8 things health experts want you to know about the Delta variant
A Sacramento-area COVID-19 surge is likely, given the highly contagious variant and the low vaccination rate
For most of June, there were fewer than 10 patients with active COVID-19 at the UC Davis Medical Center on any given day. On several days there were five or six.
This week, it’s ranged from 18-25 patients daily. And UC Davis Health experts expect that to go up.
Another COVID-19 surge
“We’re all thinking that another surge is likely,” said Christian Sandrock, director of critical care at the medical center. “It is frightening. I don’t think we’ll go back to the worst we’ve seen, due to the vaccine, but it’s hard to tell.”
The state of California re-opened June 15, lifting most masking and distancing requirements. The Delta variant, which originated in India, was spreading rapidly in the U.S. around the same time.
“The substantial increases in COVID-19 cases are consistent with a fourth surge largely, if not entirely, driven by unvaccinated people and not masking,” explained Natascha Tuznik, associate clinical professor of infectious diseases at UC Davis Health.
— Dean Blumberg
chief of pediatric infectious diseases
“It’s a concern but it’s not unexpected, given the increased transmissibility of the Delta variant in combination with opening back up,” said Dean Blumberg, chief of pediatric infectious diseases at UC Davis Children’s Hospital.
Sacramento County has the third highest COVID case rate in the state, with 11.5 cases per 100,000 people over the last seven days. The county’s COVID-19 vaccination rate is around 50%, well below the statewide rate of 63%.
UC Davis Health experts are warning that Delta should be taken very seriously. Here’s what they’ve learned about the variant:
1. Delta is highly contagious

COVID infects an entire family, including a vaccinated UC Davis doctor
Christian Sandrock has been taking care of critically ill COVID patients since the beginning of the pandemic. The director of critical care at UC Davis Medical Center and an infectious diseases expert, Sandrock got the vaccine as soon as it was available.
But recently, he got some unwelcome news: He had COVID-19. So did his fully vaccinated wife and their two young children who were both too young for the vaccine.
“I thought I would just have a fever for a day or so and it would go away, but it’s been a bit rougher. I’ve had chest pains, a pertussis-like cough and headache. My sinuses are really a mess,” Sandrock said. “I would hate to see what it was like if I wasn’t vaccinated. It might have killed me.”
He’s pretty sure that his wife got COVID after spending time with another vaccinated person, indoors. She lost her sense of smell. His youngest children had fevers of 104 for a week. He was the last to get sick.
“All of a sudden, I just felt terrible. I could literally look at the clock and tell you the moment – with the snap of a finger, I just knew,” he said.
Sandrock says he and his family are recovering, and he’s grateful he was vaccinated. Even though he ended up with a breakthrough case, he believes the vaccine protected him from severe disease. He recommends that everyone get vaccinated – and that even those fully vaccinated still consider safety measures.
“I would recommend that people who are vaccinated still mask up indoors, because the rates are climbing,” he said.
Nearly 80% of current COVID-19 cases in UC Davis Health patients are the Delta strain.
That’s in line with what the Director of the Centers for Disease Control and Prevention, Rochelle Walensky, told a Senate committee this week: Delta accounts for 83% of the new cases in the U.S - up from about 50% just a couple of weeks ago.
“The Delta variant is 40-50% more transmissible than the Alpha variant,” said Tuznik. The Alpha variant was 50% more transmissible than the original strain of SARS-CoV-2.
2. Symptoms are the same, but cases are skewing younger
“We haven’t really seen more severe symptoms with Delta [than the other strains], but we are seeing one trend internationally: 30-50-year-olds are making up more hospital admissions,” Sandrock said.
“Symptoms are the same but what we are seeing with Delta is `quicker sicker,’ especially in younger people,” Tuznik noted. One possible explanation? Research published recently found that the variant grows more rapidly – and to much greater levels – in the respiratory tract.
3. Delta is hitting the unvaccinated
“The Delta variant in the U.S. is affecting for the most part the unvaccinated,” said Lorena Garcia, professor of epidemiology in the Department of Public Health Sciences. “That is different than the surges in winter or early spring when the vaccine was not available to everyone. Now when you combine being unvaccinated with not wearing masks and no social distancing, you see this surge during the summer.”
Most hospitalized COVID patients at UC Davis Medical Center are unvaccinated. “Vaccines continue to work very well – including against Delta,” Blumberg said. “At this point in the pandemic, you’re either going to get vaccinated or you’re going to get COVID.”
Nationally and statewide, the data show that areas with lower vaccination rates tend to have higher COVID-19 infection rates.
“My biggest concern is the unvaccinated population and ongoing refusal to vaccinate,” said Tuznik. “Vaccination works. Vaccination prevents severe COVID-19 disease, which may be fatal. Essentially all fatalities at this time are being seen in the unvaccinated.”
Learn how to schedule your vaccination at UC Davis Health.
4. Breakthrough cases are rare, but do occur
Breakthrough cases, when a vaccinated person gets COVID, do occur, but they are rare, and most are mild and don’t result in hospitalization or death. “The increased transmissibility of the Delta variant is almost certainly contributing to breakthrough cases,” said Tuznik.
“In the U.S., there have been 65,000 breakthrough cases among the 160 million people who’ve been fully vaccinated. So that’s 0.04% of the people vaccinated reporting breakthrough cases,” Blumberg noted.
For vaccinated patients who get COVID, symptoms have been largely similar to a cold, with a significant loss of smell.
“In vaccinated people who do get COVID, it’s definitely more of the asymptomatic people with limited symptoms,” Sandrock said. “They may have a couple of days of cough, fever or headache but it’s not as severe.”
No vaccine is 100% effective. With the COVID-19 vaccines averaging about 90% efficacy, health experts expect about 10% of those vaccinated could be infected. In Sacramento County, that’s 74,000 people who could get it – but are still protected from severe disease and hospitalization.
5. Many of our patients wish they’d gotten vaccinated
“A number of younger patients, when they come in to us, critically ill, they start saying ‘I should have gotten the vaccine,’” Sandrock said. “We are seeing a lot of that. As they start to get really sick, they’re like, ‘Why did I not get the vaccine? Why did I not listen?’ I’d say more than half of them do that.”
6. Delta could be catastrophic in some communities
In California’s communities with lower vaccination rates, particularly rural areas with limited access to care, Delta could be even more damaging.
— David Lubarsky, CEO, UC Davis Health
Vice Chancellor, Human Health Sciences
“It could be extremely devastating,” said Garcia. “We already have an example in what is occurring around the world in low income countries where the vaccine is not available for the poor. The preventable deaths and severe illness are overwhelming. The impact will be felt for decades to come.”
Learn about UC Davis Health’s efforts to care for and vaccinate underserved communities.
7. Some experts are still masking up after vaccination
“My advice is to continue masking. Even if you’re vaccinated, definitely avoid large indoor gatherings – begrudgingly, again – and mask in grocery stores, drug stores and other locations that don’t verify vaccination status,” said Tuznik. “Socially distanced outdoor activities should be fine, but if you might come into close contact, even briefly, with a stranger, then mask up just in case.”
“I’m fully vaccinated and I still wear a mask at the grocery store or even outdoors in a crowded situation like at the farmer’s market, because many unvaccinated people are choosing to go unmasked and I’m not comfortable with that,” Blumberg explained.
8. There are more variants to come
“We have the Delta now and then it’s being followed by the Lambda in South America,” said Sandrock. “If people want to get back to normal, they need to get vaccinated. As long as a good chunk of people are unvaccinated, in the world, we’re just going to continue having new strains come along that are going to cause these periods where we’ll have to go back and forth to a modified life.”
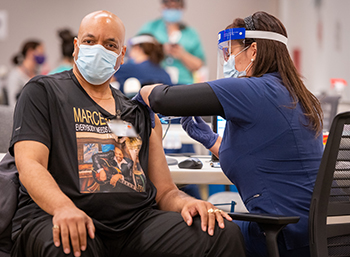
UC Davis Health has delivered more than 167,000 doses of the COVID-19 vaccine to date at its vaccine clinics, as well as schools, churches, community centers and doctors’ offices.
“We are in the middle of our own surge, with patient census is as high as it was a year ago,” said David Lubarsky, CEO of UC Davis Health. “At UC Davis Health, we are making it easy for people everywhere and in every circumstance to do the right thing and get vaccinated, so we can finally stop this pandemic. The risks are real, and as we hear every day from people who have gotten seriously ill, almost all of whom are not vaccinated, they really wish they had gotten the vaccine."
Our primary care doctors are providing the COVID-19 vaccine every day in our Midtown Sacramento clinic. There’s also weekly availability during appointments at these locations:
- Mondays in Rancho Cordova
- Tuesdays in Davis
- Wednesdays in Roseville
- Thursdays in Elk Grove
- Fridays at the MIND Institute (for individuals with neurodevelopmental conditions)



