Supporting caregivers in their difficult yet critical role
For National Caregivers Day, experts discuss the challenges of caring for people with dementia or Alzheimer’s disease
Feb. 18 is National Caregivers Day, which honors individuals who provide personal care and physical and emotional support to those who need it most. More than 40 million people provide care nationwide. Their hours are long, the work is stressful and it often takes a toll on the caregiver’s health.
Below is a Q&A that addresses a wide range of issues faced by caregivers. Helen Kales is a geriatric psychiatrist and an expert in helping caregivers manage the complex care needed by people with dementia and Alzheimer’s disease. Terri Harvath is the director of the Betty Irene Moore School of Nursing Family Caregiving Institute and consults with family caregivers in the new Healthy Aging Clinic.
Caregivers can feel invisible to their family, friends and health care teams. Why is it important to acknowledge their contributions?
HARVATH: Family caregivers are the linchpin in the care for older adults. They are the ones who implement any plan of care that we have for patients when they leave our hospitals and clinics. In addition, they often have a deep understanding of how illness symptoms manifest and can detect subtle changes in condition that are clinically important. A recent study from AARP documents the complexity of care that families often provide with little to no training. To ensure families can provide safe and competent care, we must recognize the vital role they play in the care of frail, older adults and offer them the education and support they so desperately need.
What are some common misconceptions about caregiving?
KALES: Caregiving is often presented as a completely negative thing in our society. But there are a lot of studies that show caretaking has benefits. Some of it depends on what your relationship was like with the person before caretaking, but for a lot of people, it can bring families closer. There can be a lot of meaningful shared experiences, especially if you can laugh. People who can find humor in situations and are able to cope with humor generally look at caretaking more positively.
HARVATH: It is important to note that most families want to provide care to their older relatives and only relinquish that care when the person’s needs exceed what the family can provide. We don’t adequately prepare family caregivers for the complex role they take on. We need to help them understand how to detect subtle changes in the older person’s condition before it becomes a serious threat to their health. We need to teach them how to manage complex care tasks (e.g., catheters, oxygen, injections) so they feel comfortable providing care and know when to ask for more help.
If we support family caregivers and include them as both a member of the older person’s care team and a target of our interventions, we can deliver better, family-centered care in the community where most older adults prefer to remain.
Caregivers provide roughly $470 billion in unpaid assistance. Who is at risk when their health needs are not met?
HARVATH: Family caregivers often set their own health needs on the back burner because of the demands of their caregiving situation. This means that they are often sicker when they finally do seek care, adding to the illness burden they experience. This can jeopardize care for their older family member, taxing our long-term care system further with the care families can no longer provide.

What are some misconceptions about caring for people with Alzheimer’s disease or dementia?
KALES: One misconception is that people think of Alzheimer’s disease as a memory problem — which it is. However, it is much more than that. Everyone with dementia has behavioral changes. Those can include agitation, depression, aggression, hallucinations, wandering and others. Behaviors like these are the most difficult, stressful, and costly aspects of care and often cause caregivers the most stress and depression.
What are some of the underlying reasons for these behavioral changes?
KALES: Sometimes, the behavior happens because the person lacks the ability to communicate. Maybe they are hungry, thirsty, or tired, and their behavior is an expression of an unmet need. Or it could be an expression of pathologies, such as being in pain or having an infection or an injury. The change in behavior tells us that something is happening that we need to pay attention to. Rather than memory, behavior is what puts people in nursing homes, and the reason there is an overuse of psychiatric medications for people with dementia. About 70% of people with dementia are put on psychiatric medications; much of that prescribing is for sedation.
What is the DICE method? How can it help caregivers with behavioral changes?
KALES: DICE stands for describe, investigate, create and evaluate (DICE). It is designed to help caregivers take care of people with dementia, but it can be a useful technique for other caregivers. It’s very common for people with dementia to be prescribed sedating medication. The goal of DICE is to have their symptoms assessed and treated like any other symptom. For example, if you went to a doctor and said, ‘I’m short of breath,’ and the doctor immediately said, ‘you must have pneumonia,’ you would think you were going to a quack. You expect the doctor to investigate your symptoms before arriving at a conclusion. The same should be true for patients with dementia or Alzheimer’s disease.
What do you mean by “investigate” the behavior?
KALES: Say, for example, someone suddenly starts getting agitated when it’s time for a bath. Maybe it turns out they are very modest and feel uncomfortable with a new caregiver of a different gender. Or maybe the shower or bath is too hot or too cold. By describing and investigating the behavior, it’s easier to find a non-pharmacological intervention. When patients are simply sedated, the underlying problem, or pathology, won’t be revealed. More information about this method is available at the DICE website. We are also launching a national study using this method, which has been developed into an app that can be used on any smartphone, tablet or desktop device. People can find out more information about the study on the WeCareAdvisor study page.
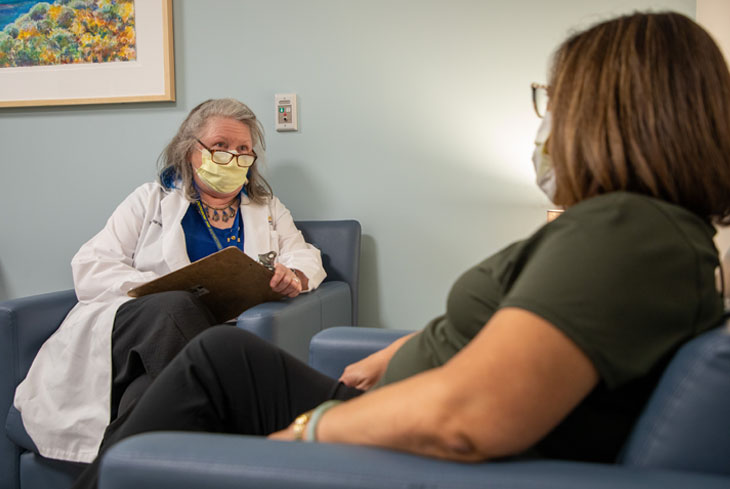
How many of the caregivers that you see at the Healthy Aging Clinic are caring for a family member with cognitive decline and how do you support them?
HARVATH: At the Family Caregiving Institute, we provide 1:1 consultation to family caregivers to better understand the challenges they face. The vast majority of the caregivers we see deal with dementia and usually two to three other chronic conditions (e.g., diabetes, hypertension). We help connect them to services they may be unaware of to ease the burden they are experiencing. In addition, we offer coaching for some of the dementia-related behavior symptoms they struggle with and offer support to try to alleviate some of the stress they experience. We also help them with some of the difficult decisions they face (e.g., can my mom keep driving? Is it time to move dad into a care setting?) to ensure they are making informed choices when safety concerns are in tension with a desire to protect autonomy and quality of life.
The pandemic has added stress for caregivers and people with dementia. Do you have any advice that might help improve mental health?
KALES: One suggestion is to make sure both of you get outside and get some sunlight. It sounds simple, but most older adults get only a fraction of the daily light that they need. Light synchronizes our circadian rhythms and improves mood and sleep, both for caregivers and people who are older. The other piece of advice is to tailor activities to what your loved one enjoys. For example, music can improve someone’s mood, but not if you don’t like that song or artist.
Any other advice for activities that help manage behavioral symptoms of dementia?
KALES: It’s good to tailor activities they like to their current abilities. For example, maybe someone liked to fish but can’t anymore. You could still have them look at a fishing magazine, watch a fishing video or organize a tackle box. Also, even if someone is physically or cognitively impaired, everybody wants to feel useful and have a sense of purpose, even it’s just tossing a salad or folding laundry. We build helping strategies like those into the DICE approach.
What is the single most important advice you have for caregivers who feel overwhelmed and undervalued?
HARVATH: I like to stress that there is often no single right way to go when caring for an older family member, especially when there is dementia in the mix. It is also important to note that we often make decisions that only provide the illusion of safety and not actual or complete safety. We certainly saw this during the pandemic when some of the nursing homes and assisted living facilities that were supposed to provide safe harbor were not always able to do so. So instead, finding the ‘best’ path forward (i.e., the path that works the best for this family at this time) often involves trial and error until they land on something that works. In finding that best path, it is important to keep quality of life and the older person’s expressed preferences in mind and not only attend to safety.
Learn more about the Family Caregiving Institute, which is dedicated to the well-being of family caregivers through education and research.
Learn more about the DICE approach and the WeCareAdvisor.





