UC Davis Health first in nation to name vice chair for geriatric emergency medicine
Move follows addition of new Healthy Aging Clinic, age-friendly emergency department accreditation
Older adult patients in the Emergency Department (ED) arrive with unique needs. In addition to physical illnesses, they may face cognitive decline and are challenged with resources to support them at home or in the community.
Reflecting the importance of a strong focus on older adults seen in the ED at UC Davis Medical Center, Emergency Medicine Chair Nathan Kuppermann recently named a new vice chair for Geriatric Emergency Medicine and Wellness.
Katren Tyler is the first to be named to this role in the nation.
Tyler, UC Davis emergency medicine faculty since 2005, developed a Geriatric Emergency Medicine Fellowship five years ago, the fourth in the U.S. and the only one on the West Coast. She also served as physician lead in the development, recognition and recent accreditation of the UC Davis Age-Friendly Emergency Department.
“This change signals a commitment from and sustained focus of the department on caring for older adults in the ED,” Tyler said. “More is not always more. Older people need a different focus and different attention paid to them.”
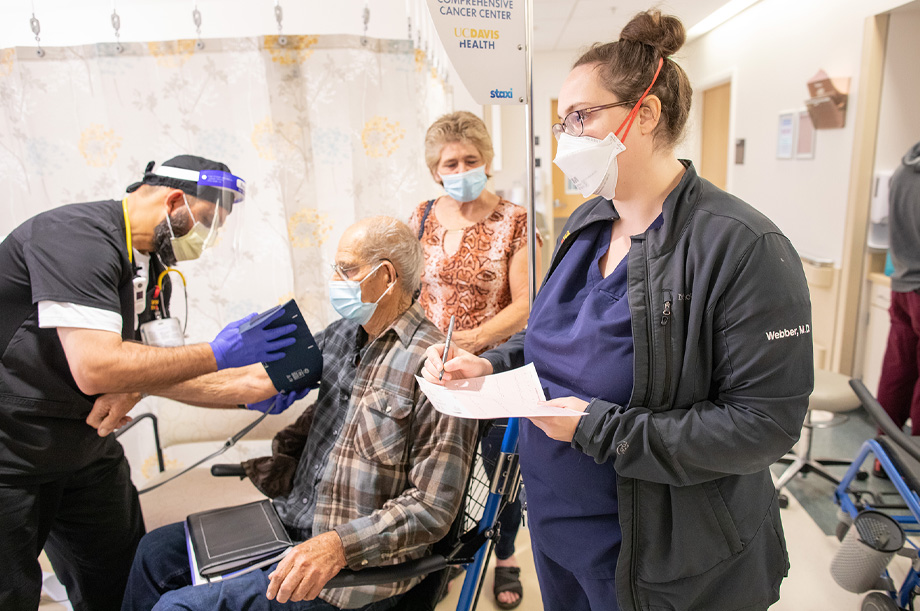
Unique needs come with aging
Under Tyler’s leadership, the UC Davis Health ED was recently awarded the Level 1 Geriatric Emergency Department Accreditation by the American College of Emergency Physicians (ACEP). UC Davis Health is the only ED in Sacramento to earn this accreditation and joins only 21 other EDs in the nation that have achieved gold status.
Most rooms in the UC Davis Health ED are age-friendly and a multidisciplinary team developed innovative workflows to improve the care of older adults in the department. This work was critical to earning the ACEP recognition and being named an Age-Friendly Health Systems Committed to Care Excellence by The John A. Hartford Foundation and the Institute for Healthcare Improvement (IHI).
What matters to patients affects bottom line
More than 46 million older adults age 65 and older live in the U.S. today. That number is expected to more than double by 2050, which could cripple health care systems.
If we don’t collectively get more efficient at caring for older adults in a way that is both caring and associated with better outcomes, health systems will be completely bogged down in navigating the care that older adults need.—Katren Tyler, vice chair for geriatric emergency medicine and wellness
“If we don’t collectively get more efficient at caring for older adults in a way that is both caring and associated with better outcomes, health systems will be completely bogged down in navigating the care that older adults need,” Tyler said. “Health systems like to pretend that we can do these things for free or that they’re easy to introduce. In reality, we know that changing culture and practice change requires a sustained commitment.”
Tyler and Kuppermann believe in leveraging the strength of an academic health system in the area of research. Last year, the Department of Emergency Medicine was ranked among the top 20 of schools nationwide in terms of funding from the National Institutes of Health, a position the department has held for more than a decade. That $1.23 million is key to caring for the older adult population in a sustainable way.

“It’s important that we have reliable and actionable data so that we can interface with the community to provide the best possible care for older patients,” Tyler said.
“Our Department of Emergency Medicine is unique in many ways. You’ve got to be a proactive and innovative thinker. We have 11 different fellowships, including one of only a handful of geriatric emergency medicine fellowships in the country. My guess is in the next 10 years, there will be another 15 programs like ours,” Kuppermann added.