Pediatric GI telehealth for COVID-19 pandemic and beyond
New review looks at the current landscape and identifies future challenges
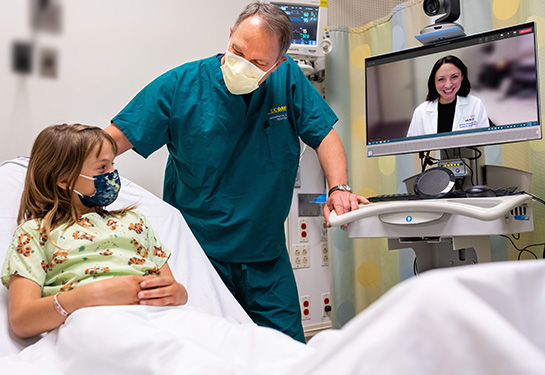
For many pediatric gastroenterology (GI) patients and families, telehealth visits during the COVID-19 pandemic have provided convenient, cost-effective care for chronic diseases like inflammatory bowel disease and celiac disease.
The use of technology to provide care remotely has also improved access to specialty care in rural communities, helping families overcome travel difficulties and reducing the time that children are away from school for doctor visits.
How is telehealth currently being used within pediatric GI and what does the future hold? This is the question asked in a new review by UC Davis pediatric gastroenterologist Daphne Say, which was published in the Journal of Pediatric Gastroenterology and Nutrition.
“As communities emerge from the COVID-19 public health emergency, telehealth has evolved into an important tool for pediatric specialists. This technology improves access to care for medically complex and underserved patient populations,” explained Say, lead author of the study. “Though traditional in-person care has resumed as physical distancing restrictions relaxed, telehealth for pediatric GI seems to be here to stay.”
In the review, Say and her co-authors aim to assess the current pediatric gastroenterology telehealth landscape. They examine challenges that inhibit successful telehealth implementation and sustainability and propose strategies by which telehealth can evolve to meet the needs of pediatric GI physicians and their patients.
Avenues for improvement in telehealth
Study authors note there are no specific diagnoses or patient populations within GI that are inherently appropriate or inappropriate for telehealth. While not every patient encounter works best as a telehealth visit, the following were obstacles identified that impeded telehealth adoption:
- inequitable access to broadband internet or video-capable devices
- poor digital literacy
- limited English proficiency.
With the end of the COVID-19 public health emergency, the study authors anticipate more telehealth obstacles. These may include the end of licensing waivers that previously permitted physicians to provide care across state lines through telehealth and concern that many commercial insurers may restrict reimbursement for telehealth services.
The study authors propose that the following are avenues for improvement and innovation in telehealth pediatric GI practice:
- Focus on identification of clinical scenarios best suited for virtual evaluation
- Standardization of telehealth curricula for pediatric GI trainees (medical residents and fellows)
- Development of recommendations for return to in-person care
“The ultimate question is how telehealth can be integrated into an in-person care model that increases efficiency, optimizes the patient and clinician experience, and is also financially solvent,” Say noted. “It is imperative that we keep abreast of changes in local regulations and reimbursement policies in order to ensure equitable integration of telehealth into the traditional in-person care delivery model.”
Other study co-authors were Sagar Pathak and Sabina Ali, of UC San Francisco School of Medicine; Arvind Srinath, of University of Pittsburgh School of Medicine; and Rajitha Venkatesh, of Nationwide Children’s Hospital.