New training model helps surgeons practice minimally invasive spina bifida repair
A team of development engineers at UC Davis Tech Foundry and medical professionals at UC Davis Health has developed a teaching model to train pediatric surgeons on fetoscopic repair of spina bifida.
Spina bifida is a congenital condition where spinal tissue fails to fuse properly in the womb, leading to lifelong health problems. Fetoscopic repair is a minimally invasive surgical procedure to address conditions like spina bifida in a fetus. It is a type of laparoscopic surgery, where surgeons make tiny incisions and insert very small tools and a long, thin camera inside the patient’s body.
“Fetal surgery, and fetoscopy for spina bifida in particular, is one of the more technically complex procedures in pediatric surgery, yet there are very few opportunities for surgeons to practice it,” said Payam Saadai, an associate professor of surgery at UC Davis Health. He had the initial idea for a training model.
One of the biggest benefits of fetoscopic repair over similar treatments for spina bifida is that it allows the mother to have a vaginal delivery in the future, due to its minimally invasive nature.
From idea to rough sketch to fully realized tool
Saadai passed his idea on to laboratory supervisor Christopher Pivetti and surgical research resident Elizabeth Reynolds, who both work in Professor of Biomedical Engineering and Surgery Aijun Wang’s lab at Aggie Square in Sacramento. Aggie Square is UC Davis’ innovation district where researchers, industry professionals and entrepreneurs work side by side.

Also at Aggie Square, on the first floor of the district’s flagship building is Tech Foundry, a 7,500-square-foot device development facility. This set up an ideal situation to collaborate.
Pivetti and Reynolds were interested in Saadai’s idea. They sketched out notes and diagrams on graph paper, then brought them to Tech Foundry to see if they could bring the idea into reality.
For Valerie Quiroz, the development engineer who took on the project, the sketch was all she needed. She transformed the sketch and medical jottings into a working prototype featuring 3D-printed, silicone-cast and laser-cut components.
A Teaching Model
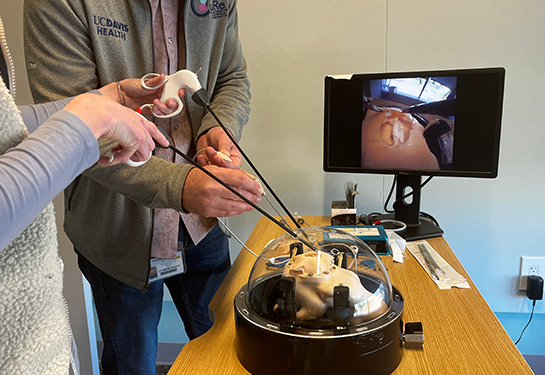
The model simulates a fetus suspended in amniotic fluid inside the uterus. It features a chamber that can be filled with liquid and holds a small doll. It also includes a dome with small holes through which laparoscopic instruments can fit.
On the backside of the doll is a raised area of skin, almost like a balloon. This is to mimic fetal myelomeningocele, the most severe form of spina bifida. It’s when the fetus’s spine and spinal canal remain open at the bottom of the spinal column, creating a bulge of skin.
“The raised area will be a consumable part that will be replaced for the next user,” Quiroz said. “[It] is intended to mimic multiple layers of tissue, such as skin, dura mater and placode, and allow surgeons to practice surgical techniques, including suturing.”

Due to the small area of skin on the fetus, and the fine laparoscopic tools, fetoscopic repair is one of the most technical and delicate pediatric procedures. With the new teaching model, pediatric surgeons at UC Davis Health can now practice and perfect the technique for treating spina bifida before ever entering the operating room.
“The fetal operation requires technical precision and is only available at a few centers in the world,” Saadai said, “so the fetal model directly supports this work by creating a safe, reproducible environment where our team can train and refine these techniques, dramatically shortening the learning curve for such a complex operation.”

Advancing the CuRe
Thanks to the teaching model, fetoscopic surgery will be an option alongside the CuRe trial at UC Davis Health. The CuRe Trial, or Cellular Therapy for In Utero Repair of Myelomeningocele, is a groundbreaking treatment using a stem cell patch to repair spina bifida tissue.
The trial is led by Wang and Distinguished Professor and chair of the Department of Surgery Diana Farmer , with Pivetti, Reynolds and Saadai as members of the clinical research team. The trial is a world first and was recently found to be safe in a paper published in The Lancet, but requires invasive surgery.
“For the CuRe Trial, we use an open surgical approach to treat the fetus, meaning we make a larger cut on the uterus and float the baby's defect to that opening for repair. The disadvantage to this approach is that these moms cannot have a standard vaginal delivery again,” Pivetti said.
Pivetti explained that the training model will be used in the next stage of the CuRe trial. The goal is to replace the open surgery with a minimally invasive fetoscopic surgery. During the procedure, a surgeon would administer the small stem cell patch with laparoscopic tools before closing the incision to allow the tissue to regenerate.
“By developing not just fetoscopic techniques but also the training infrastructure, which we have never had at UC Davis before, we position our health center as one that is advancing the next generation of both fetal therapy and surgical innovation,” Saadai said.