What you need to know about the latest in shellfish allergy diagnosis and treatment
Shellfish allergy is very common in adults and children. It affects around 3% of adults and a little over 1% of children. Despite its prevalence and its potentially lethal symptoms, shellfish allergy remains a big challenge to clinicians to diagnose and treat.
In their review published in Current Opinion in Allergy and Clinical Immunology, Patrick Leung, Ph.D., and Christine Wai, Ph.D., examined the current status in the diagnosis and clinical management of shellfish allergy. They highlighted the imminent need for more specific diagnostic methods and effective and safe therapeutic approaches for shellfish allergy.
In this Q& A, Leung who is a professor of rheumatology, allergy and clinical immunology at UC Davis Health, answered questions on the latest advances in diagnosing and treating shellfish allergies.
Let’s start with the basics. What causes shellfish allergies?
There are many known allergens or proteins that might cause shellfish allergy. In fact, our review identified 49 crustacean and eight Mollusca allergens. They include sarcoplasmic calcium-binding protein and the newly identified glycogen phosphorylase from shrimp to name a few (see full list on WHO/IUIS and AllergenOnline). However, among all allergens, tropomyosin is best recognized as the major pan-allergen and the most well-studied shellfish allergen. It is also a common allergen in arthropods, like house dust mites and cockroach.
What are the standard diagnostic tests for shellfish allergy?
To diagnose shellfish allergy, the routine workup would involve a thorough review of clinical history, a skin prick test, and a serum-specific IgE antibody test to whole shrimp and tropomyosin determination. Clinicians will then assess whether an oral food challenge is necessary to confirm a diagnosis.
Still, accurate diagnosis of shellfish allergy should take into consideration factors that might greatly affect the sensitivity and specificity of these conventional tests. These factors include:
- likelihood of cross-reactivity among shellfish, house dust mite and cockroach
- the lack of standardization in allergen preparations used in the test
- variability of test protocols between laboratories
- the stability and shelf-life of the reagents
A blind food challenge remains the gold standard for food allergy diagnosis. However, this method is resource-intensive, time-consuming, expensive and with the risk of anaphylaxis that hampers its clinical implication. Recently, there has been a successful study on using nasal allergen provocation test to diagnose shellfish allergy. Yet, there is still a great need for a noninvasive but accurate diagnostic method for shellfish allergy.
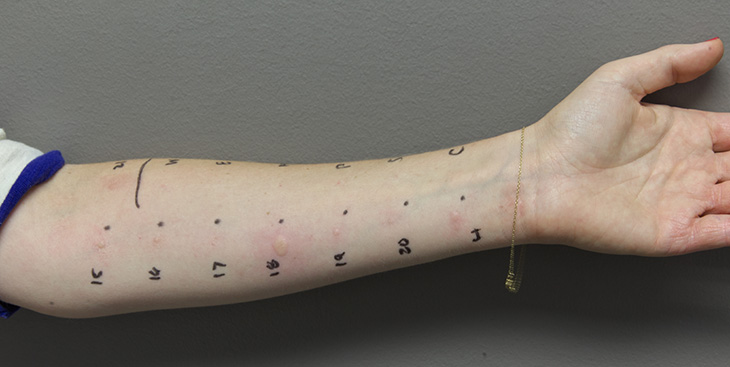
Based on your review, what would the best diagnosis plan look like?
Clearly, identification and validation of the optimal diagnostic algorithm for shellfish allergy are much needed. It is known that skin prick test and blood antibody test have low specificity. So, for patients with clinical history of shellfish allergy and negative skin and blood tests, we can do component-resolved diagnosis (CRD) and antibody crosslinking tests.
CRD allows the noninvasive and specific detection of a specific antibody reaction to individual allergenic molecules and allergen peptides. This CRD approach has the potential to diagnose shrimp allergy using serum samples.
As for the antibody crosslinking tests such as BAT (basophil activation test) and EXiLE, our group recently showed that their diagnostic value is higher than the conventional allergy tests. We found that a single- step diagnostic approach using BAT can replace skin prick test and specific IgE measurement in shrimp allergy diagnosis.
So, we suggest stepwise and combinatorial diagnostic strategies to conclude the diagnosis of shellfish allergy. For patients with inconclusive results using traditional standard testing, second-step tests can be ordered, which include CRD and IgE crosslinking tests. Food challenges are offered only when the results are uncertain to minimize risk to patients.
How long does it take shellfish allergy to resolve, if at all? Do people outgrow their shellfish allergy?
Studies show that 46% of people allergic to shrimp had their allergy resolved in 10 years. Meanwhile, patients are advised to avoid shellfish in their diet and take rescue medication in case of an allergic episode.
What role does immunotherapy play in treating allergies?
Immunotherapies are designed to desensitize food-allergic patients and to restore food tolerance in order to improve the quality of life in the affected individuals. There are different immunotherapy approaches for shellfish allergy.
One option is the use of hypoallergens. Our group constructed two hypoallergens of shrimp tropomyosin, namely MEM49 and MED171. These altered peptides do not cause an allergic reaction but carry a similar structure to tropomyosin. We found that these hypoallergens have the capacity to induce a specific antibody known as Immunoglobulin G (IgG) with inhibitory functions, which makes them great potential treatments in translational medicine.
DNA vaccine-based immunotherapy is another emerging trend in the treatment of allergies. Our group investigated the combined approach of using hypoallergens and DNA vaccine for the treatment of tropomyosin-induced shrimp allergy. We found that this treatment has the potential of sustaining tolerance against shrimp allergy.
Also, research on peptide-based immunotherapies identified six T cell peptides with immunoregulatory value, making them potential allergen-specific immunotherapy candidates.
Our group also identified 25 mimotopes (peptides resembling the epitopes of an allergen) of shrimp tropomyosin considered favorable immunotherapy candidates. These mimotopes can induce epitope-specific antibodies.
What do we know about the use of herbal medicines and probiotics in regulating allergic reactions, especially shellfish allergies?
One emerging immunotherapy approach is the use of traditional Chinese herbal medicine, such as the FDA-approved herbal formulation FAHF-2. Clinical trials showed that FAHF-2 treatment was safe and well-tolerated but with limited efficacy.
As for probiotics, they are commonly consumed as dietary supplements. They have been shown to modulate the immune system in allergic populations. Lactobacillus and Bifidobacterium are the two main probiotics shown to protect against atopic disease. Recent studies highlight the potential of probiotic supplementation to restore oral tolerance against shrimp allergy. A combination of probiotics and oral immunotherapy may be a possible strategy to enhance the safety and efficacy of allergen-specific immunotherapy.
What are some of the potential treatments to an allergic reaction?
Anti-inflammatory drugs (such as corticosteroids) and anti-IgE (like omalizumab) are mainstream nonspecific treatments that can be used alone or used in combination with oral immunotherapy for rapid desensitization and to reduce risk of allergic reactions. Other treatment options prescribed according to the needs of the patients include antihistamines and epinephrine.