Rapid whole genome sequencing leads to better outcomes for babies, lower medical costs
UC Davis Children’s Hospital was one of five participating hospitals statewide in California’s Project Baby Bear
The evidence is in: A state-funded Rapid Precision Medicine program led by Rady Children’s Hospital-San Diego yielded life-changing outcomes for critically ill infants at five California hospitals while significantly reducing health care costs. UC Davis Children’s Hospital and the UC Davis Mind Institute were key participants in the research.
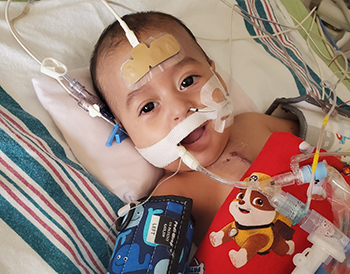
A study published today in the American Journal of Human Genetics outlined the success of Project Baby Bear, a real-world quality improvement program designed to test the clinical and economic value of using rapid Whole Genome Sequencing (rWGS ®) to diagnose and guide treatment for infants with unexplained rare disease.
Employing the most comprehensive diagnostic testing available, Rady Children’s Institute for Genomic Medicine used rWGS to analyze the genetic code of 184 infants in intensive care who were covered by Medi-Cal. The results provided doctors and families with vital information that empowered them to make life-altering medical decisions resulting in shorter hospital stays, targeted personalized care and fewer costly, invasive procedures.
“It’s very rare to be able to use the most advanced medical technology to both improve a child’s life and save money, yet Project Baby Bear proved it’s possible,” said David Dimmock, senior medical director of the institute. “We identified the exact cause of rare, genetic diseases in an average of three days, instead of the four to six weeks standard genetic testing offers. This allowed physicians to deliver timely treatment tailored to the baby’s specific condition, in some cases avoiding irreversible health consequences.”
Rapid WGS proved to be a valuable tool in clinical decision-making. Among the infants sequenced, rare genetic diseases that explained the baby’s admission to intensive care were diagnosed in 74 babies, or 40%.
Guided by the vital information provided by rWGS, clinicians were able to provide precision medicine that changed care for 58 babies, or 32%. Conclusive diagnosis allowed doctors to make treatment plans with more confidence. Results from genome sequencing also empowered parents to join physicians in making informed care decisions.
“The study highlights the importance of using state-of-the-art rapid genome sequencing technology in our most vulnerable population – neonates and acutely sick infants from historically underserved communities – to provide precision medical care based on accurate diagnosis,” said Suma Shankar, director of the UC Davis Precision Genomics Clinic and co-lead of the UC Davis site for Project Baby Bear.
“Many families felt relief in knowing and understanding the cause for their baby’s illness and the ability to receive cutting edge therapies based on receiving rare specific diagnosis early on in the course where timing is crucial to prevent long term disability,” said Shankar, who is also a UC Davis MIND Institute faculty member.
In addition to changes in treatment, rWGS resulted in avoidance of other costly procedures such as tracheostomies or gastric tube insertions, eliminated the need for further testing and led to fewer days in the hospital.
“These findings show that rWGS should be considered early for infants admitted to intensive care when the cause of the child’s condition is unknown.” said Patrick Frias, president and CEO of Rady Children’s Hospital. “Project Baby Bear has demonstrated that it’s feasible and effective to use rWGS to inform precision medicine for the most vulnerable infants; it achieves both improved health outcomes and cost savings.”
Project Baby Bear was funded by the State of California as a $2 million Medi-Cal pilot. Participation was limited to acutely ill babies enrolled in Medi-Cal who were admitted to intensive care between November 2018 and May 2020.
Patient blood samples were sent to RCIGM for sequencing and interpretation from regional neonatal and pediatric intensive care units at the following participating hospitals: UC San Francisco Benioff Children’s Hospital Oakland; UC Davis Children’s Hospital (Sacramento); Valley Children’s Hospital (Madera); CHOC Hospital (Orange County) and Rady Children’s Hospital–San Diego.
Encouraged by the early success of Project Baby Bear, the State of Florida and State of Michigan have since initiated their own publicly funded rWGS demonstration projects.
The California Legislature is currently considering adopting AB114, the Rare Disease Sequencing for Critically Ill Infants Act, introduced by Assemblymember Brian Maienschein (D-77). Also pending is a federal bill, Ending the Diagnostic Odyssey Act, introduced by San Diego Congressman Scott Peters (D-52).
The study referenced in this release is: "Project Baby Bear: Rapid Precision Care Incorporating rWGSin 5 California Children’s Hospitals Demonstrates Improved Clinical Outcomes and Reduced Costs of Care" (AJHG-D-21-00121R1) The American Journal of Human Genetics. DOI: 10.1016/j.ajhg.2021.05.008.
Related links
UC Davis Children's Hospital joins program to test critically ill newborns