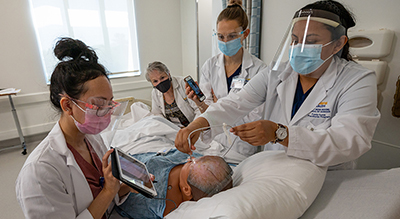
Social conditions, environmental factors and health outcomes. In the agricultural Central Valley of California, these are among the worst. The region has the worst air, water and land pollution in the state. And 100% of the population lives in a federally designated health professions shortage area. During the height of the COVID-19 pandemic, virus positive rates in the Central Valley more than doubled that of the rest of the state. Health care providers had to pivot from in-person services to telehealth.
While the nation experienced a rapid increase in virtual visits, the pandemic highlighted the lack of access to digital health systems for rural and underserved communities. So, faculty from the Betty Irene Moore School of Nursing at UC Davis saw an opportunity to improve digital health to underserved communities. In September 2020, researchers at the Center for Information Technology Research in the Interest of Society & the Banatao Institute (CITRIS) at the University of California launched Accountability, Coordination and Telehealth in the Valley to Achieve Transformation and Equity (ACTIVATE). The effort is co-led by Director of Health David Lindeman and Katherine Kim, a former associate professor at the School of Nursing (Kim left the school in July 2021). The public-private pilot initiative aims to bring telehealth services to underserved rural residents in Merced County.
“We want to co-design solutions that connect the clinic setting to the home environment to improve the health and well-being of rural and underserved people,” Kim explains. “We’re building this model to enable health equity and provide a sustainable model that will start in the Central Valley and expand into the rest of the country.”
At the heart of connecting patients to providers via technology is the ability for communities to connect to broadband services. In fact, researchers consider the internet a “super social determinant of health.” In 2019, residents of the Central Valley were among the least connected.
“These communities lack computers, tablets and smartphones, as well as health devices, such as blood pressure machines or glucometers,” Kim says. “It also takes education and mentoring for someone to learn to use the digital technology. Add to that the lack of resources of clinics to provide the technology and culturally appropriate education to patients.”
The ACTIVATE team addresses these challenges through a digital health pathway that maps out what a patient’s journey may look like as they navigate diabetes, hypertension or mental health challenges. The pathway represents the relationship a patient has with the clinic overtime and including many interactions and requiring a team-based approach.
But researchers did not create the pathway alone. They co-designed it with Livingston Community Health, which serves these patients in Merced County, to get input from the many voices in the community.
“Our team has real-time knowledge of our patients’ needs. We also recognize any barriers to health and provide options,” explains Rosa Pavey, Livingston’s clinical training manager. “Our long-term hope is for all patients to recognize, understand their diagnosis and learn how to treat it while using the education and equipment provided through this program.”
Driving the program are critical health care workers at the front lines of care who have the cultural and linguistic skills to break down barriers to access physical and mental health services. In the first pilot of 12 patients, participants received health education and training in digital literacy as well as tablets, internet access, and remote patient monitoring equipment needed to connect with health care providers and self-manage chronic health conditions.
“Telehealth represents a safe and effective way for many populations, including rural and low-income communities, to access necessary health care,” says David Lubarsky, CEO of UC Davis Health. “Ultimately, we plan to provide a roadmap for both public and private partners, setting a gold standard in California and across the nation.”
The program is expected to rapidly expand throughout the state to other community health centers and clinicians that serve vulnerable populations. But Kim says the success relies on permanent funding.
“If we don’t have ongoing reimbursement for primary care telehealth for patients in their homes, community health centers won’t be able to provide the service,” Kim says. “As we document our model and create our toolkit, we’ll disseminate those findings to other states. We hope that all we’ve learned and created can be used throughout the country.”