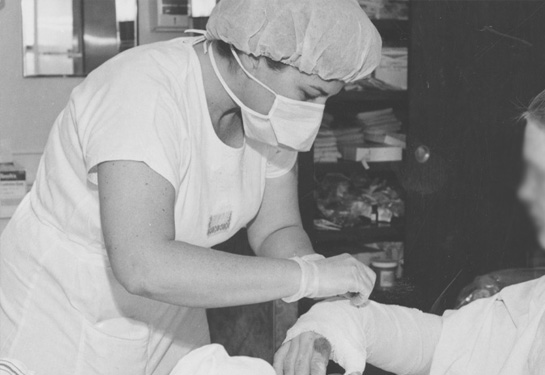
Advances in burn care after deadly plane crash lead to better survival rates
Quality of life for burn survivors improves
This story is part two in a three-part series commemorating the Farrell’s Ice Cream Parlour crash in Sacramento in 1972, and the subsequent nationally recognized burn center expertise that resulted from the tragedy.
Part one: Fiery crash 50 years ago spurs today’s world-class burn care
Part three: Support and resources for burn survivors result of tragic plane crash 50 years ago
When an out-of-control plane slammed into Sacramento’s Farrell’s Ice Cream Parlour in September 1972, the region was not well prepared to treat the dozens of burn victims from the ensuing fire.
The nearest burn center was nearly 400 miles away at UCLA. A smaller burn unit was roughly 90 miles away in San Francisco.
“In the aftermath of the fire, people learned there was no resource to handle an event like that,” said Joe Pick, executive director of the Firefighters Burn Institute.

The institute was a silver lining that resulted from the crash that left 22 people dead and 25 in need of specialized treatment for their traumatic injuries. From the ashes of the wreckage came a dedicated center for burn treatment at UC Davis Health, transforming the regional response to burn care. For more than 48 years, it has offered the highest-quality treatment and recovery for severely burned patients from throughout Northern California and greater hope for their families.
“Those injured in 1972 were taken to local hospitals, where surgeons did their best to treat them, but unfortunately they had very limited knowledge of burn care,” said Tina Palmieri, a surgeon and chief of the Firefighters Burn Institute Regional Burn Center at UC Davis Medical Center. “Their initial treatment would have been to assess them for traumatic injuries and burns.”
Defining quality burn care
Since its launch in 1974, the UC Davis Burn Center has been one the nation’s top programs for burn care, research and training. Its mission and reputation have greatly expanded over the past four decades. Burn treatment involves many components, from initial first aid and assessment of the degree of the burn to wound excision, grafting and infection control.
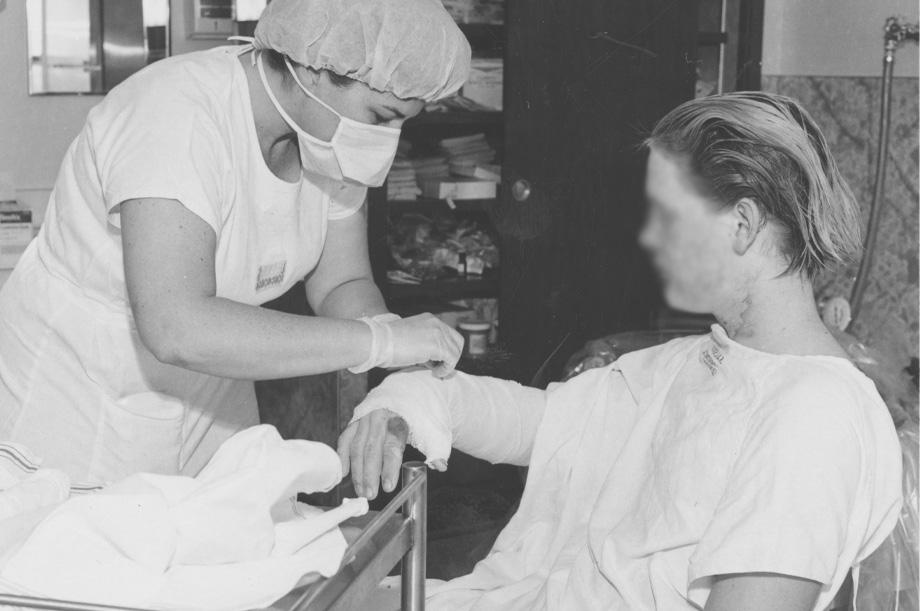
According to a national study, “the last 50 years has seen a tremendous improvement in the advancement of burn treatment with a significant reduction in mortality which can be attributed to the developments in early burn excision, early fluid resuscitation, infection control and nutrition.”
Palmieri credits mortality reduction to the advent of burn center triage criteria, including burn degree, percentage of body surface area and patients who require special social, emotional or long-term rehabilitation intervention.
“We also use new methods for mechanical ventilation and resuscitation for those critically injured,” she explained. “The burn field continues to expand its knowledge about burn injury, particularly with respect to artificial skin, stem cells and cultured skin.”

What has also helped treatment is the physical space in which teams care for patients. In 2010, the burn unit moved into its current location — triple the size of its former space — consolidating into a single location and accommodating more patients.
The move created individual rooms for patients, which has improved the survival rate, since the leading cause of death among burn victims is infection. Since many survivors require months of care, the new rooms also included windows, which helps with emotional health. And because the improved capabilities were the direct result of an additional $1 million raised by area firefighters, the move ushered in a new name — the Firefighters Burn Institute Regional Burn Center.
“Merely surviving a burn is not good enough,” Palmieri said. “Our goal is to return our patients to a meaningful life.”.
In 2021, the team received re-verification as an Adult Burn Center from the American Burn Association (ABA) for meeting the highest standards of care for burn-injured patients. Fortunately for children, whose burns present a unique challenge, expert care is across the street.

No burn too small
The Shriners Children’s Northern California also credits the deadly crash in 1972 for its inception 23 years later.
Burn surgeon David Greenhalgh built that program from the ground up. Although he retired in February 2022, after more than 25 years as a leading burn surgeon at UC Davis Health, he continues to oversee the program and his patients at Shriners Children’s. He is guided by the motto: “there is never a burn too small for us to treat.”
Young burn patients face more serious risks than adults, in part because toddlers explore with their hands and mouths and get burned, he said. "Small children with big burns can be very uncomfortable due to their injuries — even in the burn center."
Greenhalgh credits the entire team of physicians, nurses, therapists and dietitians who work in tandem to closely monitor patients in the hospital and provide follow-up care after being discharged.
I’m grateful that the firefighters long ago had the foresight to support a burn program.—David Greenhalgh, Shriners Children’s and UC Davis Health (retired) burn surgeon
Bracing for the next emergency
The UC Davis Burn Center team can quickly leverage resources in burn management, surgery, trauma and intensive care to treat a range of burn-related injuries. And with increased expertise and need, the volume of those for whom they care has increased as well. In 1997 before Shriners Children’s opened, the UC Davis Burn Center admitted 180 patients. Last year, the number of patients admitted for treatment between the two centers quadrupled to approximately 750.
Part of that growth is due to the increasing numbers and size of major wildfires in Northern California. As the only burn center in a vast region, UC Davis Health takes on a mission and responsibility to being prepared for and focused on the needs of burn patients. The next nearest centers are in the Bay Area, Fresno, Las Vegas, Salt Lake City and Portland.
Over the years, the center's surgeons, nurses and rehabilitation specialists have been on the front lines of treating patients injured by wildfires. They regularly practice their response plan for large-scale fires with multiple victims and collaborate with other burn centers throughout the western U.S.
“We’ve been affected by so many big fire events in recent years that we have to assume another one is coming,” said Len Sterling, the burn center’s nurse manager. “We want to be nimble, flexible and treat all patients who need us.”

Remaining challenges, awaiting support
Despite the success of treating burn survivors, many challenges remain, especially as people live longer. The focus of burn care in the future includes treating the elderly, caring for those with extensive burns, increasing the quality of the lives saved by shortening healing times and hospital stays and finding more ways to reduce scarring.
“It’s hard to push the survival of the youngest burn victims any higher. But we’ve made great strides in the elderly,” Greenhalgh said. “When I first started in burns, we wouldn’t bother to resuscitate 60-year-olds with 60% burns. But we’ve made the greatest improvements in this population because of better wound coverage and critical care.”
Palmieri added, “Quality of life has become the priority for most people who are burned, as we can save most people. For the very young and the very old, however, improving survival is still a major priority.”
Support for all victims, young or old, is critical.
Beyond the expertise of the surgery team and UC Davis Health are experts who provide resources and peer support that bring hope and inspiration to patients and their families.
Had a burn center like today’s existed 50 years ago, the UC Davis team agrees, the victims would have had a greater chance of not only surviving but living more functional lives.
“I’m grateful that the firefighters long ago had the foresight to support a burn program,” Greenhalgh added. “I’m proud to say we were able to work with them -- and we have one of the best programs in the country.”