Best practices for children with prominent ears
UC Davis surgeons outline the nuances of treating this common condition with otoplasty
Children with protruding ears can face bullying, anxiety and other issues. One solution is otoplasty, a safe and common procedure to change ear shape and size. In an article published in the journal Facial Plastic Surgery Clinics of North America, UC Davis Health’s Travis Tollefson, a professor in the Department of Otolaryngology, and colleagues, outline several best practices for surgeons approaching otoplasty.
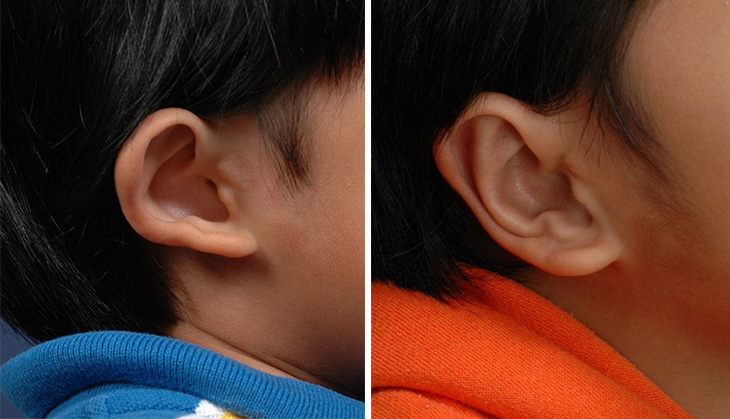
For Tollefson, who also directs the Division of Facial Plastic and Reconstructive Surgery, the process begins with in-depth conversations with families. Ideally, the child is old enough to participate in these talks and help make any decisions. He encourages all participants to consider the physical and psychological aspects of craniofacial differences when approaching these procedures.
“We want the families to know that there's no such thing as a normal child or a child that's not normal,” Tollefson said. “They're all just children with differences in how their ears look, how their nose looks, how their lips look. It’s important not to stigmatize these kids.”
Tollefson notes that some parents may have sensitivity over their own ears and may transfer those concerns to their child. He encourages physicians to discuss the parents’ experiences, as well as the child’s, to better reach consensus among family members. He says in some cases, the best solution is doing nothing at all.
Setting Expectations
Otoplasty is a safe and effective procedure, but ultimately the results will be viewed subjectively. While surgeons hope to improve ear projection and symmetry, Tollefson says it’s important to recognize that the human face is intrinsically asymmetrical. Whether it’s eyes, knees or ears, each component in any bilateral correction will be compared to the other. Precise measurements are a necessary step towards achieving good outcomes, but it’s also important to set expectations.
“Anytime we’re operating on two parts of the human body on two sides, there’s risk that the two sides won't turn out exactly the same,” Tollefson explained. “We have to communicate to the parents and child that there's going to be minor differences between the two sides. Our goal is to make it better, not to make it perfect.”
Tollefson and colleagues take advantage of UC Davis’s 3D-printing lab, which gives surgeons a great tool to show parents and children models of the ears before and after surgery. This gives surgeons a unique opportunity to tell the story of the procedure.
“It helps set expectations and create a better experience for the family,” Tollefson said. “I explain where the scar will be and the efforts we make to prevent complications, such as blood collection behind the ear.”
Taking a conservative approach to the amount of skin being removed from behind the ear is a smart way to avoid excess tension. That’s an important consideration when surgeons mark things out before surgery.” —Travis Tollefson, professor, Department of Otolaryngology, director, Division of Facial Plastic and Reconstructive surgery
Conducting the Procedure
Tollefson notes that surgeons must be meticulous to avoid bleeding during surgery and keloid scarring afterwards. Some patients are more prone to develop these scars behind the ears, which develop after surgery.
To prevent keloids, he says, surgeons must avoid tension. The procedure involves taking away skin, which can be tricky. Removing too much skin should be avoided because this places excess tension on the wound, potentially leading to unwanted scarring.
“Taking a conservative approach to the amount of skin being removed from behind the ear is a smart way to avoid excess tension,” said Tollefson. “That’s an important consideration when surgeons mark things out before surgery.”
Following surgery, patients wear a pressure dressing for up to three days. Once again, setting expectations is important because young patients may want to adjust or even remove it. After the dressing officially comes off, a scarf or headband can keep the ears appropriately positioned, particularly at night when they can be flipped forward on the pillow and hyperextended.
While otoplasty is an effective plastic surgery procedure to change ear shape, it may not be covered by insurance.
“Insurance needs to be part of an open-ended discussion,” Tollefson said. “The pediatrician who referred the child may reference bullying and other social implications in the referral, but that may not help with coverage. Families and surgeons should be on the same page to set up realistic expectations and avoid potential conflicts.”
Co-authors on the article included Steven G. Hoshal and Megan V. Morisada, both of UC Davis.