Residency Program - Case of the Month
August 2015 - Presented by Dr. R. Jeanna Su and Dr. Mingyi Chen
History
A 74-year-old woman underwent living donor kidney transplantation for chronic kidney disease on 5/15/2012. Patient received immunosuppressive therapy with Tacrolimus (FK-506) and mycophenolate mofetil (MMF) initially. She was discontinued from MMF and slowly weaned down on Tacrolimus to a goal level between 3-4 ng/ml to maintain a non-rejected state. Patient's serum creatinine has been stabilized to 1.2-1.9 mg/dl. However, the patient developed fatigue, fever, cough, diarrhea and small bowel obstruction 30 months after the transplantation and was found to have bilateral pleural effusion. Physical examination found left auxiliary lymphoadenopathy and hepatosplenomegaly. She was transferred from nephrology transplant facility to hemetology/oncology service on 11/19/14.
Biopsy and Fixation
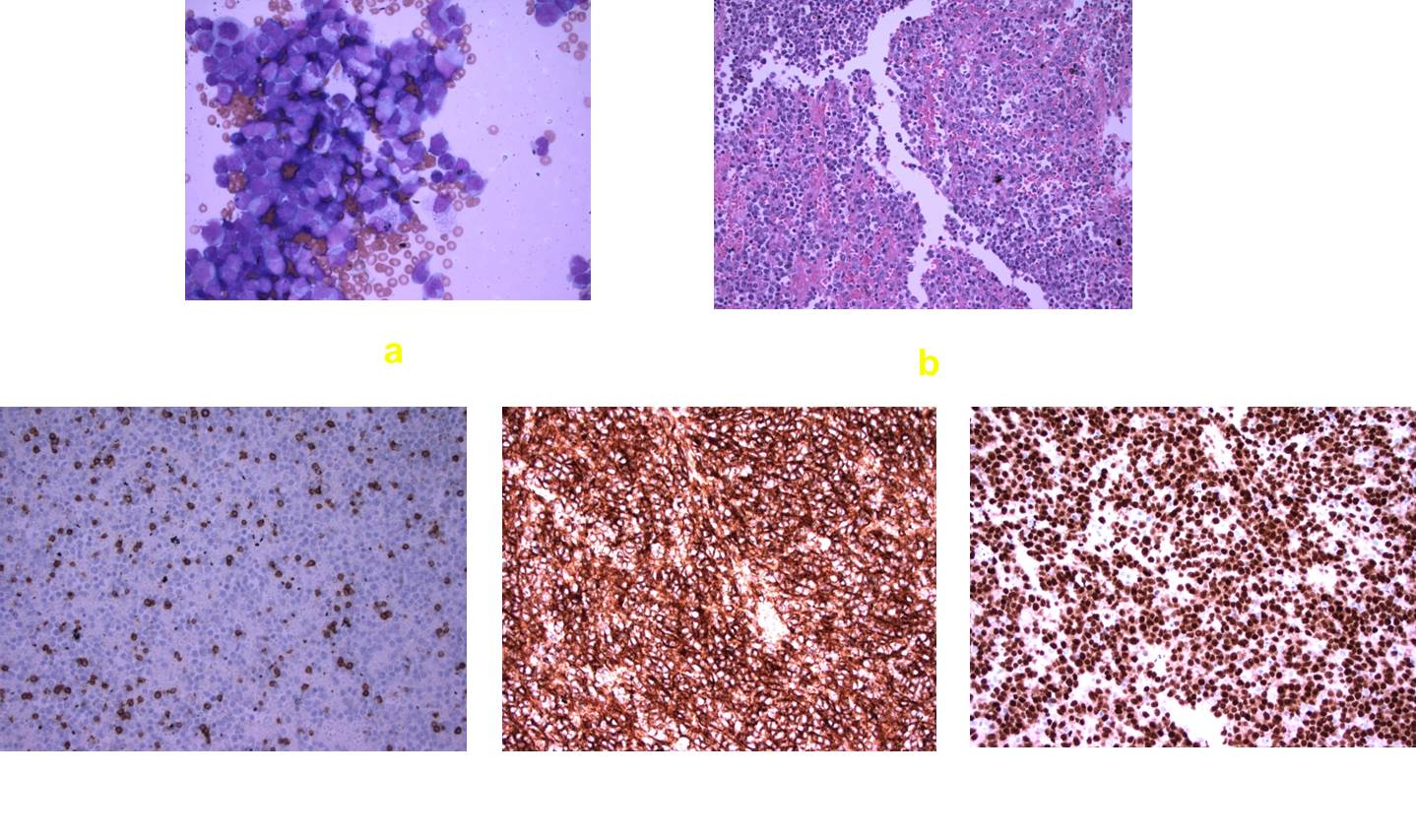
Pleural fluid cytology studies (Figure 1a) and HE stained cell block sections (Figure 1b) showed numerous large atypical lymphoid cells. Fine needle aspiration (FNA) smears (PAP and HE stains) of left axilla lymph node showed a component of large to intermediate lymphocytes admixed with small lymphocytes in the background.
Figure 1a & Figure 1b |
 |
Gross and Microscopic Description
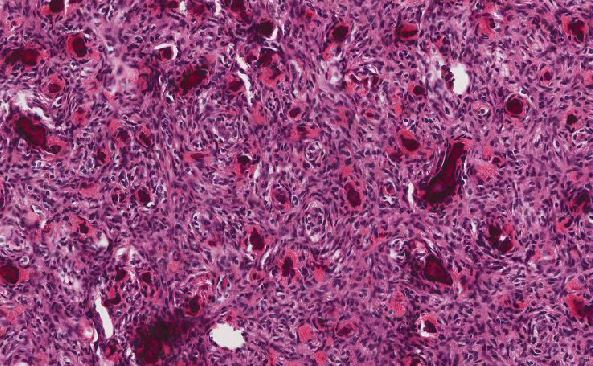
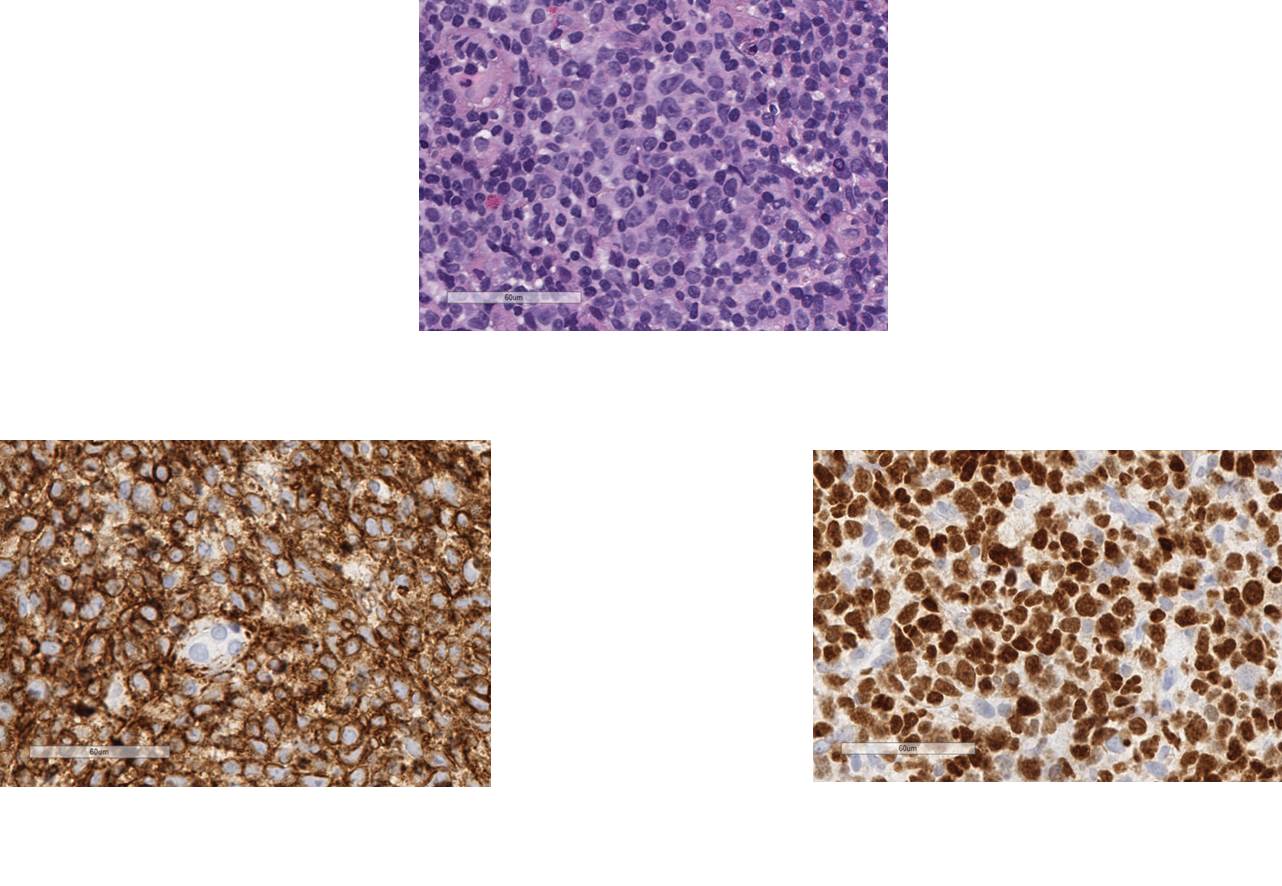
The concurrent lymph node biopsy HE stained sections showed sheets of large atypical lymphoid infiltrate. Large lymphoid cells have oval to round, vesicular nuclei containing fine chromatin, occasional nucleoli, large amount of basophilic cytoplasm and many mitotic figures (Figure 2).
Figure 2 |
 |
Immunohistochemistry/Flow Cytometry
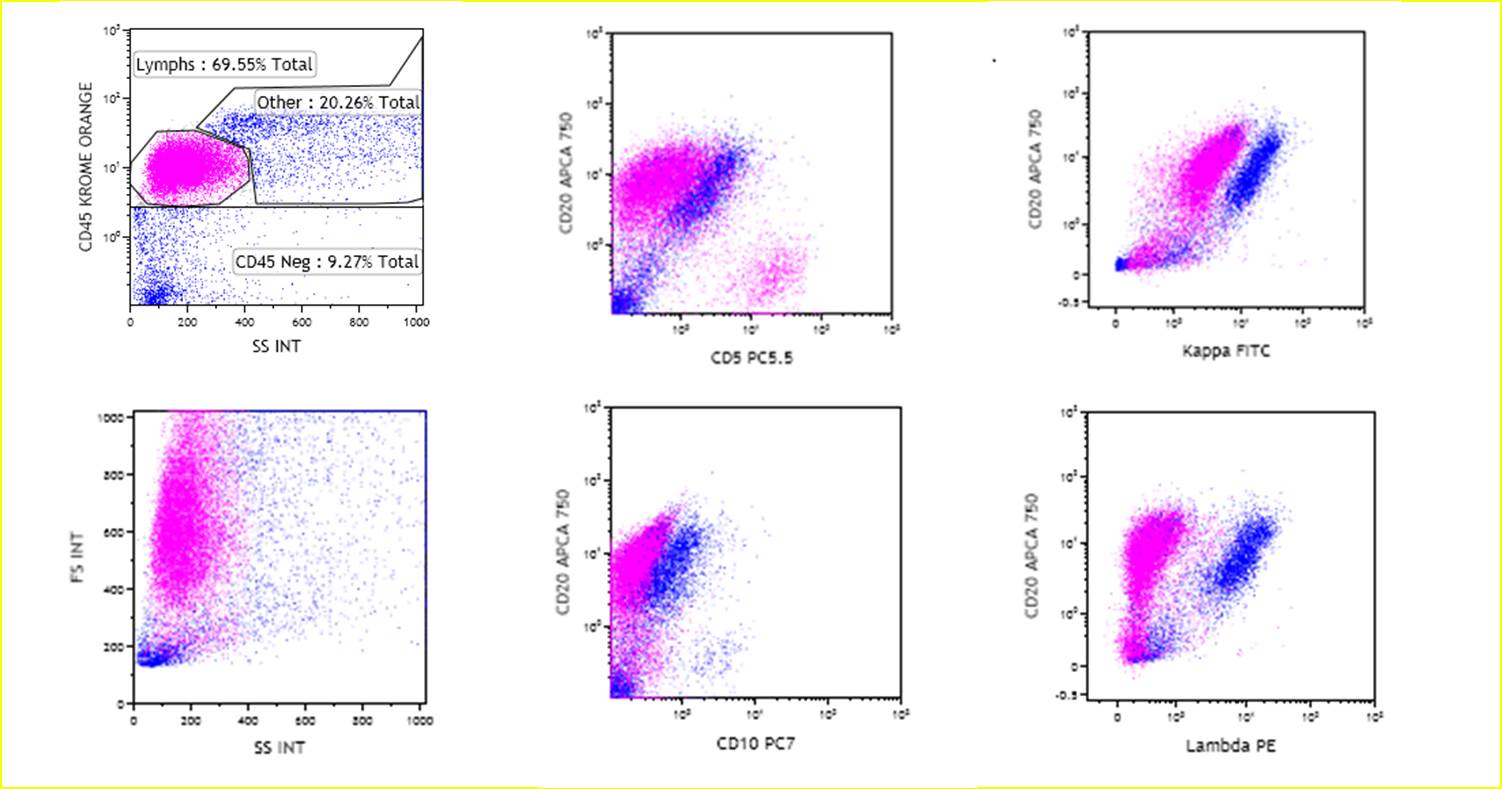
By immunohistochemistry, the abnormal lymphoid infiltrate on left axilla lymph node was diffusely positive for B-cell marker (CD20 and PAX-5) with co-expression of BCL-2, BCL-6 and MUM1 (Figure 2). CD30, CD138 and Cyclin D1 were negative on these cells. CD3 and CD5 stains highlighted the reactive non-neoplastic T-cells in the background. The tumor cells showed high proliferation index with 60-70% of cells positive for Ki-67 (Figure 2). Similar pattern of immunohistochemistry staining was observed on pleural fluid cytospin smear (Figure 1). Overall, the combined morphologic and immunohistochemical findings were diagnostic for diffused large B cells lymphoma (DLBCL). The negative CD10 and positive BCL6 and MUM1 staining was consistent with a non-germinal center phenotype. Flow cytometry analysis of pleural fluid, fine needle aspirates and core biopsy of the left axilla lymph node consistently showed a kappa restricted B cell population that was CD5- and CD10-. The lymphoid gate accounts for 70% of events. The cells marked as B cells with kappa light chain restriction. There was no abnormal coexpression of CD5/19 or CD10/19 (Figure 3), consistent with kappa monotypical CD5-/CD10- DLBCL, a high grade mature B-cell lymphoma.
Figure 3 |
 |
Cytogenetic findings
Epstein Barr Virus (EBV) serology showed past infection, however, EBV DNA was not detected by PCR in blood. EBER in Situ Hybridization (ISH) was negative on lymph node specimen (Figure 4). Human herpesvirus-8 (HHV8) detection was negative (Figure 4). Hepatitis C virus (HCV) antibody and RNA PCR were negative. Cytomegalovirus (CMV) IgG antibody was positive and BK virus (BKV) was detectable in the urine.
Figure 4 |
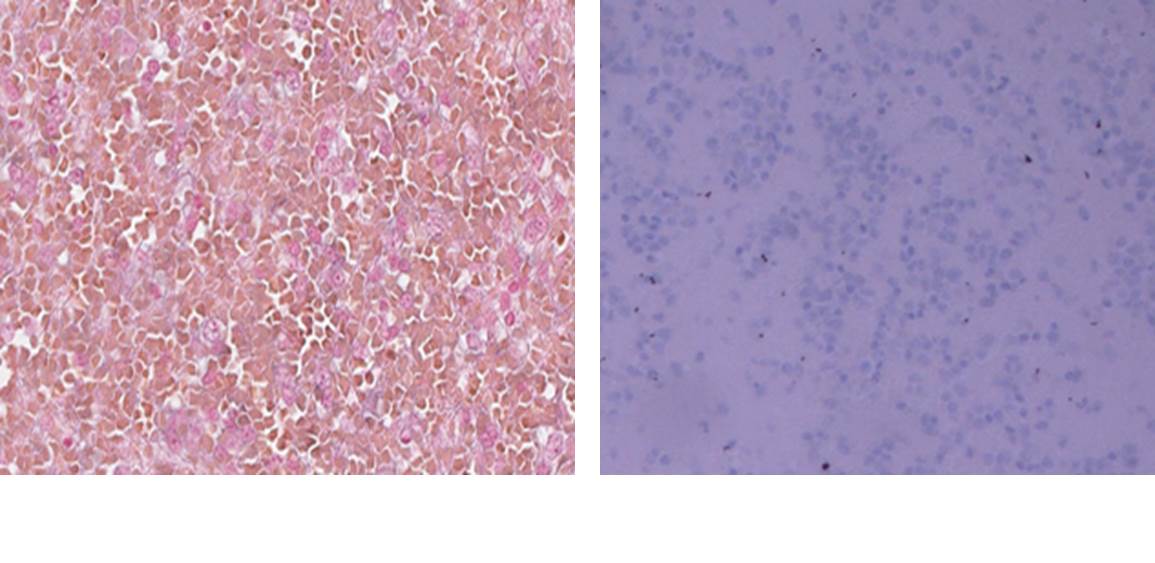 |
Molecular findings
FISH for bcl-2, bcl-6 and c-myc translocations were negative
Answer

 Meet our Residency Program Director
Meet our Residency Program Director