Boy with ruptured, near giant, partially thrombosed ACOM aneurysm makes excellent recovery
On the day that 13-year-old James collapsed, he gave his parents a hug and a kiss and headed to his first-period class. It was an ordinary day in April 2022.
But minutes later, he was unresponsive on the playground. An ambulance transported James to UC Davis Children’s Hospital.
A CT scan would reveal that James had a ruptured, near giant, partially thrombosed ACOM aneurysm. Treatment was required.
Preparing for surgery
There were no signs or symptoms beforehand. He was healthy and had never had headaches. He had no genetic predispositions that his family was aware of.
But James had brain surgery scheduled the next morning.
“He was sedated, intubated on a ventilator, and they gave him a lot of medication so his blood pressure stayed low. Then it was just a waiting game, hoping he would make it through the night,” said Bryan Gast, James’ father.
UC Davis neurosurgeon Ben Waldau had two options. He could clip the aneurysm, or he could use a coiling procedure, in which a coil was inserted via catheter through the groin. He would position the catheter in the aneurysm and direct the coil through the catheter into the aneurysm.
“Coiling or flow diversion embolization of this aneurysm may have failed since near giant pediatric aneurysms may have unstable walls and may keep expanding despite endovascular treatment techniques,” Waldau said.
Waldau hoped he could clip the aneurysm, but he wouldn’t know what was possible until James was on the operating table. And then, Waldau faced another challenge.
Once in surgery, Waldau initially thought he could not approach the aneurysm because James’ intracranial pressure (ICP) was elevated, and his brain was significantly swollen which blocked the surgical corridor to the aneurysm.
Additional medication and changes in head positioning were required to help bring the swelling down to make the approach possible.
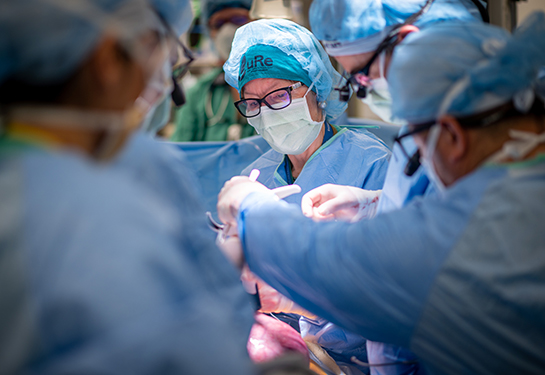
“We were then able to approach the aneurysm using our standard brain relaxation techniques and place a clip across the neck, which led to complete exclusion of the aneurysm from the circulation. There was no residual on a follow-up diagnostic cerebral angiogram six months later,” Waldau said.
James underwent a hemicraniectomy for high ICP several days later. A cranioplasty was conducted about two months later by pediatric neurosurgeon Marike Zwienenberg.
A bright future
James was discharged from the hospital after 52 days. He continues to make great strides. He has relearned to ride a bike and takes piano lessons. He has gone back to the rock-climbing gym, a pastime he enjoyed before his world changed so drastically.
James was able to return to school full-time for his eighth-grade year. James continues to have regular neurosurgery appointments with Waldau. His parents still stay in touch with members of his care team to provide updates on his many “firsts” — including getting out of bed without a helmet, first swim, first time riding a bike and first day of school.