Western diet rich in fat and sugar linked to skin inflammation
A Western diet rich in fat and sugar may lead to inflammatory skin diseases such as psoriasis, a study by UC Davis Health researchers has found.
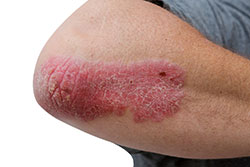
The study, published today in Journal of Investigative Dermatology, suggests that dietary components, rather than obesity itself, may lead to skin inflammation and the development of psoriasis. A common and chronic skin disease, psoriasis causes skin cells to form scales and red patches that are itchy and sometimes painful.
Diet and Skin Inflammation
Previous studies have shown that obesity is a risk factor for the development or worsening of psoriasis. The Western diet, characterized by a high dietary intake of saturated fats and sucrose and low intake of fiber, has been linked to the increased prevalence of obesity in the world.
“In our study, we found that short-term exposure to Western diet is able to induce psoriasis before significant body weight gain,” said Sam T. Hwang, professor and chair of dermatology at UC Davis and senior author on the study.
For the UC Davis Health study, which used a mouse model, Hwang and his colleagues found that a diet containing both high fat and high sugar (mimicking the Western diet in humans) was required to induce observable skin inflammation. In four weeks only, mice on Western diet had significantly increased ear swelling and visible dermatitis compared to mice fed a controlled diet and those on high fat diet alone.
“Eating an unhealthy diet does not affect your waistline alone, but your skin immunity too,” said Zhenrui Shi, visiting assistant researcher in UC Davis Department of Dermatology and lead author on the study.
Bile Acids and Skin Inflammation
The study detailed the mechanisms by which inflammation happens following a Western diet. It identified bile acids as key signaling molecules in the regulation of skin immunity. Bile acids are produced in the liver from cholesterol and metabolized in the intestine by the gut microbiota. They play an important role in dietary lipid absorption and cholesterol balance in the blood.
The study found that cholestyramine, a drug used to lower cholesterol levels by binding to bile acids in the intestine, helped reduce the risk of skin inflammation. The finding suggests that bile acids mediate the development of psoriasis. The binding of cholestyramine to bile acids in the gut and its subsequent release through the stool allows for lowering of skin inflammation.
Further studies are needed to understand the mechanism behind diet-induced skin inflammation and the interaction between metabolism, microbes and immunity.
This study was supported by a National Psoriasis Foundation Discovery Grant, an NIH/NIAMS R01 grant (1R01AR063091-01A1) and an NCI/NIH grant (U01-CA179582-03A1).
Other collaborators include Xuesong Wu, Mindy Huynh and Mimi Nguyen from Department of Dermatology at UC Davis, Prasant Jena and Yui-Jui Yvonne Wan from Medical Pathology and Laboratory Medicine at UC Davis and Sebastian Yu from Department of Dermatology at Kaohsiung Medical University.



