News
-
May 29, 2026
School of Medicine celebrates students, residents, faculty and staff
Read the storyarrow_forwardThe UC Davis School of Medicine recognized students, residents, faculty and staff for outstanding contributions to the medical school as part of its annual awards. Jeffrey Hoch, associate director of the Center for Healthcare Policy and Research, received the Kaiser Foundation Hospitals Award for Excellence in Teaching.
-
May 8, 2026
Why human review is key to the success of AI in health care
Read the storyarrow_forwardProfessor Courtney Lyles discusses ways to detect and prevent bias in AI models and how UC Davis Health is building fairer and more reliable AI systems to serve patients and physicians. Lyles is director of the Center for Healthcare Policy and Research and a leading researcher in digital health.
-
April 8, 2026
Transportation problems disrupt dialysis care for patients with kidney failure
Read the storyarrow_forwardTransportation challenges create major barriers for kidney failure patients who receive hemodialysis at a clinic. These disruptions also heavily impact clinic staff. New research from the Center for Healthcare Policy and Research calls for more coordination between health and transportation systems.
-
April 2, 2026
Aggie Square partners release first community benefits progress report
Read the storyarrow_forwardUC Davis, the city of Sacramento and Wexford Science & Technology released the inaugural Aggie Square Community Benefits Partnership Agreement Annual Progress Report, highlighting early outcomes and investments tied to the development of the Aggie Square innovation district. The Center for Healthcare Policy and Research was among the first tenants at Aggie Square and hosted numerous public-facing events at the district during its first year of operations.
-
March 2, 2026
UC Davis leads national effort to revitalize primary care
Read the BMC Proceedings paperarrow_forwardLearn about the webinar on CHCF's websitearrow_forwardA new paper in BMC Proceedings highlights consensus recommendations from a 2024 conference on strengthening the U.S. primary care system. Center for Healthcare Policy and Research faculty and staff led efforts to create seven priority actions to improve workforce development, payment models, and research investment. The paper follows a February 2026 webinar, sponsored by the California Health Care Foundation (CHCF), featuring primary care experts discussing how they’re working to improve primary care.
-
January 29, 2026
Rethinking how health research is done
Read the storyarrow_forwardA School of Nursing doctoral student’s experience with the T32 ReACH program reveals how improving health begins with people and place. The ReACH program is led by Center for Healthcare Policy and Research Director Courtney Lyles and faculty affiliate Leigh Ann Simmons.
-
January 14, 2026
‘Whole health’ approach a winner for heart failure patients
Read the article in U.S. News & World Reportarrow_forwardA Center for Healthcare Policy and Research initiative to improve health and well-being among heart failure patients is showing success. The novel “whole health” program helping patients manage weight and improve their health and well-being was highlighted by U.S. News & World Report.
-
November 06, 2025
Hot Topics in Kidney Health podcast explores study on patient transportation
Listen on the NKF websitearrow_forwardWhat does it mean to design a study with patients, not just for them, and why does that shift matter for kidney care outcomes? Na’amah Razon and Bethney Bonilla from the Center for Healthcare Policy and Research answer these questions and more in a podcast with the National Kidney Foundation (NKF).
-
October 29, 2025
Science for Health Policy Summit brings together academics and policymakers
Learn about the summitarrow_forwardThe UC Davis Center for Healthcare Policy and Research hosted the Science for Health Policy Summit in Sacramento to strengthen the connection between health research and policy. Leaders in health policy and research discussed how they could help one another and improve evidence-based policymaking.
-
OCTOBER 22, 2025
Your top low back pain questions answered
Read the storyarrow_forwardUC Davis family and community medicine doctor Joshua Fenton answers the top 10 questions people ask about low back pain. He led a Center for Healthcare Policy and Research study testing communication strategies to reduce low-value, lower back (lumbar) spinal imaging.
-
October 15, 2025
What's at stake with federal research funding cuts
Read the storyarrow_forwardFrom Labs to Lives highlights the life-changing impact of federally funded research at UC Davis from medicine to food, agriculture to technology.
-
October 06, 2025
Heart failure patients benefit from “whole health” approach
Read the storyarrow_forwardThe Koa Family Program supports “whole health” for heart failure patients like Barbara Tiney and has shown positive outcomes in improving overall well-being. The Koa Family Program was created by the Center for Healthcare Policy and Research.
-
September 16, 2025
Podcast: Aimee Moulin on expanding opioid treatment in emergency departments
Listen on Health Affairsarrow_forwardHow can emergency departments become a gateway to treatment for opioid use disorder? In a Health Affairs interview, Aimee Moulin shares insights from her study on expanding low-barrier access to treatment and improving patient navigation in emergency settings. Moulin is a physician and investigator with the Center for Healthcare Policy and Research.
-
August 11, 2025
Prescribing blind: Clinical prevention in an evidence-free zone
Read the op-edarrow_forwardIn a MedPage Today op-ed, Joy Melnikow imagines a hypothetical future scenario facing a primary care physician. Drawing on her experience as a primary care physician and public health leader, including as a former director of the Center for Healthcare Policy and Research, Melnikow considers the possible consequences of a changed preventive services task force and immunization advisory committee in the U.S.
-
August 8, 2025
Dean’s Excellence Awards recognize outstanding achievements
Read about the awardarrow_forwardJoshua Fenton was recognized with the 2024 Dean’s Award for Excellence in Mentoring by the UC Davis School of Medicine. Fenton is a professor and vice chair of research in the Department of Family and Community Medicine and an affiliate of the Center for Healthcare Policy and Research.
-
June 23, 2025
New report aims to revitalize declining primary care in the U.S.
Read the storyarrow_forwardThe UC Davis Center for Healthcare Policy and Research hosted a national conference last October to discuss the crisis in primary care in the U.S. Now, an expert panel has released its recommendations.
-
May 2, 2025
CHPR's new home: UC Davis’ Aggie Square formally inaugurated
Read the storyarrow_forwardThe UC Davis Center for Healthcare Policy and Research moved into its new home at Aggie Square. The innovation district brings together UC Davis' cutting-edge research with private-sector companies and start-ups.
-
April 10, 2025
UC Davis Health uses AI models to leave no patient behind
Read the storyarrow_forwardThe Center for Healthcare Policy and Research brought together a team of experts from the population health, information technology, and equity teams at UC Davis. They created a population health AI predictive model. Its algorithm is programmed to identify patients who may benefit from care management services to deal with health problems before they lead to emergency department visits or hospitalization.
-
March 17, 2025
Community clinic achieved marked improvement in system-based tobacco cessation
Read the storyarrow_forwardWellSpace Health, a community clinic in the Sacramento area, launched a quality improvement project to advance “system-based” tobacco cessation in partnership with the UC Davis Center for Healthcare Policy and Research.
-
February 14, 2025
CHPR to develop better electronic clinical quality measures for Medicare program
Read the storyarrow_forwardOver the next five years, the UC Davis Center for Healthcare Policy and Research will develop and validate new electronic clinical quality measures using electronic health records data from UC Davis Health and the UC Health Data Warehouse.
-
January 23, 2025
Medi-Cal members have tobacco treatment disparities by chronic disease status
Read the storyarrow_forwardResearchers at the UC Davis Center for Healthcare Policy and Research studied California’s 1.5 million smokers who are covered by California’s Medicaid program, called Medi-Cal, to understand tobacco treatment disparities.
-
December 2, 2024
Applied methods discussion group starting in 2025
Read the storyarrow_forwardThe UC Davis Center for Healthcare Policy and Research in partnership with the Division of Health Policy and Management in the Department of Public Health Sciences will launch a new Applied Methods Journal Club in 2025. Participants will discuss the latest innovative methods in applied health services research.
-
November 6, 2024
The value of a negative result
Read the storyarrow_forwardSpinal imaging for back pain may not be needed, but patients might still ask for it. A program designed to help clinicians engage patients with back pain did not help reduce imaging rates, found a study from the Center for Healthcare Policy and Research.
-
November 1, 2024
UC Davis convenes experts to seek solutions to national primary care crisis
Read the storyarrow_forwardThe Center for Healthcare Policy and Research hosted a who’s who of state and national thought leaders and physicians eager to improve the declining state of primary care.
-
November 1, 2024
Researchers evaluate program to treat opioid addiction
Read the storyarrow_forwardResearchers at the Center for Healthcare Policy and Research received an award to help address the opioid overdose crisis by assessing a unique emergency department service. The $1.05 million, 3-year grant from the Centers for Disease Control and Prevention will support an evaluation of CA Bridge, an initiative to expand medication for addiction treatment in emergency departments.
-
October 2, 2024
UC Davis advances treatment of heart failure through ‘whole health’ program
Read the storyarrow_forwardResearchers have received a grant from the Rosenfeld Foundation to support a “whole health” approach to improve the health and well-being of heart failure patients. The grant builds on a recent Center for Healthcare Policy and Research pilot project.
-
October 1, 2024
Can telehealth help patients stick with Buprenorphine for opioid addiction?
Read the storyarrow_forwardA Center for Healthcare Policy and Research study focused on patients prescribed buprenorphine in emergency departments explores the effectiveness of telehealth visits in boosting long-term use of the medication for treating opioid addiction.
-
September 25, 2024
How does transportation impact dialysis patient outcomes?
Read the storyarrow_forwardLed by family medicine physician Na’amah Razon, researchers are conducting a study to better understand the impact transportation and different modes of transportation have on dialysis patient outcomes.
-
September 3, 2024
Women leading the way in healthcare research
Read the storyarrow_forwardSeptember marks Women in Medicine Month, an annual event celebrating the significant contributions of women in the healthcare field. In honor of this occasion, we spotlight three exceptional women working with the UC Davis Center for Healthcare Policy and Research.
-
August 22, 2024
Do workplace support programs help address frontline physician burnout?
Read the storyarrow_forwardA study by the UC Davis Center for Healthcare Policy and Research explored workplace support programs during the COVID-19 pandemic and their relationship to frontline physician burnout.
-
August 12, 2024
UC Davis nursing professor awarded $1.25 million training grant
Read the storyarrow_forwardUC Davis received a $1.25 million grant from the National Institutes of Health to focus on health equity. Courtney Lyles, director of the Center for Healthcare Policy and Research, is a co-principal investigator on the grant with Center affiliate and nursing professor Leigh Ann Simmons.
-
August 1, 2024
Research insights from a statistician working on mental health
Read the storyarrow_forwardYi Zhang, a senior statistician at the UC Davis Center for Healthcare Policy and Research, is working to collect and analyze data from multiple California counties as part of the EPI-CAL project. The project's goal is to transform mental health care in California.
-
July 1, 2024
Hypertension studies seek to advance digital health equity
Read the storyarrow_forwardTwo studies are being conducted by researchers at the UC Davis Center for Healthcare Policy and Research to advance equity and improve access to hypertension treatment. Both studies are in partnership with UC San Francisco.
-
June 28, 2024
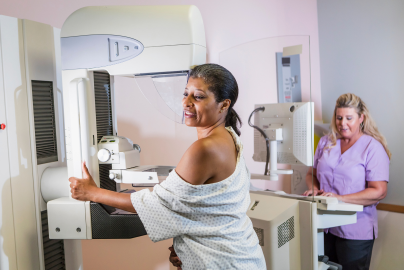
New guidance calls for all women to get mammograms starting at age 40
Read the storyarrow_forwardNew guidance recommends all women get screened for breast cancer every other year starting at age 40. The recommendation issued by the United States Preventive Services Task Force comes alongside a new systematic evidence review and modeling study published in JAMA that helped inform the updated recommendations.
-
June 28, 2024
Discover the latest on patient safety and get CME credits on PSNet
Read the storyarrow_forwardThe Center for Healthcare Policy and Research has won a $4 million award to run and edit the Patient Safety Network, an online resource to help improve patient safety and prevent medical errors.
-
June 3, 2024
Community-based research and healthy aging: Q&A with David Johnson
Read the storyarrow_forwardLed by David Johnson, a gerontologist at UC Davis Health, the Good Life program supports the healthy development and personal growth communities of color in and around Oakland, CA. Johnson takes a community-engaged approach to his research. This means members of the community are equal partners and collaborators in the research process.
-
May 1, 2024
CA Quits works to advance tobacco treatment for the Medi-Cal population
Read the storyarrow_forwardSince 2018, the CA Quits statewide project has focused on the implementation of tobacco treatment best practices with health systems and health plans serving California’s low-income population. The project is housed at the UC Davis Center for Healthcare Policy and Research.
-
April 1, 2024
Students get research experience through health equity-focused internship
Read the storyarrow_forwardThe UC Davis Center for Healthcare Policy and Research hosted four undergraduate students interested in health equity. The students interned at the Center from January through March 2024 as part of the Quarter at Aggie Square’s Advancing Health Care Equity experience.
-
March 18, 2024
Report finds state’s mental health programs need funding, community engagement
Read the storyarrow_forwardResearchers evaluated California’s mental health crisis management and prevention programs in a report that called for more sustainable programs and community collaborations to support people with mental illness. The report's contributors include staff and faculty affiliates from the Center for Healthcare Policy and Research.
-
March 7, 2024
New report highlights impact of roadway air pollution on indoor air quality
Read the storyarrow_forwardA new report by the UC-led California State Policy Evidence Consortium investigates the impact of near-roadway air pollution on indoor air quality. Dominique Ritley and Katrine Padilla, researchers at the Center for Healthcare Policy and Research, contributed to the report.
-
March 1, 2024
How health policy experts help California lawmakers make evidence-based decision
Read the storyarrow_forwardUpon request from the state legislative health committees, the California Health Benefits Review Program provides analyses of the medical, financial, and public health impacts of legislation affecting health insurance benefits and mandates. The Center for Healthcare Policy and Research coordinates the program's UC Davis team.
-
February 6, 2024
Paper finds novel weight-loss, telewellness program makes financial sense
Read the storyarrow_forwardA new economic analysis of a telewellness, weight loss study found that a community-based “whole health” program is a cost-effective approach to improving wellness among vulnerable populations. The analysis was published in AJPM Focus by a team from the Center for Healthcare Policy and Research.
-
February 1, 2024
Advancing healthcare quality and safety: Q&A with Patrick Romano
Read the storyarrow_forwardPatrick Romano is a healthcare quality expert who leads the Center for Healthcare Policy and Research's quality and safety research, including the AHRQ Quality Indicators program. The award supporting this work was recently renewed for three years with $1.4 million of funding. In this Q&A, Romano discusses the importance of healthcare quality and safety research and his latest work.