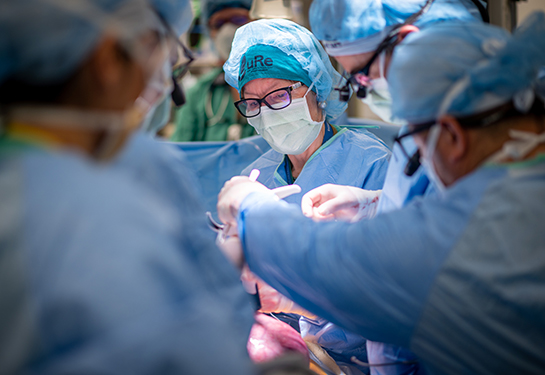
Preventing hospital readmissions following TAVR procedures
Why are some patients more prone to rehospitalization after transcatheter aortic valve replacements (TAVRs)? To answer that question, UC Davis Division of Cardiovascular Medicine researchers examined intermediate and high-risk patients undergoing TAVR between 2012 and 2018 and found a complex mix of causes. In addition to possible complications from the procedure, higher-risk patients faced chronic health issues that could lead to rehospitalization. Their findings were published in Catheterization and Cardiac Interventions.
“Many of the patients we care for with aortic valve disease have other health problems,” said interventional cardiologist Jeffrey Southard, clinical professor and senior author of the study. “Unfortunately, fixing aortic valve stenosis does not cure everything. Patients feel better and have improved quality of life, but we have to be attuned to all of their medical problems to keep them out of the hospital and feeling well.”
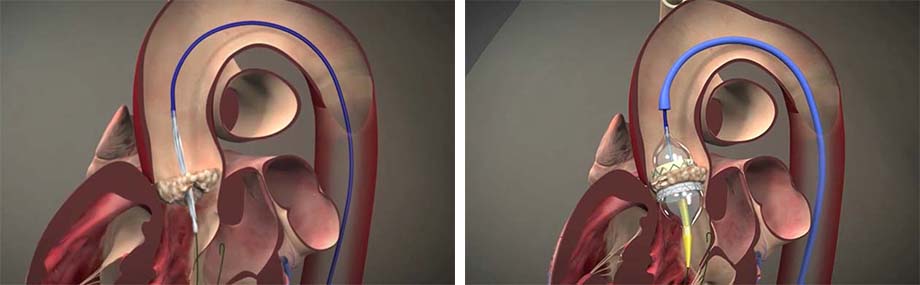
TAVR is a minimally invasive procedure to replace a malfunctioning and stenotic aortic valve and implant a new one. Until recently, it was only indicated for patients deemed too sick for open surgery. These patients frequently have diabetes, high blood pressure, chronic kidney disease, chronic lung disease or are obese.
TAVR is now available for most patients with severe symptomatic aortic stenosis but requires discussion with a team made of surgeons and cardiologists to help determine the best course for the patient now and in the long term.
This was the first study to examine rehospitalizations for both high and intermediate risk TAVR patients.
These patients tend to have a lot of other conditions. This research is helping us identify which of those issues might bring them back to the hospital. We are also adjusting our approach to treat patients’ comorbid conditions more aggressively in an outpatient setting. By keeping them at home and out of the hospital, we improve our patients’ quality of life and reduce healthcare costs.” —Jeffrey Southard, interventional cardiologist
The reasons behind readmissions
The study followed 611 TAVR patients for one year after their procedures, identifying 410 who had no readmissions and 201 who had one or more. Overall, there were 317 readmissions: 36% for cardiovascular issues and 64% for non-cardiovascular problems.
The most common cardiovascular causes were heart rhythm abnormalities, bleeding and stroke. While the high-risk patients were admitted more often, both high and intermediate risk patients returned for similar reasons.
Patients readmitted in the first month after their TAVR often experienced cardiovascular problems, possibly associated with their procedure. Fortunately, a number of technological and procedural refinements have dramatically reduced the complications associated with TAVR, including access site bleeding and the need for a permanent pacemaker. Heart rhythm issues, bleeding and stroke incidence are now much lower than they were during the study period (2012 to 2018), helping reduce readmissions within the first month.

Those who were readmitted after a month often had non-cardiovascular issues. Some came in for lung-related problems, urinary tract infections or other conditions not related to the procedure.
Many of these patients live several hours away from their treating cardiologists at UC Davis. Out of an abundance of caution, primary care doctors and referring cardiologists, who are not familiar with the procedure, would send their patients back to UC Davis rather than treating them locally This is understandable with a new procedure.
“As cardiologists, we need to pay close attention to the issues that bring patients back within the first month,” Southard said. “We must also ensure that patients’ other medical problems are being cared for by their local doctors, and that we communicate well with them.”
To prevent potentially unnecessary trips to the hospital, the UC Davis cardiology team stepped up education for both patients and their physicians, helping them better understand the procedure and the issues that might call for readmission.
“These patients tend to have a lot of other conditions,” said Southard. “This research is helping us identify which of those issues might bring them back to the hospital. We are also adjusting our approach to treat patients’ comorbid conditions more aggressively in an outpatient setting. By keeping them at home and out of the hospital, we improve our patients’ quality of life and reduce healthcare costs.”
The study was published in the journal Catheterization and Cardiovascular Interventions.
Coauthors included Jonathan Yap, Steven Russo, Benjamin R. Stripe and Garrett B. Wong, all of UC Davis.