Endocrine surgeons perform first ‘scarless’ thyroidectomy in Central Valley
Innovative surgical technique allows removal of thyroid gland
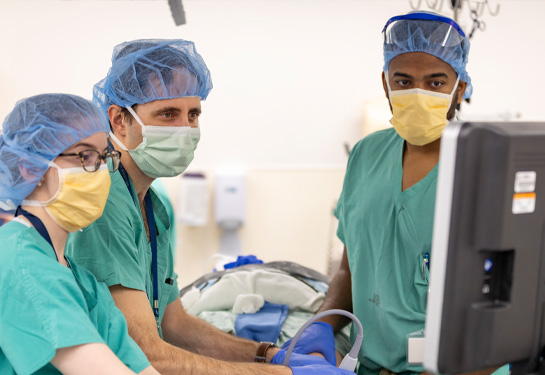
UC Davis Health endocrine surgeons performed the institution’s first “scarless” thyroidectomy, the removal of the thyroid gland. UC Davis Medical Center is the first hospital in the California Central Valley to perform the procedure.
Claire E. Graves, assistant professor of surgery, and Michael Campbell, associate professor of surgery, performed the procedure using a technique known as a transoral thyroidectomy. It was pioneered in Thailand in 2014 and has spread to a handful of medical centers in the United States.
Innovative surgical technique involves the lip
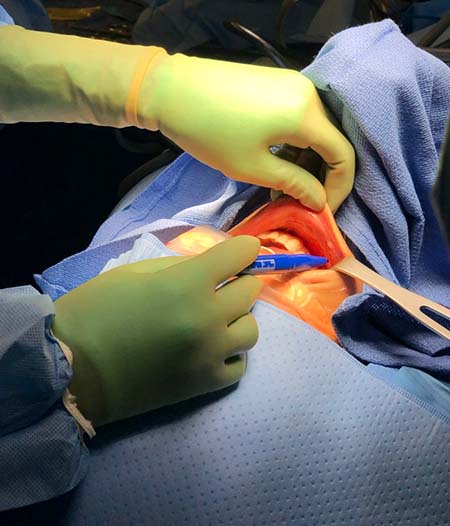
This surgical technique requires three small incisions inside the lower lip. Through these incisions, the surgeon places endoscopic instruments between the jaw and the skin to remove the thyroid gland, which is a short distance from the incision site. The procedure leaves no visible surgical scar on the neck of the patient.
The technique is limited by the size of gland that can be removed through the lip without discomfort at the chin. A modification of the technique also uses a small incision just under the chin. This “submental” incision is hidden from view but shortens the path from the incision to the thyroid gland to decrease surgical trauma.
“The transoral thyroidectomy, as well as the transoral and submental approach, were developed due to increased interest from patients to minimize the visible evidence of surgery,” explained Graves. “For many patients, a scar on the front of the neck affects whether or not they want to pursue surgery. Patients are often concerned about how it will affect their quality of life.”
The thyroid is a small gland responsible for producing hormones that play a crucial role in many of the body’s systems — from cells and tissues, to organs like the heart, brain, liver, and kidneys. It's estimated that over 30 million Americans have thyroid dysfunction. Approximately 150,000 thyroidectomies are performed each year in the United States.
Patients undergo thyroid removal surgery for several reasons:
- A nodule on the gland that is cancerous or may become cancerous
- A thyroid nodule that is enlarged and causing dangerous or bothersome symptoms
- An overactive thyroid (hyperthyroidism) that does not respond to other treatments
This procedure has a patient-centered value as a scar on the front of the neck is not only a health privacy issue, but it’s a constant reminder for a patient that they had surgery. If it was for cancer, then it’s a constant reminder that they had cancer. This procedure offers our patients another option that they have not previously had.”—Michael Campbell
The benefits of a “scarless” procedure
Traditionally, surgeons remove the thyroid gland using a small horizontal incision in the center of the neck. The scar size depends on the size of the gland, with the average being 4 to 6 centimeters long.
“People don’t look into the deeper understanding of what that cosmetic value actually is for patients,” said Campbell. “This procedure has a patient-centered value as a scar on the front of the neck is not only a health privacy issue, but it’s a constant reminder for a patient that they had surgery. If it was for cancer, then it’s a constant reminder that they had cancer. This procedure offers our patients another option that they have not previously had.”
Currently, a patient’s eligibility for a transoral thyroidectomy depends on the treatment required.
“A transoral thyroidectomy requires careful selection of the appropriate patient and disease to utilize this approach,” said Graves. “This procedure will not work for patients with large tumors, or where there is concern that cancer has spread beyond the thyroid.”
The main benefit of a transoral thyroidectomy is the lack of scarring. Data show the procedure is as effective as the traditional, through-the-neck route.
Individuals seeking a surgical consultation should visit the UC Davis Health Request an Appointment web page or call 1-800-2-UC DAVIS (1-800-282-3284). Physicians wishing to make a surgical referral should visit our Refer a Patient web page.