OCT images predict likelihood of stopping eye injections
Early reduction in central subfield thickness increases odds of successfully discontinuing anti-VEGF treatments within 2 years
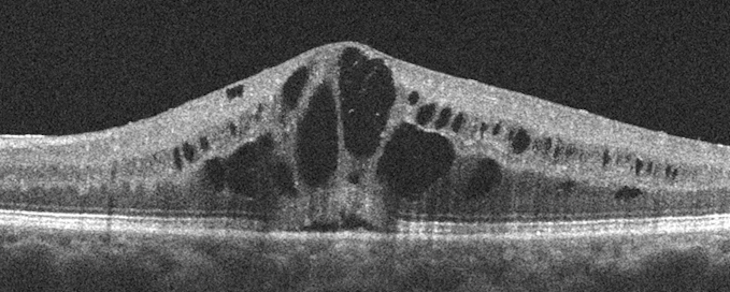
Patients with retinal vein occlusions who require frequent anti-VEGF injections are more likely to successfully wean off injections within two years if they show an early anatomic response, as measured using optical coherence tomography (OCT).
The researchers also found that early improvements in vision and an OCT feature known as disorganization of retinal inner layers (DRIL) predict long-term visual recovery.
The results of this new study from the Department of Ophthalmology and Vision Sciences at UC Davis Health were presented at the ARVO Annual Meeting in June.
“Injection of anti-VEGF agents for conditions such as age-related macular degeneration, diabetic retinopathy, and retinal vascular occlusions are invasive, costly and a tremendous burden for patients and providers,” said Glenn C. Yiu, senior author of the study and a professor in the Department of Ophthalmology and Vision Sciences.
Yiu notes that in 2016, 42% of the Medicare reimbursements to ophthalmologists were for eye injections. “Identifying predictors or prognostic factors for clinical outcomes and successfully discontinuing therapy is a critical unmet need in our field,” Yiu said.
For this study of 66 single eyes from 66 patients, the researchers employed masked graders to grade OCT images using standardized protocols to classify a battery of different anatomic features. The image biomarkers, analyzed at baseline, three months and six months after starting treatment, included:
- size of the largest intraretinal cyst
- subretinal fluid thickness
- number of hyperreflective foci
- percent disorganization of the retinal inner layers
- percent disruption in outer retinal layers, including the external limiting membrane, ellipsoid zone and interdigitation zone within the central macula
The results showed the main factor associated with successful discontinuation of anti-VEGF injections was a lower central subfield thickness (CST) at six months.
This suggests that baseline OCT biomarkers may be of limited utility to predict long-term vision compared to the same imaging after patients have received a few treatments.”—Glenn C. Yiu
Every 50 µm decrease, as measured by OCT, nearly doubled the odds of successfully stopping treatments within two years.
The study also found that many structural measures such as retinal thickness or retinal layer disruptions showed a stronger relationship with visual outcomes when assessed at later time points than at initial presentation. However, only DRIL was independently linked to visual outcomes in multivariate models.
“This suggests that baseline OCT biomarkers may be of limited utility to predict long-term vision compared to the same imaging after patients have received a few treatments,” Yiu said.
The UC Davis Eye Center
The UC Davis Eye Center provides world-class eye care, pioneers collaborative vision research, and trains the next generation of specialists and investigators to become leaders in the Sacramento region and beyond. The Eye Center team aims to transform vision care and develop cures for blinding eye diseases, from cornea to cortex.