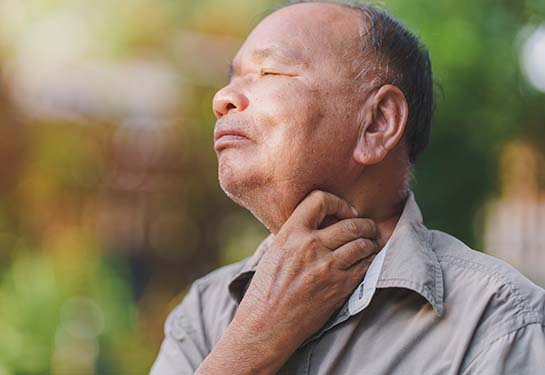
How does removing the voice box affect the sense of smell?
Total laryngectomy blunts olfactory functions and impacts patient’s quality of life
A new study by UC Davis Health researchers assessed the quality of life of patients who had their voice box removed. It showed that 60% experienced moderate to severe changes to their sense of smell, even two years after the operation.
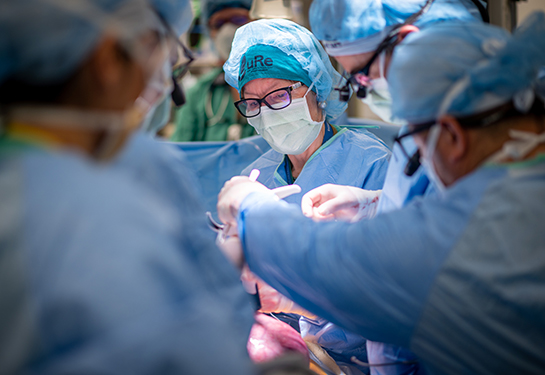
Total laryngectomy is a surgery to remove the voice box - also known as the larynx. People with cancer on or near their vocal cords or those with a damaged larynx due to a severe injury or radiation treatment may need this life-saving operation.
The voice box includes cartilage that covers the larynx when swallowing to protect the lungs from food and drink going down the wrong way. A dysfunctional larynx may result in choking or pneumonia.
Removing the larynx changes the way people speak and swallow. Patients are generally informed about how the surgery will affect their voice and swallowing, but they are not often made aware of one other side effect: the loss of smell and taste.
“Most counseling to laryngectomy patients focuses on the voice and swallowing. While patients are also expected to experience changes in their smell and taste, they rarely are prepared for such changes. That's what led us to look at smell specifically and its impact on the patient’s quality of life,” said the lead author of the study Marianne Abouyared, an assistant professor of otolaryngology and head and neck surgeon at UC Davis Health.
Why do laryngectomy patients lose their sense of smell?
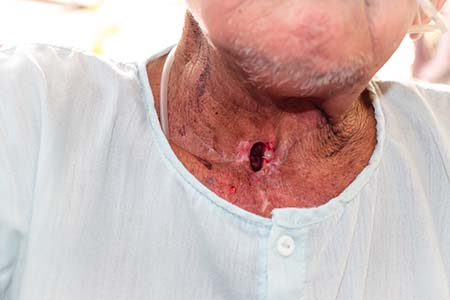
In a total laryngectomy, the surgeon removes the vocal cords and voice box and creates a permanent hole (called a stoma) in the patient’s neck. After surgery, the patient breathes only through this opening.
Breathing through the stoma affects the patient’s sense of smell largely because air no longer passes through the nose. The permanent disconnection between the upper and lower airways disrupts the normal airflow. This disruption reduces stimuli to the sensory tissues and causes loss of smell.
The study
The study enrolled 30 total laryngectomy patients. These patients had a median age of 71 years, were mostly male, and 63% of them had a history of tobacco use. They had the operation either for squamous cell carcinoma (57%), dysfunctional larynges (37%) or papillary thyroid carcinoma (6%). Their average time between surgery and filling out the survey was approximately two years.
The researchers assessed the patient’s quality of life using the Questionnaire of Olfactory Disorders Negative Statements (QOD-NS) and the Sino-nasal Outcome Test-22 (SNOT-22).
While patients are also expected to experience changes in their smell and taste, they rarely are prepared for such changes.”—Marianne Abouyared
A QOD-NS score less than 38.5 is considered abnormal. The researchers found that the average QOD-NS score was 37.9, and 30% of the patients had abnormal scores. The group of patients with abnormal scores included a greater percentage of former smokers and more days since surgery than the group with normal scores.
Studies indicate that a SNOT-22 score greater than 20 indicates a moderate to severe impact on quality of life. The average SNOT-22 score was 32. Around 63% of the patients scored in the moderate to severe category and the rest in the normal to mild. Patients who were smokers were more likely to report severe symptoms.
“It wasn't surprising that people had a change in their sense of smell. Interestingly, patients who had their surgery a long time before filling out the survey reported more severe scores. So, this is something people are dealing with for a long time post-surgery,” Abouyared said.
Can patients smell normally again?
The study stressed the importance of patient counseling, considering how patients are affected in the short and long term. Patients typically think their speech and swallowing will be the most significant factors affecting their quality of life. The study showed that changes to their sense of smell will also shape their experience. The researchers proposed olfactory or smell counseling for patients.
According to Abouyared, there have been some studies on olfactory retraining in laryngectomy patients. Nasal Airflow-Inducing Maneuver is one approach that involves generating negative pressure through repeated yawning with closed lips. This “polite yawning” promotes nasal airflow and allows odors to reach the nasal epithelium.

“Nasal Airflow-Inducing Maneuver is a simple, inexpensive technique that has been shown to optimize odor perception and successfully improve smell in up to 50% of patients who routinely practice it after laryngectomy,” said Toby Steele, associate professor of rhinology, sinus and skull base surgery and coauthor of the study.
The study was published in the American Journal of Otolaryngology. Coauthors of this study are Roberto Solis, Mehrnaz Mehrzad, Beverly Garber, Angela Beliveau, Arnaud Bewley and Andrew Birkeland of UC Davis, and Amarbir Gill of the University of Utah.
Related stories: