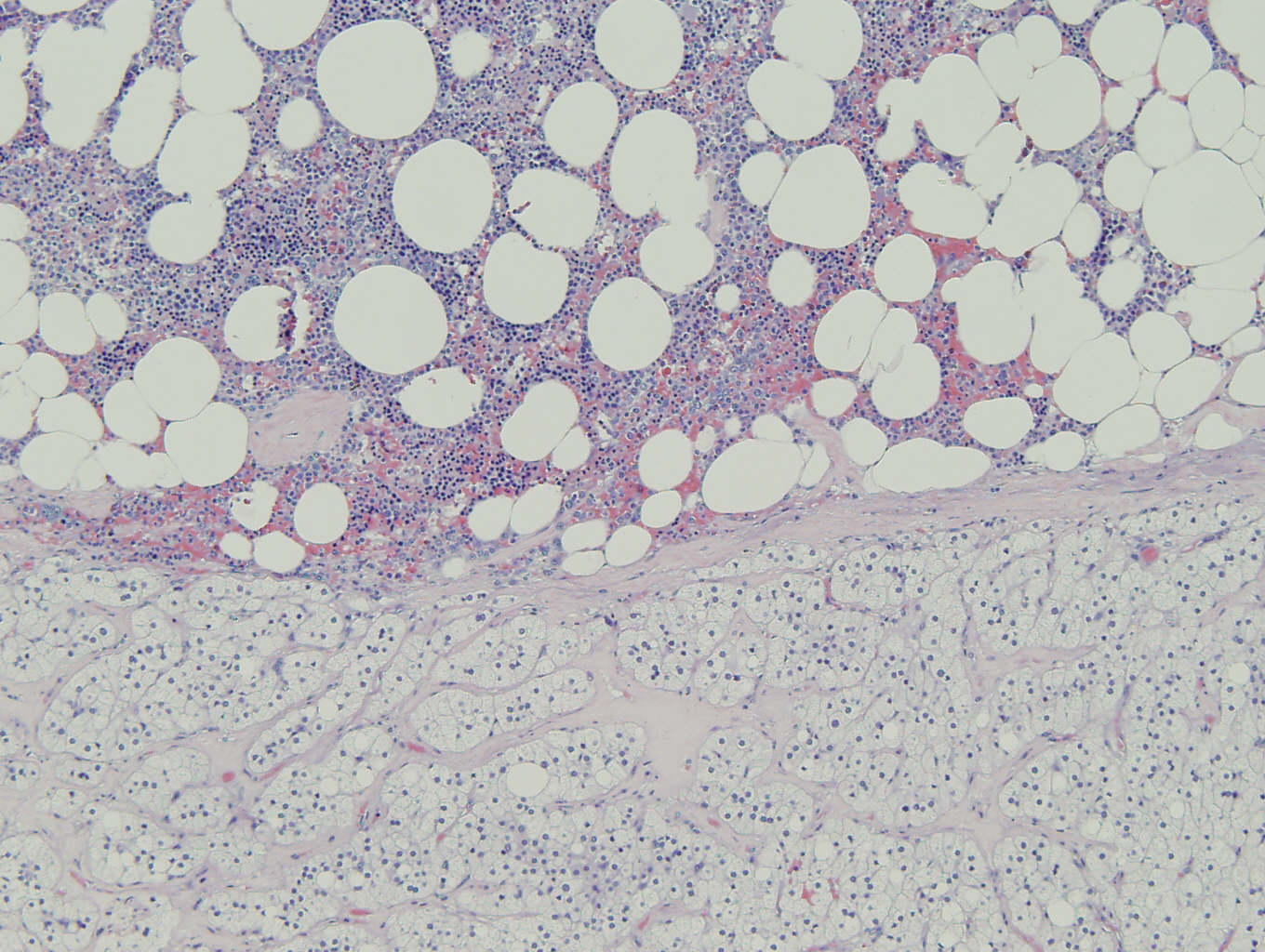
Microscopically the tumor was comprised predominately of normal adrenal cortical parenchyma with areas of cystic degeneration. The diagnosis of myelolipoma was made by identifying foci of mature adipose tissue and hematopoietic elements. The hematopoietic elements showed trilineal hematopoiesis with no increase in immature elements or evidence of dysplasia.
Discussion:
Myelolipomas are rare benign lesions comprised of mature adipose tissue admixed with hematopoietic elements (1). They are typically found in the adrenal gland; however extra adrenal sites, such as the mediastinum, have also been reported (2). Autopsy studies indicate an incidence of 0.08% to 2.0% (3-5). Ante-mortem diagnosis usually represents an incidental radiological finding. Identification of the fatty component suggests the diagnosis radiologically (6). Occasionally patients present with abdominal pain or a palpable mass. Retroperitoneal hemorrhage, in the setting of rupture of a large mass, is a rare but significant sequela. Myelolipomas are hormonally inactive. Unlike other types of extramedullary hematopoiesis, an association between myelolipomas and altered bone marrow function has not been identified.
These lesions range in size from microscopic foci to 40 cm (1-9). Grossly they are comprised of yellow areas, consistent with adipose tissue and residual cortical parenchyma, and hemorrhagic areas (1). Microscopically mature adipose tissue is admixed with hematopoietic elements and residual cortical parenchyma (1-3, 5-7). The hematopoietic foci show trilineal hematopoiesis, typically varying in cellularity, and increased numbers of megakaryocytes (1-3, 5-7).
The etiology of this lesion is not known. A common theory is that these masses result from metaplasia of stromal cells secondary to stimuli such as stress, necrosis, or infection. This hypothesis derives support from experiments from the 1950s, in which researchers induced myelolipomatous changes in rats by injecting them with necrotic tumor and adrenocorticotropic hormone (10). More recent evidence suggests that myelolipomas may be clonal. Bishop et al. evaluated the H&E morphology, immunohistochemical phenotype, and X chromosome inactivation of the hematopoietic elements of 19 adrenal myelolipomas (7). They confirmed previous findings of highly variable cellularity in the hematopoietic foci (range of 5% to 90%) and increased megakaryocytes. They found no evidence of increased immature hematopoietic elements by either H&E or immunohistochemistry (CD117, CD34). Also there was no evidence of dysplasia in any of the hematopoietic lineages. Of note, the investigators did identify increased stromal reticulin fibrosis. Also, analysis of X chromosome inactivation (performed in 11 of the cases) showed non-random inactivation in the hematopoietic elements of 8 (72%) cases (one case was non-informative, two showed random inactivation). Seven of these also showed non-random X-inactivation in the adipose tissue. These findings suggest that myelolipomas may be clonal in origin.
For most lesions no treatment is necessary. Larger lesions (some authors suggest those greater than 10 cm) may require surgical resection to prevent the possibility of rupture and subsequent retroperitoneal hemorrhage (1, 8, 9).
References:
-
Rosai J. Adrenal gland and other paraganglia. In: Rosai and Akerman's Surgical Pathology- 10th Edition. New York: Mosby Elsevier, 2011.
-
Lam KY, Lo CY. Adrenal lipomatous tumor: a 30 year clinicopathological experience at a single institution. Journal of Clinical Pathology 2001; 54: 707-712.
-
McDonnell WV. Myelolipomas of the adrenal. Archive of Pathology 1956;416-419.
-
Olsson CA, Krane RJ, Klugo RC et al. Adrenal myelolipoma. Surgery 1973;73:665-670.
-
Plaut, A. Myelolipoma in the adrenal cortex. American Journal of Pathology 1958;34:487-515.
-
Kenney PJ, Wagner BJ, Rao P, et al. Myelolipoma: CT and pathologic features. Radiology 1998;208:87-95.
-
Bishop E, Eble JN, Cheng L, et al. Adrenal myelolipomas show nonrandom X-chromosome inactivation in hematopoietic elements and fat: support for a clonal origin of myelolipomas. American Journal of Surgical Pathology 2006;30:838-843.
-
Han M, Burnett AL, Fishman EK, Marshall FF. The natural history and treatment of adrenal myelolipoma. The Journal of Urology 1997; 157:1213-1216.
-
Sanders R, Bissada N, Curry N, Gordon B. Clinical spectrum of adrenal myelolipoma: analysis of 8 tumors in 7 patients. The Journal of Urology 1995;153:1791-1793.
-
Seyle H, Stone H. Hormonally induced transformation of the adrenal into myeloid tissue. American Journal of Pathology 1950;23:211-233.

 Meet our Residency Program Director
Meet our Residency Program Director