A dose of hope: One year after the COVID-19 vaccine’s arrival, everything has changed
UC Davis health care workers reflect on the relief and excitement and look ahead to a post-pandemic future
Of all the milestones over the past two years, none stands out quite like Dec. 15, 2020 for UC Davis Health. On that day, the first doses of Pfizer-BioNTech COVID-19 vaccine arrived at UC Davis Medical Center.

It changed everything.
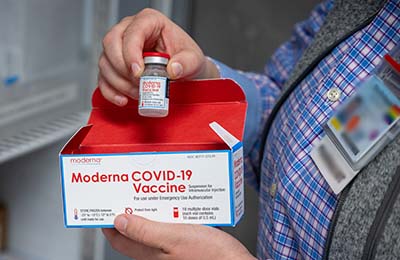
“The day was high anticipation,” said Chad Hatfield, chief pharmacy officer at UC Davis. “We didn’t know exactly when the vaccine was going to get there, but I had a tracking number from FedEx and finally got a confirmation that it was coming that morning.”
UC Davis Health was among the nation’s first health systems to receive an initial allotment of the vaccine, due largely to its storage capability, high at-risk population and ability to distribute shots quickly to the community.
The 4,875 doses arrived shortly after 7 a.m. Hatfield was outside on that cold morning, waiting at the loading dock to accept the life-saving shipment. After the box was wheeled in, Hatfield and his team got to work.
This Washington Post video features Hatfield and highlights the vaccine’s arrival.

“We brought it into the central pharmacy, unpacked it from the dry ice and loaded it into the negative 80 freezer and from there we immediately started to unthaw them and send them to our vaccination site,” he said.
That’s where clinical nurse Eva Teniola was waiting, along with a group of other emergency department employees. They included doctors, nurses, respiratory therapists, staff who clean rooms, food service workers and reception staff who greet patients. Within three hours of the vaccine’s arrival, inoculations began.
The first COVID-19 shots
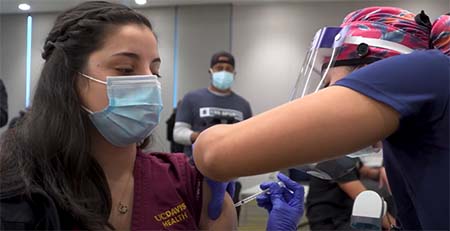
Teniola was the first to get her shot – and UC Davis Health was the first system in the region to start vaccinating its employees. She was ready.

“Honestly, looking back at Dec. 15, I didn’t feel nervous at all,” Teniola said. “All I could feel was relief, excitement and hope. I was thankful that the day had finally come, for I had prayed for and been waiting for a COVID vaccine.”
Upon receiving her injection, Teniola thrust her arms into the air in celebration – an image that was widely circulated and made its way to California Department of Public Health advertisements promoting the arrival of vaccines.
Teniola reflects that life has changed a lot in the year since. “I am most confident that I am protecting my patients, myself and my loved ones. I am less fearful. People outside the medical field may not realize how amazing it is to see the decrease of COVID cases since the vaccine rollout. It is impressive!”
#amazing #mood at the @UCDavisMedCntr #CovidVaccine site this morning: #smilingFaces (under masks of course), extra #energy--we can get through #COVID19 #pandemic. dose 1 ✔ pic.twitter.com/wX4h4KRqw1
— Dean Blumberg (@DBlumbergPedsID) December 16, 2020
It’s easy to forget, now that vaccine supply is plentiful, that just a year ago it was frustratingly limited. At the time, UC Davis Health had developed priority tiers to ensure the vaccine was distributed equitably among employees in the hospital.
Dean Blumberg, chief of pediatric infectious diseases at UC Davis Health, vividly remembers walking over to the North Addition Office Building for his shot when he became eligible.
“As I got closer to the vaccination site, there was a different mood. There was a bounce in people’s step and this electricity in the air, this positive mood. I didn’t understand it, but when I got there, I had a real emotional reaction, and I thought, this is the beginning of the end of the pandemic,” Blumberg reminisced.
He added: “I’m not an emotional person at all and it almost brought tears to my eyes – even remembering it now, I feel sort of emotional about it.”
As I got closer to the vaccination site, there was a different mood. There was a bounce in people’s step and this electricity in the air, this positive mood. I didn’t understand it, but when I got there, I had a real emotional reaction, and I thought, this is the beginning of the end of the pandemic.” —Dean Blumberg
Nearly 1,000 COVID-19 shots a day
UC Davis Health began vaccinating health care workers as quickly as Hatfield’s team could deliver the doses to the building’s auditorium.
“It was a mad, mad rush,” explained Ann Tompkins, director of employee health. “We operated from 5 in the morning until 10 at night and we worked seven days a week. Those first few days, we were vaccinating about 700 to 800 people as more vaccine was available – we were in the high 900s daily. We almost got to a thousand in one day.”
The extended hours allowed UC Davis Health to accommodate night shift workers and others on a variety of schedules.
On December 22, 2020, the first shipment of Moderna vaccine arrived, bolstering supplies. And within just a few weeks, UC Davis Health had vaccinated roughly 80% of its front-line health care workers.
“It was unbelievable, the excitement and the energy around that, because we were starting to see the end, the light at the end of this tunnel,” said Carla Martin, director of patient care services.
A study published in August by UC Davis Health infectious diseases specialists found that employee vaccination efforts significantly reduced transmission among health care workers.
How the COVID-19 vaccine changed lives and health care
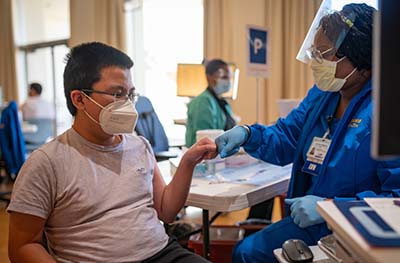
On Jan. 12, UC Davis Health began vaccinating its patients and the community, beginning with older adults who were most at risk of severe complications from COVID-19. By Feb. 21, over 50,000 shots had been delivered.

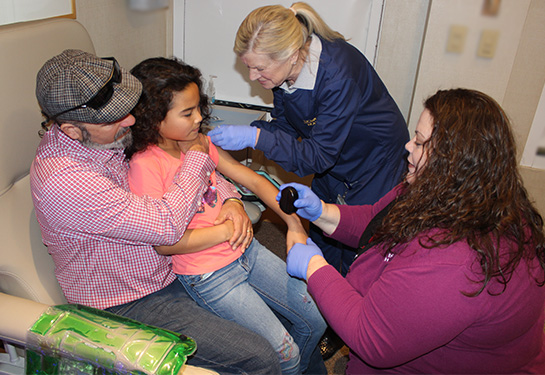
In May, the FDA expanded authorization to those ages 12-15, and in November, ages 5-11 were added.
“Absolutely, it was the beginning of the end of the pandemic,” asserted Blumberg. “Sure, we’re not out of it. We’ve had all these surges, we continue to have challenges with variants like Delta and now Omicron, and there are still more questions than answers. But now, the vast majority of people have at least partial immunity from either vaccination or previous infection, so that when breakthrough infections happen, most people won’t end up in the hospital or die,” he explained.
Blumberg notes that unlike last year, he’s visiting with family over the holidays and having dinner with fully vaccinated friends. “And,” he laughed, “we’ve got plenty of toilet paper, too.”
Eva Teniola is also enjoying seeing and hugging relatives. “It brings joy to my heart to see kids going back to school with real socialization and play, getting to travel again, and most of all fewer deaths from COVID in my emergency department and seeing my colleagues with less fear and strain in their eyes. Be encouraged,” she exhorted.
I think all of our locations went off without a hitch. You’d never know the bumps in the road and tight deadlines that we pulled through,” Hatfield said. “That’s pretty powerful as I look at my teams and other teams we’ve worked with through the health system. It’s been pretty cool to watch.” —Chad Hatfield
Hatfield, who noted that a year ago, COVID-19 vaccination management was taking nearly 100% of his team’s time, explained that now it’s about 15%. “But that 15% is relentless and constant. The logistics, data management and documentation required for the COVID vaccine are pretty involved,” he explained.
But it’s also been rewarding: “We are part of a group that’s making a true difference in society,” he said, “so that’s always been a very pleasurable side of the whole experience.”
Infectious diseases specialist Dean Blumberg notes that several key things have changed over the past year that make him optimistic:
- Anyone over age 5 who wants the vaccine can get it
- There’s no shortage of vaccine supply
- There are protocols for treating patients with COVID-19
- Monoclonal antibodies are now available for some patients
- Concerns about hospital capacity and staff have diminished
- Anyone can get tested for the virus – there’s no shortage of diagnostics
“It’s so much different than it was last year. We’re so much more prepared to deal with it – largely because so many people are now vaccinated,” Blumberg said.
UC Davis Health has administered more than 210,000 doses of COVID-19 vaccine.
Check out this timeline that covers the events of the past two years, from the first case of community-spread COVID in the nation at UC Davis Health to the expansion of the vaccine to younger age groups and the discovery of the Omicron variant.
Looking to a post-pandemic world
“A year from now, we’re going to be post-pandemic,” predicted Blumberg. “We’re still going to have COVID, but it’ll be very similar to influenza in terms of people making their own risk assessments.”
Blumberg notes there is still more to be learned about the optimal vaccine schedule, in terms of how far apart shots should be given and whether boosters will be necessary annually.
He expects vaccine hesitancy to continue but thinks vaccination rates will keep climbing. “At this point in the pandemic, there have been more than 8 billion doses administered worldwide. It’s been so intensely studied and so widely used.”
Eva Teniola encourages anyone who hasn’t yet gotten vaccinated to do so. “I am so thankful that we have the vaccine and continue to plead that we remain vigilant with what we do to protect each other. There are still unvaccinated people out there, and I hope not to see you in my emergency department, but if you do end up here, I will take good care of you,” she said.
For Hatfield, a major focus has been ensuring that vaccine supply is widely available. “We’ve changed our strategy from mass vaccination sites to more remote locations and clinics and that involves a different set of logistics.”
He adds that UC Davis Health continues to reach out to rural areas and the underserved. “We’ll continue to support those mobile vans and pop-up clinics, getting the vaccine out to the communities that need them,” he said.
“I think all of our locations went off without a hitch. You’d never know the bumps in the road and tight deadlines that we pulled through,” Hatfield said. “That’s pretty powerful as I look at my teams and other teams we’ve worked with through the health system. It’s been pretty cool to watch.”
Learn how to schedule your vaccine at UC Davis Health
UC Davis Medical Center is a comprehensive academic medical center where clinical practice, teaching and research converge to advance human health. Centers of excellence include the National Cancer Institute-designated UC Davis Comprehensive Cancer Center; the region's only Level 1 pediatric and adult trauma centers; the UC Davis MIND Institute, devoted to finding treatments and cures for neurodevelopmental disorders; and the UC Davis Children's Hospital. The medical center serves a 33-county, 65,000-square-mile area that stretches north to the Oregon border and east to Nevada. It further extends its reach through the award-winning telemedicine program, which gives remote, medically underserved communities throughout California unprecedented access to specialty and subspecialty care. For more information, visit medicalcenter.ucdavis.edu.