Residency Training Program | Otolaryngology – Head and Neck Surgery

The Otolaryngology - Head and Neck Surgery Residency Training Program at the University of California Davis Medical Center in Sacramento, CA is five years in duration. Four applicants per year are selected to join the program. Residents who are in their last year of training and who are in good standing will serve as chief residents to their fellow trainees.
UC Davis provides comprehensive and robust clinical training in Otology & Neurotology; Head and Neck Oncology; Laryngology and Voice Disorders; Sinonasal Surgery and Allergy; Maxillofacial Trauma and Reconstruction; Pediatric Otolaryngology; and Facial Plastic and Reconstructive Surgery. In addition, our program provides residents with unique training opportunities in Cleft and Craniofacial Reconstruction, Skull Base Surgery, Microvascular Reconstruction, office based Laryngologic Surgery, and Pediatric Vascular Anomalies.
We offer two secondary clinical training facilities at the Sacramento VA Medical Center and at South Sacramento Kaiser Hospital, where trainees gain further training and knowledge of different healthcare systems and practices.
UC Davis Otolaryngology faculty organize and support several international medical missions within which residents are routinely involved during their training. Over the past 30 years, these have included missions to Ecuador, Nicaragua, Zimbabwe, China, and the Philippines.
Didactics are presented in a variety of formats. Grand Rounds presentations – including faculty, resident, and guest lecturers – are held weekly. Special areas of interest are covered in-depth. Our weekly resident didactics have been restructured into flipped-classroom instruction, spanning the gamut of subjects within otolaryngology – head and neck surgery, dentistry, audiology, speech pathology, and head and neck radiology. Rotating evening conferences hosted by each division further build on our residents’ knowledge base in all fields.
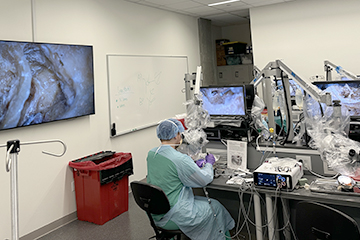
The department has a state-of-the-art temporal bone and endoscopic sinus surgery lab complete with multiple microscopic dissection stations, stealth image-guidance equipment, and microvascular surgery instrumentation. Each year residents are provided formal courses in temporal bone otomicroscopic dissection and endoscopic sinus surgery. Microvascular surgery training is available through independent study.
Our department feels a strong research experience is an integral component to the development of outstanding physicians and surgeons. To that end, our residents are provided dedicated research time during which they design and execute both clinical and basic science research projects in conjunction with our faculty or with faculty throughout the university. The department has research laboratories on both the Sacramento and Davis campuses within which to complete their work.
The goal of our program is to train residents to become exceptional otolaryngologists – head and neck surgeons. This is accomplished through intensive surgical and clinical instruction, a strong educational program, and a flexible research experience. After training at UC Davis, the majority of our graduates choose fellowship training and academic careers.
At UC Davis Otolaryngology, we place high value on scholastic excellence, intellectual curiosity, mentorship, personal development, and professionalism. We feel that our program offers its residents a rich and rewarding training experience from which they can launch as successful practitioners of our art and science.
First year residents complete five rotations in a variety of general surgery services as well as in Neurosurgery, Anesthesia, Emergency Medicine, Critical Care, Otolaryngology. Radiology/Pathology/Trauma and Pediatric ICU.
The second year resident takes night call in the hospital approximately every fourth day. During the on call time, the resident is responsible for inpatient consultations, emergency room consultations, calls from staff on hospital floors regarding our inpatients, from families or patients and referring physicians. S/he assists in any surgery occurring during that shift. S/he evaluates any patients for consultation and confers with a more senior resident, or faculty, for help in the assessment and decision-making procedure for treatment.
While in the clinic, s/he sees a variety of new and returning patients. These patients are discussed with a senior resident, fellow or a faculty member who helps in arriving at a treatment plan.
While in the operating room, under supervision, the resident performs such surgeries as tonsillectomy, adenoidectomy, myringotomy with placement of ventilation tubes, and placement of mandibular and maxillary arch bars. Small facial lesions are excised and facial lacerations are sutured. When more advanced cases are in progress, the first year resident may assist or be delegated to help in the clinic.
During the second year, the resident begins to take the otolaryngology Home Study Course that consists of packets of articles followed by an examination graded by computer. Second year residents frequently present the history and physical examination at our Case Presentations and Tumor Conference. Presentations should be focused and limited.
The third year resident continues to take hospital night call every fourth day. While in clinic, s/he makes basic decisions independently and follows through with diagnostic testing or trials of conservative management. If any surgical intervention is considered, a faculty member must be consulted. The third year resident assists medical students in evaluating and managing selected patients.
Surgical procedures appropriate for the third year resident include open reduction of mandibular and zygomatic fractures, submandibular salivary gland excision, septoplasty, laryngoscopy, bronchoscopy, esophagoscopy and selected sinus procedures. S/he assists in more major procedures, presents cases at Case Presentations and Tumor Conference, and is expected to present details from the literature regarding the subject being discussed.
The fourth year resident takes backup call from home and helps supervise residents and students in the clinic. S/he has primary responsibility for the majority of the complex inpatients on the otolaryngology service. Surgical procedures include tympanoplasty, endoscopic sinus surgery, cleft palate repairs, tympanomastoidectomy, middle ear surgery, radical neck dissection, and septorhinoplasty. On his/her call nights, the fourth year resident comes in for any major problems and for all surgical procedures. The backup call resident is expected to help with in-house call responsibilities when the workload limits expedient care. When there is not a fifth year resident on the team, the fourth year resident serves as chief resident.
The fifth year resident is the chief resident in charge of his or her team. All complex clinic patients and emergency room consults are reviewed by the senior resident before presentation to faculty, if possible. The fourth year resident decides on a treatment protocol subject to confirmation by a faculty member. Surgical procedures include rhinoplasty, blepharoplasty, cleft surgery, rhytidectomy, composite resection, laryngectomy, tympanomastoidectomy and middle ear surgery.
Three to five months of research will be completed during the second half of the PGY 3 and the first half of the PGY 4 of the residency program. The research will typically be broken into two blocks, depending on the nature of the research project. Typically, only one resident will be on research at a time. The rotations must be coordinated between the residents.
Residents on research will be required to attend all teaching conferences on the Sacramento campus and will have a Tuesday morning clinic (follow-up patients only) immediately after the Tuesday morning educational conference. Research residents will be relieved of weekday call schedule throughout their research months.
PGY 2 residents will meet with the research committee in September. Prior to the meeting, residents should individually meet with the faculty about possible research topics. They will present their ideas to the research committee and will be given feedback. The residents are expected to explore research options and do background reading during a one week research rotation.
Each PGY 2 resident will submit a written proposal to the research committee on May 1. In mid-May, the committee will meet with the PGY 2 residents to review the proposals and to work out any anticipated problems. If the resident wishes to pursue a research project outside of the department, a departmental faculty will be assigned to the resident at that time to act as an advisor and supervisor during the research months.
Between June and December of the PGY 3 year, residents are expected to make plans including submitting Resident Research Grants to the Academy (due date is January 15, awards announced in March) and obtaining animal protocol approval. Animals and reagents must be ordered at least two months in advance of the starting date of the research project.
All residents will present their research results at the annual UC Davis Resident Research Forum in June of each year. An award is given for best research project. PGY 2 residents are expected to present their research proposals.
Residents are strongly encouraged to participate in the annual Bay Area Resident Research Symposium held en June of each year. Approved expenses for research presentations at required national meetings are covered by the department.
The Department of Otolaryngology is dedicated to Diversity, Equity, and Inclusion (DEI) efforts. The following are some examples of our commitment.
Two of our Otolaryngology faculty, Dr. Rodney Diaz and Dr. Maggie Kuhn, serve on UC Davis Health’s IDARE Taskforce (Inclusion, Diversity, Anti-Racism, and Equity Taskforce).
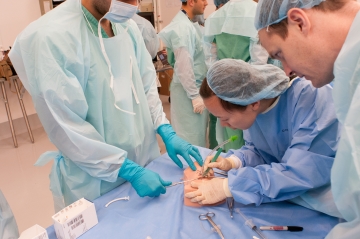
Our department hosts students from Sacramento Charter High School for an annual hands-on surgical skills session. The students learn about Otolaryngology and facial trauma, and they have the opportunity to work directly with skull models to practice reduction and fixation of various fracture patterns.
Prep Medico (Preparando Estudiantes Para Ser Medicos) is a UC Davis Program in which our department hosts Latino pre-med and medical students to shadow in our clinic. This program provides scholarships, mentorship, and internship opportunities for members of the growing Latino community in California, with the ultimate hope to increase the number of Latinos who chose to become physicians.
Our faculty are frequent speakers for UC Davis’ Health Equity Academy – Leaders for Tomorrow’s Healthcare (HEALTH). This program is offered to current California High School students three times a year and is free to participate. Students come from socioeconomically disadvantaged, underrepresented, or rural backgrounds. Through this program, they gain exposure to various career pathways in healthcare and meet health professionals of all levels (medical students, residents, faculty).
For more information regarding UC Davis Health DEI efforts, please visit: Office for Health Equity, Diversity and Inclusion
UC Davis Health System consists of UC Davis School of Medicine, UC Davis Medical Center, UC Davis Medical Group and the Community Hospital Program. As a part of this network, UC Davis Health System has developed one of the strongest telemedicine programs in the world.
UC Davis Medical Center located in Sacramento, 18 miles from the Davis campus, is the primary teaching facility for the School of Medicine and for postgraduate medical education offered by UC Davis. Approved residency training programs are available in 21 disciplines including Neurosurgery, Ophthalmology, and General Surgery. The hospital was founded in 1928 as the Sacramento County Hospital and in 1966 began its association with the University of California, Davis. Since 1973, the hospital has been owned and operated by the University of California.
UC Davis Medical Center, a major referral center for Northern California, is licensed for 613 beds and offers complete inpatient services, diagnostic facilities and 24-hour major emergency medical services. Specialty programs include a Trauma Service, a Burn Unit, a Transplant Service, a Regional Poison Center, an Eye Transplant Bank, a Regional Mental Health Program, a Model Family Practice Unit, a Neonatal Intensive Care Unit, a Comprehensive Rehabilitation Center and seven specialized intensive care units. There is a comprehensive ambulatory care program with over 100 Outpatient Specialty Services. The medical staff is comprised of approximately 669 full time faculty members of the School of Medicine and approximately 2,000 community-based physicians. The housestaff consists of 813 interns, residents and fellows and 407 medical students.
The University Children's Hospital is a NACHRI accredited children's hospital. There are currently 36 pediatric ward beds, two pediatric ICU's and a neonatal ICU. Dedicated pediatric operating rooms opened in 2006. Additionally, Shriners Hospital for Children - Northern California, located next to UC Davis Medical Center, provides an extensive pediatric experience.
The UC Davis Medical Center has approximately 32,886 admissions annually and had 863,394 specialty clinic visits and 46,196 emergency room visits last year.
The hospital and clinics occupy six main buildings on a 140-acre site. The Otolaryngology, Dental, and Speech and Audiology clinics are located in the Glassrock Building at 2521 Stockton Boulevard, 5th and 6th floors. The academic/administrative offices for these specialties occupy the 7th floor together with conference rooms and the Resident's Library. The entire complex is located one half mile south of Highway 50 on Stockton Boulevard.
Despite changes in the health-care industry, UC Davis Medical Center is undergoing rapid growth in its facilities. Between 1995 and 2009 the medical center will invest approximately $1,500,000,000 in new facilities. These will include new outpatient clinics, research facilities and a new 12 story inpatient tower. Twenty four new ORs, a new ER and 30 ICU beds are scheduled to open in 2009. This is an exciting time to be part of the campus.
 As California's capital city, Sacramento is on the move, serving up a diverse menu of outdoor activities, cultural events and nightlife.
As California's capital city, Sacramento is on the move, serving up a diverse menu of outdoor activities, cultural events and nightlife.
The city is racially and ethnically diverse, and in the past has been named by Time magazine and the Civil Rights Project as the most racially integrated major city in America. In addition to the obvious benefits of a rapidly expanding and diverse patient population, Sacramento is a very livable city. The standard of living is higher and the cost of living is lower when compared to California's other heavily populated regions — the Los Angeles area and the San Francisco Bay area.
-
Recreational opportunities. Sacramento's climate is ideal for persons seeking an active lifestyle. Horseback riding, golf and tennis are year-round activities. If you like the water, two major rivers (and numerous other waterways) are available for swimming, fishing, boating and rafting. Or set out on foot if you prefer hiking, camping, or rock climbing. The 30-mile American River Bike Trail is a riverfront paved path popular with cyclists, runners and leisurely-paced walkers.
-
Sports on tap. Sports fans in Sacramento can cheer on their favorite local team, whether it's at the arena, diamond or field. Enjoy NBA basketball at Sacramento Kings games, home-run excitement with the Triple-A Sacramento River Cats and fast feet on the field with men's professional soccer team Sacramento Republic FC.
-
Cultural connections. With professional ballet, opera and theatre companies, along with extensive dining options, art galleries and museums, Sacramento offers plenty of entertainment. In the evenings, find everything from DJs spinning hip-hop to bands playing original tunes. Join the nightclub crowd in downtown Sacramento, or keep the beat with salsa dancers stirring it up in the clubs. Explore local wineries and savor new cuisines. If you like a street fair atmosphere, try the monthly Second Saturday arts event. The Crocker Art Museum, with its impressive collection and extensive space for touring exhibits, is the region's visual arts hub. The Mondavi Arts Center at UC Davis provides two performance venues for local, national and international performances.
- Outdoor living. Most of the year, Sacramento's sunny days and mild evenings provide plenty of reasons to step outside and enjoy the weather. Sacramento is a Tree City, USA, in recognition of the beauty and density of the tree canopy. The City of Sacramento has an extensive park system, providing more than a thousand acres of green space and natural habitat. In Old Sacramento, experience Sacramento's waterfront pioneer days while you dine on the Delta King riverboat, or ride on a California State Railroad Museum steam-powered train excursion. Further afield, Sacramento is surrounded by some of the region's most beautiful and popular scenic vistas.
- Food and Dining. Sacramento is the farm-to-fork capital of America, which is showcased by the city’s vibrant dining scene. You’ll find our residents “eating the grid” at any one of the city’s many happy hours, or on a group outing during restaurant week. There’s no better way to enjoy the City of Trees’ beautiful park system than with food truck events. The greater Sacramento area also offers a vast array of global cuisines that reflect the diversity of our population. World class wines and Michelin-star restaurants are just a short trip to the Napa Valley away. For those who enjoy cooking at home, Sunday farmers markets and other events give you a chance to buy directly from the same farms that supply some of California’s best restaurants, and many neighborhoods within Sacramento have their own farmers markets.
More info: Living in Sacramento