Nursing Professional Practice Model: A Compass for Optimal Outcomes
What is a Professional Practice Model (PPM) Compass
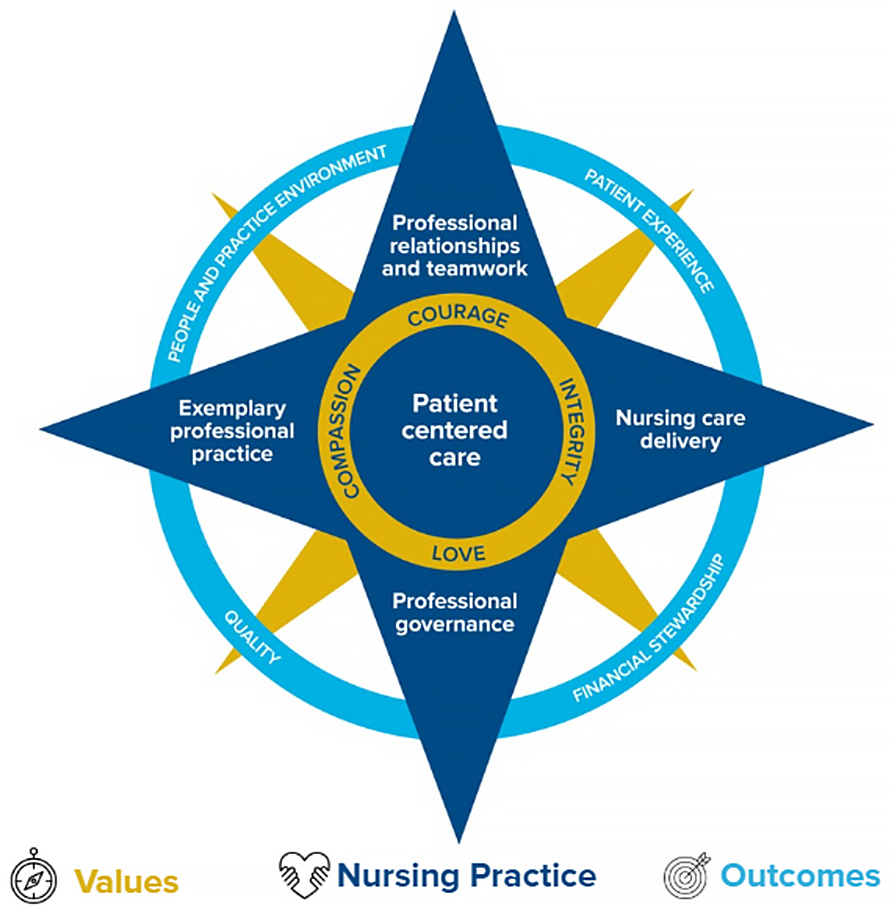
Our PPM Compass guides our nursing values, nursing professional practice with our mission to achieve optimal outcomes for patients, families, and our community. Like a compass, it provides direction and a framework for how nurses practice, collaborate, and lead while remaining focused on what matters most: achieving optimal outcomes for patients, families, and our teams.
Values
 Our nursing values are our beliefs that guide how we treat each and every patient.
Our nursing values are our beliefs that guide how we treat each and every patient.
Love – We build relationships grounded in inclusivity, patience, kindness, and gratitude. In our teams and work, we bring our whole selves in an authentic and caring spirit and encourage others to do the same.
Sympathy – We provide care with sensitivity and empathy.
Courage – We accept responsibility when faced with challenges to ensure optimal outcomes.
Integrity – Our behaviors consistently reflect the highest standards of professionalism and ethics.
Nursing Practice
Our nursing practice provides our RN’s with the steps on how exceptional care here at UC Davis Health is delivered. This is accomplished through:
- Professional Relationships and Teamwork
- Nursing care delivery
- Professional governance
- Exemplary professional practice
Professional Relationships and Teamwork
We believe healthcare works best when relationships are strong. Every aspect of care happens within human connections, and outcomes improve when we intentionally support those relationships.
Healthy relationships are built through four core practices:
- Attuning – Being fully present and aware
- Wondering – Staying curious and suspending judgment
- Following – Letting patient and team needs guide actions
- Holding – Creating a safe, respectful environment
We apply these practices across all roles, teams, and interactions.
A healthy work environment is essential for engaging in professional nursing practice and is achieved by aligning with the six standards for establishing and sustaining healthy work environments identified by American Association of Critical Care Nurses:
- Skilled communication
- True collaboration
- Effective decision making
- Appropriate staffing
- Meaningful recognition
- Authentic leadership
Nurse engagement is measured through the Press Ganey employee survey. At UC Davis Health Center, nurses report high engagement and autonomy, with strong opportunities to influence practice and act in their patients’ best interests. They value effective interprofessional collaboration, feel appreciated, and have access to ongoing professional development. We actively use this feedback to drive improvements in the work environment.
Nurses are recognized in many ways for their clinical expertise, leadership, and compassionate care. Formal recognition includes opportunities to serve as preceptors and committee members, support to present at internal and national conferences, and honors such as the DAISY Award, Josie King Hero Award, BEST Awards and Quality. Nurses and care teams may also be recognized through national distinctions such as the Beacon Award for Excellence, PRISM Award, and Lantern Award, as well as organizational honors including Magnet Recognition Program and NICHE.
Just as meaningful, recognition happens every day—through gratitude, from patients and families, acknowledgment from peers and leaders, and the personal pride that comes from delivering exceptional care.
At UC Davis Health, experienced nurses play a vital role in developing the next generation of professionals through mentorship, coaching, and shared expertise. New graduate nurses are supported through the Vizient/AACN Nurse Residency Program, where preceptors, clinical facilitators, and mentors guide their transition into practice. This structured support builds the knowledge, skills, and confidence needed to deliver safe, high-quality care.
Mentorship is a core expectation of professional nursing practice. Nurses actively support one another through both formal and informal relationships—sharing expertise, modeling professional behaviors, and fostering a culture of continuous learning. As careers evolve, nurses remain committed to both mentoring others and seeking mentorship to support their own growth.
The Rising Nurse Leader Program further strengthens this culture by preparing emerging leaders for future roles. Participants are paired with experienced nurse leaders who provide guidance, insight, and support in navigating the complexities of clinical and managerial leadership. These partnerships build confidence, inspire growth, and cultivate strong, connected leaders across the organization.
At UC Davis Health, nurses extend their impact beyond the organization to support healthier communities. Guided by a commitment to health equity and compassionate care, nurses engage in outreach that promotes wellness, improves access, and supports underserved populations.
These efforts include community health fairs, blood pressure and wellness screenings, vaccination clinics, school and youth education programs, and participation in local public health initiatives. Nurses also partner with community organizations to provide health education, prevention resources, and support for chronic disease management.
Through advocacy, collaboration, and volunteerism, nurses help address local health needs while strengthening trust and access to care across the region.
Community outreach is an essential part of nursing practice at UC Davis Health—connecting our values to action and improving the health of the communities we serve.
Nursing care delivery
Primary Nursing is a relationship-based care model grounded in therapeutic presence, autonomy, evidence-based practice, and collaboration. Nursing presence reflects the nurse–patient relationship in which the nurse provides holistic care, recognizing each patient as a unique individual. The model is built on the principles of responsibility, accountability, and authority, which guide nursing practice and decision-making.
We offer a wide range of resources to support high-quality, patient- and family-centered care. As part of an academic health system, nurses have access to leading-edge research, evidence-based practice, and advanced technology. Nurses collaborate with interdisciplinary experts across services such as chaplaincy, child life, pharmacy, therapy services, medicine, respiratory care, social work, and speech therapy. Nurses are also empowered to use holistic approaches, including essential oils, music therapy, pet therapy, and the HUSH (Help Us Support Healing) initiative, to enhance healing and the patient experience.
Professional Governance
Professional governance empowers clinical nurses to participate in shared decision-making related to the nursing practice environment. This includes standards of practice, policies and procedures, resource stewardship, evidence-based practice, research, and quality and performance improvement. Our System-wide along with our Practice Councils coordinate nursing activities across areas such as professional practice, education, relationship-based care, nursing excellence, technology, and quality outcomes.
Nurses at UC Davis Medical Center are transformational leaders at every level of practice. Their expertise is recognized and supported through structures that promote engagement in professional nursing practice. Nurse leaders advocate for patients, professional practice, and the resources needed to deliver safe, high-quality care. Through teamwork and collaboration, they help achieve optimal outcomes.
Exemplary professional practice
We are committed to creating an environment that supports continuous learning, growth, and professional development. We view learning as a lifelong journey—essential to advancing nursing practice and delivering high-quality care in an ever-evolving health care environment.
Professionalism reflects the knowledge, behaviors, and values that guide how nurses engage with patients, families, colleagues, and interprofessional partners. At UC Davis Health, professionalism is demonstrated through inquiry, accountability, autonomy, advocacy, innovation, collegiality, collaboration, ethics, and integrity.
These attributes create a culture of trust, respect, and teamwork—directly impacting the patient experience and strengthening the practice environment. Through peer review, nurses are supported in maintaining professional standards, setting goals, and engaging in continuous improvement. This shared accountability advances quality, reinforces professional growth, and contributes to a high-performing, supportive workforce.
UC Davis Health nurses are committed to advancing the nursing profession and contributing to the transformation of health care. In alignment with the Future of Nursing vision, nurses serve as full partners in improving care, shaping practice, and preparing the next generation.
Through academic partnerships, regional and global collaboration, and mentorship, nurses expand knowledge and influence practice beyond the organization. Participation in professional organizations and leadership roles strengthens innovation, advances quality, and supports sustainable improvements across the health care system.
We are committed to a Just Culture that promotes safety, learning, and transparency. Nurses are encouraged to report errors, near misses, and adverse events to identify system opportunities and improve care delivery.
This approach strengthens quality and safety outcomes by focusing on learning and prevention, while fostering a psychologically safe and supportive practice environment. By fairly distinguishing human error, at-risk behavior, and reckless behavior, we promote accountability, trust, and continuous improvement.
Clinical expertise is developed and sustained through ongoing professional development and specialty certification. Certification is encouraged and supported, recognizing its impact on improving patient outcomes and advancing professional practice.
By prioritizing lifelong learning, we ensure nurses are equipped to deliver safe, evidence-based, and high-quality care. This investment in expertise enhances quality outcomes, strengthens confidence and engagement, and contributes to an effective and resilient workforce.
Nurses integrate clinical expertise, patient values and preferences, and the best available evidence to guide care decisions and improve outcomes. The Iowa Model of Evidence-Based Practice supports inquiry and the consistent application of best practices.
This approach drives quality and safety, enhances the patient experience, and promotes effective, efficient care delivery—supporting both clinical excellence and responsible stewardship of resources.
When evidence is limited or unavailable, nurses engage in clinical inquiry and research to answer practice-based questions and improve care. Nurse-led research and collaboration are essential to advancing knowledge and strengthening outcomes.
Through partnerships and roles as co-investigators, nurses contribute to innovation and discovery that elevate quality, enhance patient care, and improve system performance. The UC Davis Health Center for Nursing Science supports the development and translation of research into practice, ensuring that new knowledge leads to meaningful and measurable improvements.
Outcomes
 Our PPM Compass connects our values—courage, integrity, love, and compassion—to the outcomes we strive to achieve across UC Davis Health. It provides a clear and consistent framework that ensures nursing practice is intentionally aligned with what matters most: delivering optimal outcomes for patients, families, and our teams.
Our PPM Compass connects our values—courage, integrity, love, and compassion—to the outcomes we strive to achieve across UC Davis Health. It provides a clear and consistent framework that ensures nursing practice is intentionally aligned with what matters most: delivering optimal outcomes for patients, families, and our teams.
At its foundation, our values shape how nurses engage, make decisions, and provide care. Courage empowers nurses to advocate and lead. Integrity ensures accountability and trust. Love and compassion guide meaningful connections with patients, families, and one another. These values are reflected in a professional practice that is evidence-based, relationship-centered, and grounded in clinical expertise.
Through this alignment, nursing practice directly influences our key outcome areas: people, practice, and environment; patient experience; quality; and financial stewardship. A strong and supportive practice environment fosters engagement, resilience, and teamwork. Compassionate, relationship-based care enhances the patient and family experience. A commitment to evidence-based practice drives quality and safety. Thoughtful, accountable care supports financial stewardship through effective and efficient use of resources.
By aligning what we value with how we practice, our PPM creates a clear line of sight to these outcomes. It ensures that every action, every interaction, and every decision contributes to consistent, measurable, and optimal results across the organization.


