Skull Base Surgery
Our internationally recognized experts are skilled in the latest skull base surgical techniques. We provide compassionate, whole-person care.
Medically reviewed by Kiarash Shahlaie, M.D. on July 14, 2025.
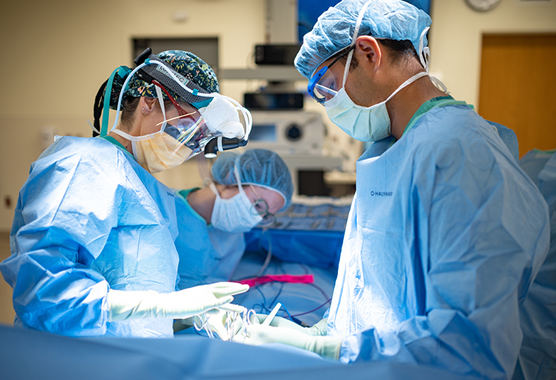
About Skull Base Surgery
At UC Davis Health, we offer expert care for people with tumors and other conditions affecting the base of the skull. This area is delicate and challenging to reach, so treatment requires advanced skill. Our team uses the latest techniques to perform surgery safely and effectively.
We understand how overwhelming it can feel to face skull base surgery. We’re here to guide you through every step with care and compassion. Our team includes specialists in ear, nose, and throat (ENT), neurosurgery, and other fields who work closely to create a personalized treatment plan for you.
Minimally Invasive Skull Base Surgery
We use advanced tools like 3D imaging, virtual reality, and robotics to plan and perform skull base surgery with precision. Our less invasive techniques mean shorter surgery, less pain, and faster recovery for you. Minimally invasive surgeries we perform include:
Endoscopic Endonasal Surgery
We perform skull base surgery through the nose with the assistance of a tiny camera, avoiding large incisions and protecting your brain.
Retrosigmoid Keyhole Surgery
We remove skull base tumors through a small opening behind the ear, avoiding large skull openings and protecting nerves.
Supraorbital Keyhole Surgery
We remove tumors through a small incision near your eyebrow, protecting your brain and reducing complication risks.
Request an Appointment
As Sacramento's No. 1 hospital, you'll benefit from unique advantages in primary care and specialty care. This includes prevention, diagnosis and treatment options from experts in 150 specialties.
Referring Physicians
To refer a patient, submit an electronic referral form or call.
800-4-UCDAVIS
Patients
Call to make an appointment.
Consumer Resource Center
800-2-UCDAVIS
Our team will guide you through every step, so you know what to expect before, during, and after surgery. We'll answer your questions, explain the process, and ensure you feel supported and informed.
-

Before Surgery
You may need imaging or lab tests to help us plan the safest and most effective approach. Your surgeon will tell you when to stop eating, drinking, and taking medications, and any other surgery preparation steps.
-
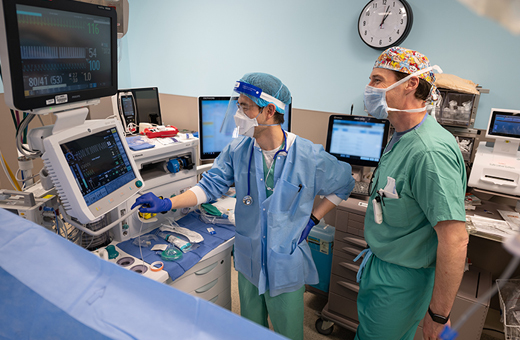
During Surgery
Our team uses advanced tools during surgery to safely reach the treatment area while protecting nearby nerves and brain tissue. You’ll be asleep under anesthesia, and we’ll closely monitor you the entire time. For tumor surgery, we aim to remove as much of the tumor as possible while minimizing risks.
-

After Surgery
After surgery, you’ll wake up in a recovery area where we’ll carefully monitor your breathing, comfort, and vital signs.
Our team will check your progress often and make sure you’re as comfortable and supported as possible. You’ll recover in the hospital for up to a week.
Home Care After Skull Base Surgery
Recovery at home usually takes several weeks, depending on your surgery type and overall health. You may need follow-up tests, additional treatments, and rehabilitation therapy. We’re here for you as you recover. Our goal is to help you feel your best.
Taking Pain Medication
You may receive prescription medication for pain. Follow your care team's instructions for all medications, including those you took before surgery.
Returning to Activity
You’ll slowly return to your normal activities. You can begin walking after you return home. Your care team will tell you when it’s safe to resume other activities.
Follow Up Care
You will have routine follow-up appointments with our surgical team. Most patients are followed for years after surgery, with repeat MRI scans and physical examinations.
When to Contact Your Surgeon
Call us if you have symptoms such as fever, heavy bleeding, or fluid draining from your nose, severe headaches, neck stiffness, or vision changes. Don't hesitate to contact your surgeon about any symptoms that are concerning.

Ranked among the nation’s best hospitals
A U.S. News & World Report best hospital in cardiology, heart & vascular surgery, diabetes & endocrinology, ENT, geriatrics, neurology & neurosurgery, and pulmonology & lung surgery.

Ranked among the nation’s best children’s hospitals
U.S. News & World Report ranked UC Davis Children’s Hospital among the best in pediatric nephrology, orthopedics*, and pulmonology & lung surgery. (*Together with Shriners Children’s Northern California)

Ranked Sacramento’s #1 hospital
Ranked Sacramento’s #1 hospital by U.S. News, and high-performing in aortic valve surgery, back surgery (spinal fusion), COPD, colon cancer surgery, diabetes, gynecological cancer surgery, heart arrhythmia, heart failure, kidney failure, leukemia, lymphoma & myeloma, lung cancer surgery, pacemaker implantation, pneumonia, prostate cancer surgery, stroke, TAVR, cancer, orthopedics, gastroenterology & GI surgery, and urology.

The nation’s highest nursing honor
UC Davis Medical Center has received Magnet® recognition, the nation’s highest honor for nursing excellence.

World-class cancer care
One of ~59 U.S. cancer centers designated “comprehensive” by the National Cancer Institute.

A leader in health care equality
For the 13th consecutive year, UC Davis Medical Center has been recognized as an LGBTQ+ Healthcare Equality Leader by the educational arm of America’s largest civil rights organization.
Latest Neurological News
-
MARCH 25, 2026
New pathway links HBCU students to research careers
-
MARCH 11, 2026
UC Davis Health named a Center for Comprehensive MS Care
-
MARCH 09, 2026
Why one family named their baby after a neurosurgeon
-
MARCH 05, 2026
Daylight saving time: More migraines, less deep sleep

