New mouse study reveals novel tool for monitoring inflammatory load
Findings help clinicians evaluate the efficacy or resistance to therapies for inflammatory arthritis
Inflammatory arthritis describes a group of diseases caused by an overactive immune system that attacks the joints and other tissues in the body. The treatment goal for the disease is to limit pain and inflammation with medications. However, currently clinicians do not have a tool to measure inflammation in a patient’s body.
A new mouse study led by researchers at UC Davis Health has identified a model that may offer clinicians a novel tool for monitoring inflammatory load and help them evaluate the efficacy of or resistance to therapies from early stages of treatment.
The researchers presented their findings this month at the American College of Rheumatology (ACR) Annual Meeting.
“During a physical exam, the sensitivity to joint inflammation is not consistent throughout the body and we currently do not have a way quantify that inflammation,” explained Siba P. Raychaudhuri, professor of rheumatology at UC Davis Health and co-leader of the study. “This animal model provides us a clearer picture of which parts of the body are being affected by inflammation. This has allowed us to develop a tool for future use in how to determine the total inflammatory load in patients with systemic autoimmune diseases. We can also use this to monitor the disease activity in our patients with inflammatory diseases.”
This animal model provides us a clearer picture of which parts of the body are being affected by inflammation. This has allowed us to develop a tool for future use in how to determine the total inflammatory load in patients with systemic autoimmune diseases. We can also use this to monitor the disease activity in our patients with inflammatory diseases.” —Siba P. Raychaudhuri
Study methods and results
In this study, the researchers worked with mice injected with collagen-induced arthritis on day 0 and day 21 of the study. The mice then developed autoimmune arthritis around day 28.
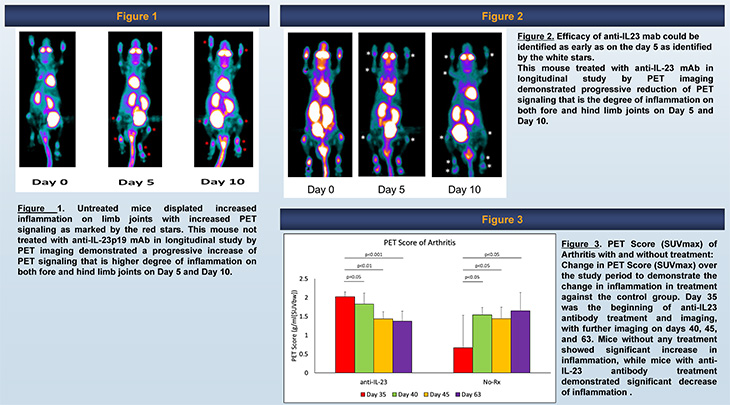
The team conducted weekly PET and CT imaging on the mice. The standardized uptake value (SUV score) of 18F-FDG, a marker for the tissue uptake of glucose, was determined for the most severe joint in each mouse to generate a comprehensive PET score (PS).
To further evaluate applications of the model to detect any changes that might occur from a therapeutic response, 15 mice were treated with mouse anti-IL-23 mab; these mice received anti-IL23 mAb weekly injections of 100ug/mouse for four weeks.
Mice were scored clinically and scanned one week after completion of the fourth dose. The mice were additionally scanned on “day 5” and on “day 10” to determine early clinical response of IL-23p19 antibody.
The clinical scores as well the PET scores for arthritis in the untreated mice gradually increased with time. Whereas the clinical scores for arthritis in the treated mice provided expected results, with clinical scores reducing over time.
“Our results confirm that the rates of the total inflammatory load can be quantified at different time points,” said Raychaudhuri. “The therapeutic treatment given to the mice provided the expected results of decreasing inflammation, allowing us to see the unique quantifiable measures of therapeutic efficacy.”
Raychaudhuri and Abhijit Chaudhari, professor of radiology, are transferring these observations to quantify the degree of inflammation in humans with systemic autoimmune diseases. For human studies, researchers are utilizing UC Davis Health's EXPLORER Total Body Scanner, which acquires PET images of the body from head to toe, all at the same time. It is the first Total Body PET scanner approved by the U.S. Food and Drug Administration.
The depth of this research underscores our divisional and departmental commitment to identify the molecular mechanisms of disease processes and develop novel therapies to treat patients suffering from these conditions.” —William Ridgway
A leader in inflammatory arthritis research
The Division of Rheumatology at UC Davis Health is among the leading centers in the country for researching inflammatory arthritis. This model for monitoring inflammatory load was one of six presentations delivered by the department at the ACR 2023 annual meeting.
Others included research on spinal inflammation, a dominant pathology in psoriatic arthritis, the regulatory role of JAK-1/TYK2 signaling on the pannus formation, and how total-body PET quantitative biomarkers reveal key differences in enthesitis between rheumatoid and psoriatic arthritis patients.
“The depth of this research underscores our divisional and departmental commitment to identify the molecular mechanisms of disease processes and develop novel therapies to treat patients suffering from these conditions,” said William Ridgway, chief of rheumatology, allergy and clinical immunology. “This type of research could potentially save lives and improve the quality of life for many individuals.”
Moving forward, the team has started extensive clinical studies to quantify the degree of inflammation in humans with rheumatoid arthritis, psoriatic arthritis and ankylosing spondylitis.
Study co-authors included Chaudhari, and Sanchita Raychaudhuri of UC Davis Health; and Christine Abria, Sneha Banerjee, Naveen Chandrasekar and Smriti K. Raychaudhuri from the Sacramento VA Medical Center